Top videos
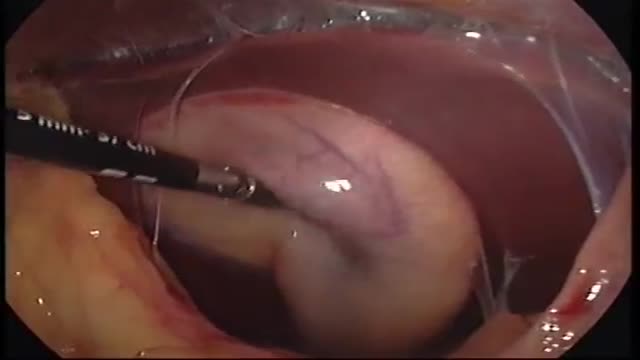
Pyogenic liver abscesses are mainly treated by percutaneous aspiration or drainage under antibiotic cover. If interventional radiology fails, surgical drainage becomes necessary. Recently, we performed laparoscopic liver abscess drainage successfully, and we aimed to focus on the topic in light of a systematic review of the literature.

Presence of abdominal pain and distension. Presence of urinary symptoms - Such as dysuria, oliguria, flank pain, and hematuria. Occurrence of any symptoms of hypocalcemia - Such as anorexia, vomiting, cramps, seizures, spasms, altered mental status, and tetany. Symptoms of hyperkalemia - Such as weakness and paralysis.
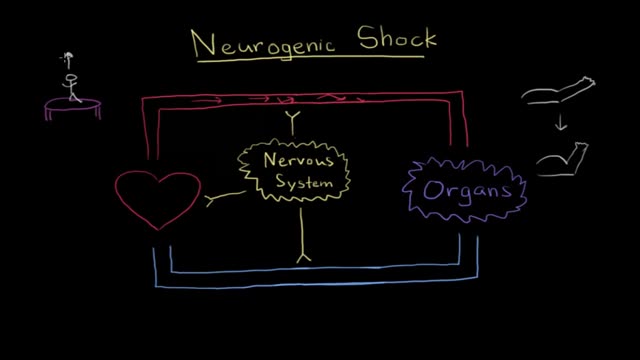
Neurogenic shock is a distributive type of shock resulting in low blood pressure, occasionally with a slowed heart rate, that is attributed to the disruption of the autonomic pathways within the spinal cord. It can occur after damage to the central nervous system such as spinal cord injury.

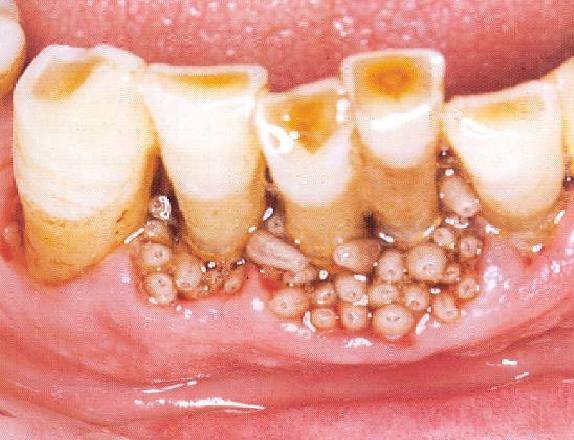
Genital warts are growths on the skin of the genital area and around the anus. They are caused by certain types of the human papilloma virus (HPV). There are more than 100 types of HPV. Some types of HPV produce warts on different parts of the body, like plantar warts on the feet and common hand warts. There is no specific treatment for HPV, but there are treatments for health problems caused by HPV. Genital warts can be treated by your healthcare provider, or with prescription medication. HPV-related cancers are more treatable when diagnosed and treated promptly. For more information, visit www.cancer.org.
Thigh pain is most often caused by injuries to bones, joints, muscles, tendons, ligaments, and other soft tissues or blood vessels. These injuries are often caused during sports competition, or strain from overuse, obesity, or pregnancy.

An MRCP scan is a scan that uses magnetic resonance imaging (MRI) to produce pictures of the liver, bile ducts, gallbladder and pancreas. Note: the information below is a general guide only. The arrangements,and the way tests are performed, may vary between different hospitals.

Rheum is made up of mucus, skin cells, oils and dust. The rheum that comes from the eyes and forms eye boogers is called gound, which you may know as eye sand, eye gunk, sleep dust, sleep sand, sleep in your eyes, or eye shnooters. When you're awake, gound doesn't cause any problems.