Top videos

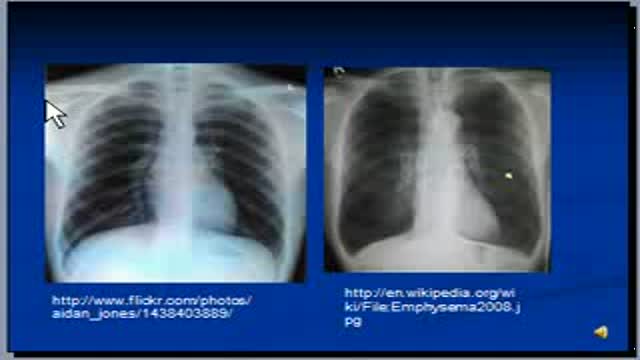
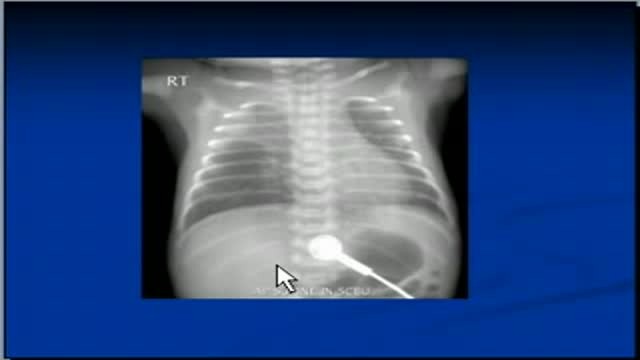
Marfan syndrome is a genetic disorder that affects the body's connective tissue. Connective tissue holds all the body's cells, organs and tissue together. It also plays an important role in helping the body grow and develop properly. Connective tissue is made up of proteins.
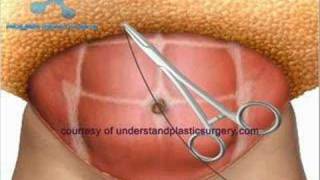
http://www.bodysculptor.com. Dr. Otto Placik, Board Certified Chicago based plastic surgeon demonstrates the results of a muscle separation(rectus diastasis) repair using 3 dimesional CAT scan and photographic images

If you use condoms perfectly every single time you have sex, they’re 98% effective at preventing pregnancy. But people aren’t perfect, so in real life condoms are about 85% effective — that means about 15 out of 100 people who use condoms as their only birth control method will get pregnant each year.
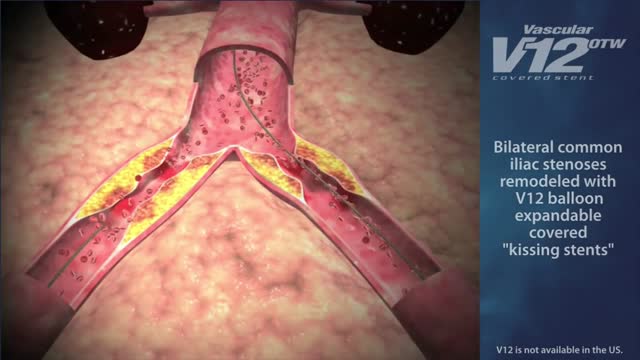
Indications for endovascular repair of the iliac artery are: Stenosis or (short-segment) occlusion of iliac artery (TASC type A and B, TASC C lesions are controversial) with ipsilateral lower extremity ischemia (lifestyle-limiting, progressive claudication, rest pain, gangrene). Patients with asymptomatic aneurysm greater than 4 cm in diameter. An iliac aneurysm which has also increased in size by 0.5 cm in last six months. Symptomatic iliac artery aneurysms mandate endovascular (or open) repair regardless of size. Patients with long occluded lesions/poor run-off/acute limb ischemia are poor endovascular candidates.

Don't let your wrinkles reveal your age. Get rid of ageing lines with botox. Book your appointment, Call at +918939636222, +9189398 81919. For more visit - https://www.dermatologistchennai.in/anti-aging-treatment-in-nungambakkam.php

Have you heard any medical lingo you've thought is strange? Funny healthcare speaker Dr. Brad Nieder discusses funny medical terminology he's learned in his medical career. He brings his medical comedy to a healthcare conference, describing how he didn't know what "stat" meant.
He goes on about how he thought up many funny terms he could say in return to the doctor who introduced him to the word. His healthcare comedy makes the crowd burst with laughter.
Dr. Brad knows how to adapt his hilarious real-life stories into customized presentations for any in-person or virtual event. Watch more of his videos as a medical comedian and all-around funny guy by browsing his videos.

Pancreatic cysts are saclike pockets of fluid on or in your pancreas, a large organ behind the stomach that produces hormones and enzymes that help digest food. Most pancreatic cysts aren't cancerous, and many don't cause symptoms. They're typically found during imaging testing for another problem. Some are actually noncancerous (benign) pockets of fluids lined with scar or inflammatory tissue, not the type of cells found in true cysts (pseudocysts). But some pancreatic cysts can be or can become cancerous. Your doctor might take a sample of the pancreatic cyst fluid to determine if cancer cells are present. Or your doctor might recommend monitoring a cyst over time for changes that indicate cancer.
Corneal cross-linking (CXL) is an in-office eye procedure that strengthens the cornea if it's been weakened by keratoconus, other corneal disease, or (rarely) a complication of LASIK surgery. Alternative and brand names for the procedure include corneal cross-linking, corneal collagen cross-linking, C3-R, CCL and KXL.

Bacterial meningitis is very serious and can be deadly. Death can occur in as little as a few hours. While most people with meningitis recover, permanent disabilities such as brain damage, hearing loss, and learning disabilities can result from the infection. There are several types of bacteria that can cause meningitis. Some of the leading causes of bacterial meningitis in the United States include Streptococcus pneumoniae, group B Streptococcus, Neisseria meningitidis, Haemophilus influenzae, and Listeria monocytogenes.

An abscess is a collection of pus. Pus is a thick fluid that usually contains white blood cells, dead tissue and germs (bacteria). The usual cause of an abscess is an infection with bacteria. Certain bacteria are more likely to be 'pus-forming' as they make chemicals (toxins) that can damage the body's tissues.

Commentary:
0:24
He may not look like he’s in good condition but you can guesst that his somewhere in nirvana at this point
0:44
After the operation, this patient loses more than just color in his skin but apparently he loses his nipples as well
1:43
This sedated patient is equipped with his own hand-gun. No pun intended
2:17
His anesthesia dose came with the usual side effects of crazy talk with a dash of attitude and sarcasm
3:17
The only thing crazier than love is being sedated during an endometriosis surgery
4:36
This may come as a surprise to some but penguins don’t actually reside in Alaska. In case you didn’t know that well now you do
5:09
If the doctor advises you against something you can’t resist doing, how many of us would still listen to him?
6:35
When them meds start kicking in , it’s time to frame this experience as an excuse to divulge some of your secret fantasies
7:05
There’s a time and place dirty jokes but anesthesia told this guy any times the right time
7:24
Her 16 year old son talks about the last thing he remembers right after surgery and this is what he says
8:35
She’s definitely not in the mood at all. I wouldn’t wanna tick her off during this time if I were you
8:44
A feeling of relief after your operation may be followed by some emotional changes such as mood swings and over sensitivity
9:44
Even if you do say something you wouldn't normally say while you are under sedation, according to some doctors, “it's always kept within the operating room”
10:38
The beeping sounds of the medical equipments tip this patient over the edge. so she tries to drown out the noise with her own voice
11:08
Anyone who's received anesthesia can attest to feeling pretty loopy. Although many won't remember it's fairly common to say some wacky things after waking up
11:53
It's typical for people to feel sad or vulnerable after surgery. Kind of like how this girl is feeling right now
12:04
If she wasn’t under the influence in the hospital right now , it would be pretty hard to justify this type of behavior
12:17
Imagine working as an anesthesiologist. You might become numb to a lot of strange behaviors and everything unusual becomes the new norm for you
► Subscribe: https://bit.ly/3I4zXBT
Top Special Videos: https://bit.ly/3o64YOa
Acts Of Kindness: https://bit.ly/3E5FmXh
Try Not To Laugh Videos: https://bit.ly/3leRpdl
Social media:
► INSTAGRAM: https://www.instagram.com/topthings.tt/
► FACEBOOK: https://www.facebook.com/TopTh....ings-108385027422972
► TWITTER: https://twitter.com/TopThings10
► YOUTUBE: https://www.youtube.com/channe....l/UCArcrGQYzJhB_IfEl
#funnyvideos #anesthesia #anesthesiareactions