Top videos

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.

In breastfeeding, the latch is the moment everything comes together: Your baby takes a big mouthful of your nipple and areola (or "latches on"), begins to suck, and draws out your milk. When your baby has established a good latch, your nipple soreness is minimized and your little one gets the nourishment he needs. How do you pull all that off? First and most important, have faith in yourself and your baby. "Babies are designed to breastfeed," says Emily Pease, R.N., international board certified lactation consultant (IBCLC), of Swedish Hospital's Breastfeeding Center in Seattle. "They are born with instincts that help them find Mom's breast and latch on often with very little assistance. And if problems do come up, there are lots of ways to troubleshoot." Here are more steps to get a good latch right from the start.

Folic acid, which is also called folate, is a B vitamin. The best food sources of folic acid are fortified cereals. Folic acid plays an important role in the production of red blood cells and helps your baby's neural tube develop into her brain and spinal cord.
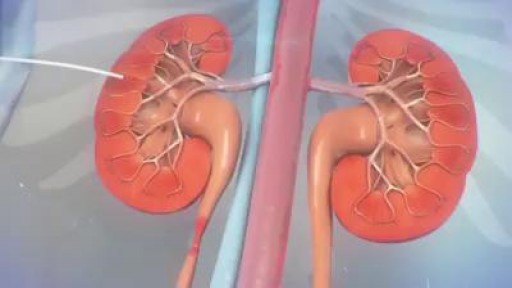
The ureter can become obstructed due to conditions such as kidney stones, tumors, infection, or blood clots. When this happens, physicians can use image guidance to place stents or tubes in the ureter to restore the flow of urine to the bladder. A ureteral stent is a thin, flexible tube threaded into the ureter.

Ultrasound or ultrasonography is a medical imaging technique that uses high frequency sound waves and their echoes. The technique is similar to the echolocation used by bats, whales and dolphins, as well as SONAR used by submarines. In ultrasound, the following events happen: The ultrasound machine transmits high-frequency (1 to 5 megahertz) sound pulses into your body using a probe. The sound waves travel into your body and hit a boundary between tissues (e.g. between fluid and soft tissue, soft tissue and bone). Some of the sound waves get reflected back to the probe, while some travel on further until they reach another boundary and get reflected. The reflected waves are picked up by the probe and relayed to the machine. The machine calculates the distance from the probe to the tissue or organ (boundaries) using the speed of sound in tissue (5,005 ft/s or1,540 m/s) and the time of the each echo's return (usually on the order of millionths of a second). The machine displays the distances and intensities of the echoes on the screen, forming a two dimensional image like the one shown below.
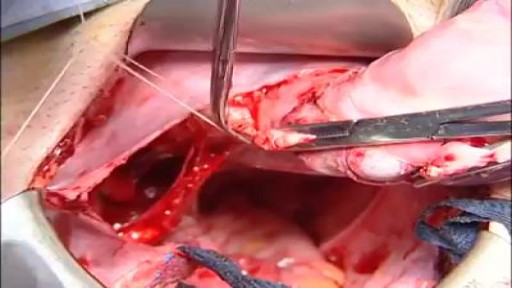
An abdominal hysterectomy is a surgical procedure that removes your uterus through an incision in your lower abdomen. Your uterus — or womb — is where a baby grows if you're pregnant. A partial hysterectomy removes just the uterus, leaving the cervix intact. A total hysterectomy removes the uterus and the cervix. Sometimes a hysterectomy includes removal of one or both ovaries and fallopian tubes, a procedure called a total hysterectomy with salpingo-oophorectomy (sal-ping-go-o-of-uh-REK-tuh-me). A hysterectomy can also be performed through an incision in the vagina (vaginal hysterectomy) or by a laparoscopic or robotic surgical approach — which uses long, thin instruments passed through small abdominal incisions.

An esophageal stent is a flexible mesh tube, approximately 2cm (3/4 inch) wide, and is placed through the constricted area of your esophagus (food tube) to allow food and beverages to pass from your mouth to your stomach for digestion and absorption of nutrients.
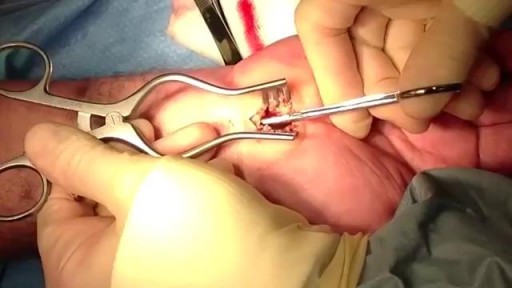
Carpal tunnel release is a surgery used to treat and potentially heal the painful condition known as carpal tunnel syndrome. Doctors used to think that carpal tunnel syndrome was caused by an overuse injury or a repetitive motion performed by the wrist or hand, often at work. They now know that it’s most likely a congenital predisposition (something that runs in families) – some people simply have smaller carpal tunnels than others. Carpal tunnel syndrome can also be caused by injury, such as a sprain or fracture, or repetitive use of a vibrating tool. It's also been linked to pregnancy, diabetes, thyroid disease, and rheumatoid arthritis.