Top videos

Have you heard any medical lingo you've thought is strange? Funny healthcare speaker Dr. Brad Nieder discusses funny medical terminology he's learned in his medical career. He brings his medical comedy to a healthcare conference, describing how he didn't know what "stat" meant.
He goes on about how he thought up many funny terms he could say in return to the doctor who introduced him to the word. His healthcare comedy makes the crowd burst with laughter.
Dr. Brad knows how to adapt his hilarious real-life stories into customized presentations for any in-person or virtual event. Watch more of his videos as a medical comedian and all-around funny guy by browsing his videos.

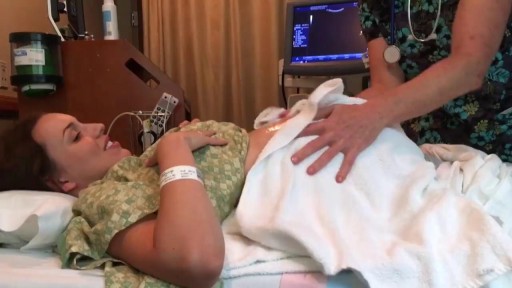
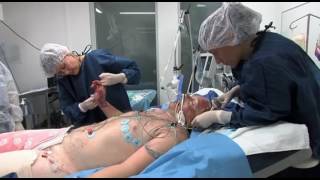
If you’ve lost a significant amount of weight, either after pregnancy or through exercise and dietary changes, excess skin and weakened abdominal muscles can leave you self-conscious about your appearance. In this video, Dr. Catherine Hannan and Dr. Lauren Patrick, two of our Board-Certified Plastic Surgeons, are performing a Tummy Tuck (Abdominoplasty) surgery. Tummy Tuck surgery gets rid of the excess skin, as well as tightens your abdominal muscles, resulting in a flatter and smoother abdomen. The results of the surgery are permanent except in cases of large weight gain or pregnancy after surgery.
We are so excited to have taken a part in our patient's body transformation journey!
Before & After Gallery:
https://www.westendplasticsurg....ery.com/surgical/bod
To learn more, visit our website or call (202) 785-4187
http://www.westendplasticsurgery.com
~~~~~~~~~~~~~~~~~~~
Social Media:
✨ Instagram: http://www.instagram.com/westendplasticsurgery
✨ Facebook: http://www.facebook.com/westendplasticsurgery
✨ Twitter: http://www.twitter.com/weplasticsurg
✨ Blog: https://www.westendplasticsurgery.com/blog
✨ Business Inquiries: info@westendplasticsurgery.com
~~~~~~~~~~~~~~~~~~~
#TummyTuck #Abdominoplasty
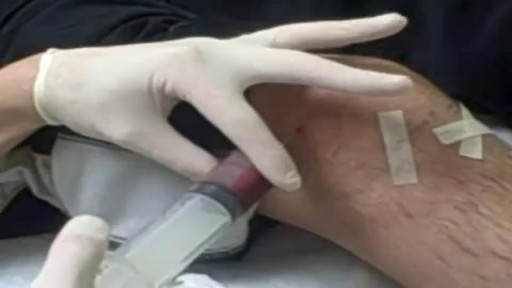
nee joint aspiration and injection are performed to aid in diagnosis and treatment of knee joint diseases. The knee joint is the most common and the easiest joint for the physician to aspirate. One approach involves insertion of a needle 1 cm above and 1 cm lateral to the superior lateral aspect of the patella at a 45-degree angle. Once the needle has been inserted 1 to 1½ inches, aspiration aided by local compression is performed. Local corticosteroid injections can provide significant relief and often ameliorate acute exacerbations of knee osteoarthritis associated with significant effusions. Among the indications for arthrocentesis are crystal-induced arthropathy, hemarthrosis, unexplained joint effusion, and symptomatic relief of a large effusion. Contraindications include bacteremia, inaccessible joints, joint prosthesis, and overlying infection in the soft tissue. Large effusions can recur and may require repeat aspiration. Anti-inflammatory medi
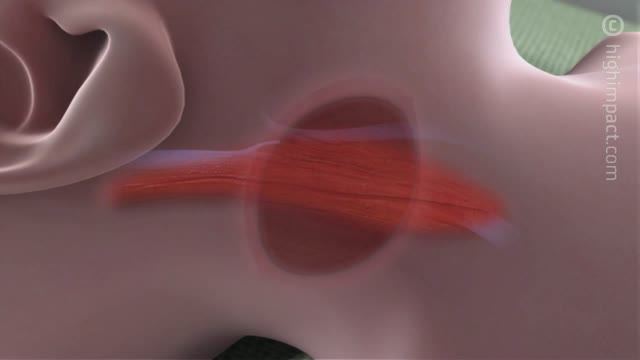
Central catheters provide dependable intravenous access and enable hemodynamic monitoring and blood sampling [1-3]. The jugular veins are one of the most popular sites for central venous access due to accessibility and overall low complication rates, and are the preferred site for temporary hemodialysis.
Corneal cross-linking (CXL) is an in-office eye procedure that strengthens the cornea if it's been weakened by keratoconus, other corneal disease, or (rarely) a complication of LASIK surgery. Alternative and brand names for the procedure include corneal cross-linking, corneal collagen cross-linking, C3-R, CCL and KXL.

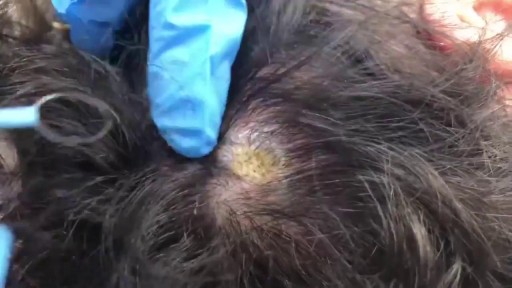
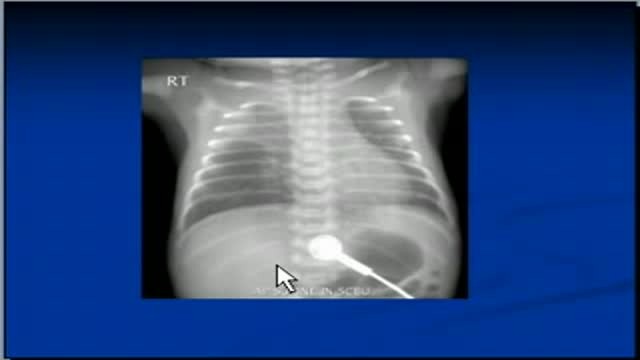
Bacterial meningitis is very serious and can be deadly. Death can occur in as little as a few hours. While most people with meningitis recover, permanent disabilities such as brain damage, hearing loss, and learning disabilities can result from the infection. There are several types of bacteria that can cause meningitis. Some of the leading causes of bacterial meningitis in the United States include Streptococcus pneumoniae, group B Streptococcus, Neisseria meningitidis, Haemophilus influenzae, and Listeria monocytogenes.

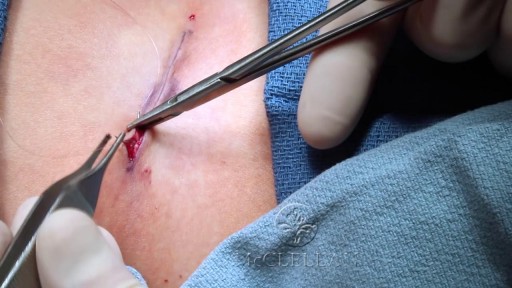
Lattrell Wells was a perfect candidate for the MACI procedure. Dr. Michael O'Malley is a sports medicine surgeon at Carilion Clinic, "It’s a two stage procedure. So what we do is we actually harvest a small portion of the patient's cartilage and bone cells and we send it to a lab where the lab then that grows additional cartilage cells. It comes back to us in a little sheet and six weeks after that initial surgery, we re-implant the cartilage in a second surgery where we implant that sheet depending on the size of lesion right where his defect. This the only option where there’s virtually no risk of any kind of graft rejection or anything of that nature.