Top videos

From our beginnings in 1990 in primary healthcare, Healthway Medical has grown to become a respected medical group in Singapore. With over 100 clinics and medical centres, Healthway Medical has a wide network of medical centres and clinics in Singapore.
We offer comprehensive services including GP & family medicine clinics, health screening, adult specialists, baby & child specialists, dental services and allied healthcare services.

If you’re wondering ‘what’s the cause of my knee pain?’ or ‘what kind of knee pain do I have?’ the position of your knee pain can often tell you what type of knee pain you have.
You confirm this if you know the common symptoms an aggravations for each type of knee problem. So if you want to know ‘why my knee hurts’... here’s a quick look at the most common type of knee problems...
Patellofemoral Pain Syndrome (Or Runner’s Knee) (Old Name: Chondromalacia Patellae)
Infrapatellar Fat Pad Syndrome (Hoffa's Syndrome)
Patella Tendonitis (Jumper’s Knee)
Prepatellar Bursitis
Osgood-Schlatter Disease
Meniscus Tear
Medial Collateral Ligament Tear
Osteoarthritic Knee Pain
Pes Anserine Bursitis.
Iliotibial Band Syndrome
Quadriceps Tendinopathy
Popliteus Strain
Baker’s Cyst
ACL Or PCL Tear/Rupture
---------------------------------------
Check out my channel...
https://youtube.com/@BodyFixExercises
OTHER VIDEOS:
How To Fix Pain In The Front Of The Knee… (Runner's Knee) https://youtu.be/g0qmx_0enAA
Knee Strengthening Exercises To Prevent Knee Pain
https://youtu.be/Pk-ae_lyx7M
How To Treat Patellar Tendinopathy (Jumper’s Knee) & Quadriceps Tendinopathy
https://youtu.be/MkPwsb-rQwU
---------------------------------------
#bodyfixexercises #kneepainrelief #kneepain
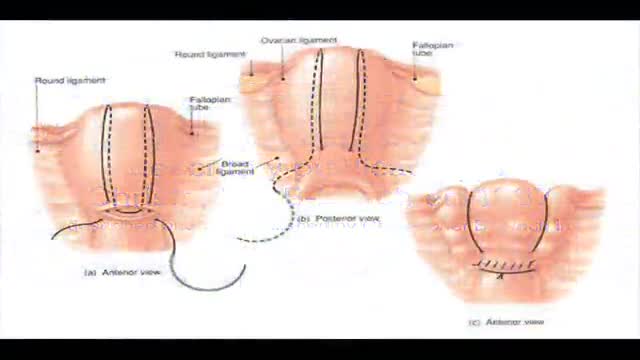
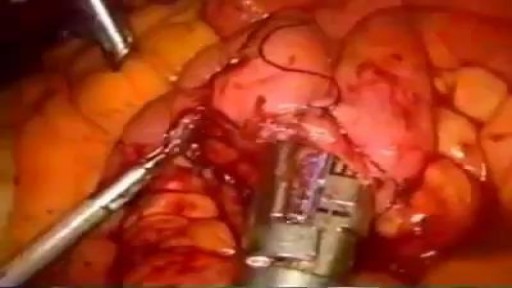
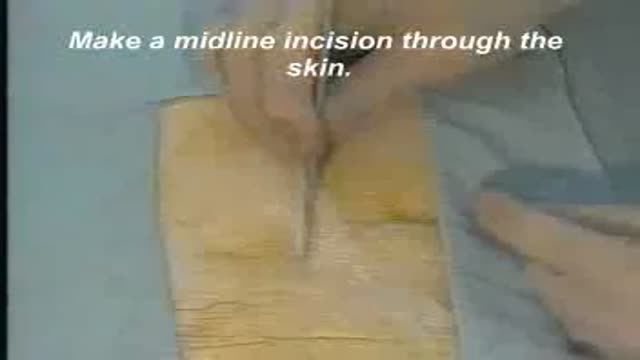
Not every woman undergoes a traditional vaginal delivery with the birth of her child. Under conditions of fetal or maternal distress, or in the case of breech presentation (when a baby is turned feet first at the time of delivery), or if the woman’s first baby was born by cesarean delivery, a procedure called a cesarean section may be required. During a cesarean, a doctor will make either a lateral incision in the skin just above the pubic hair line, or a vertical incision below the navel. As the incision is made, blood vessels are cauterized to slow bleeding. After cutting through the skin, fat, and muscle of the abdomen, the membrane that covers the internal organs is opened, exposing the bladder and uterus. At this time the physician will generally insert his or her hands into the pelvis in order to determine the position of the baby and the placenta. Next, an incision is made into the uterus and any remaining fluids are suctioned from the uterus. The doctor then enlarges the incision with his or her fingers. The baby’s head is then grasped and gently pulled with the rest of its body from the mother’s uterus. Finally, the abdominal layers are sewn together in the reverse order that they were cut. The mother is allowed to recover for approximately three to five days in the hospital. She will also be quite sore and restricted from activity for the following several weeks. There are several potential complications associated with this procedure that should be discussed with a doctor prior to surgery.

Synthol, otherwise known as site enhancement oil is used by some people (including bodybuilders) to increase the apparent size of their muscles by directly injecting the oil into their muscle tissue. Users treat it as a short cut of looking like a body builder, without the actual hard work of bodybuilding training. With repeated injections, a larger volume of synthol builds up inside the muscle, expanding its size like a balloon filling up with air. Side effects of synthol can cause nerve damage, stroke, ulcers, pulmonary embolisms, and much more. Injecting synthol is very dangerous and if that doesn’t deter potential users, there is also a problem from an aesthetic standpoint; synthol use makes ones body look deformed (just see for yourself in the pictures below).