Top videos

Folic acid, which is also called folate, is a B vitamin. The best food sources of folic acid are fortified cereals. Folic acid plays an important role in the production of red blood cells and helps your baby's neural tube develop into her brain and spinal cord.
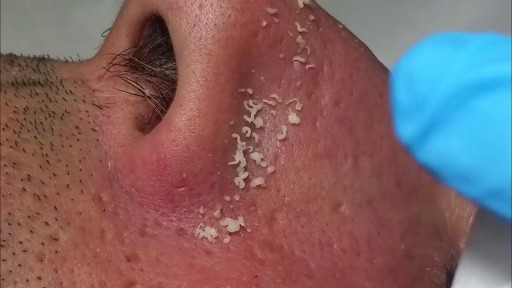
What are blackheads? Blackheads are small bumps that appear on your skin due to clogged hair follicles. These bumps are called blackheads because the surface looks dark or black. Blackheads are a mild type of acne that usually form on the face, but they can also appear on the following body parts: back chest neck arms shoulders Acne affects nearly 50 million Americans and is the most common skin disorder in the United States, according to the American Academy of Dermatology. What do blackheads look like? What causes blackheads? Blackheads form when a clog or plug develops in the opening of hair follicles in your skin. Each follicle contains one hair and a sebaceous gland that produces oil. This oil, called sebum, helps keep your skin soft. Dead skin cells and oils collect in the opening to the skin follicle, producing a bump called a comedo. If the skin over the bump stays closed, the bump is called a whitehead. When the skin over the bump opens, exposure to the air causes it to look black and a blackhead forms. Some factors can increase your chances of developing acne and blackheads, including: producing too much body oil the buildup of the Propionibacterium acnes bacteria on the skin irritation of the hair follicles when dead skins cells don’t shed on a regular basis undergoing hormonal changes that cause an increase in oil production during the teen years, during menstruation, or while taking birth control pills taking certain drugs, such as corticosteroids, lithium, or androgens Some people believe that what you eat or drink can affect acne. Dairy products and foods that increase blood sugar levels, such as carbohydrates, may play a part in triggering acne, but researchers aren’t convinced that there’s a strong connection. ADVERTISING What are symptoms of blackheads? Because of their dark color, blackheads are easy to spot on the skin. They’re slightly raised, although they aren’t painful because they aren’t inflamed like pimples. Pimples form when bacteria invade the blockage in the hair follicle, causing redness and inflammation. How are blackheads treated? Over-the-counter (OTC) treatments Many acne medications are available at drug and grocery stores and online without a prescription. These medications are available in cream, gel, and pad form and are put directly on your skin. The drugs contain ingredients such as salicylic acid, benzoyl peroxide, and resorcinol. They work by killing bacteria, drying excess oil, and forcing the skin to shed dead skin cells. Prescription medications If OTC treatment doesn’t improve your acne, your doctor may suggest that you use stronger prescription medications. Medications that contain vitamin A keep plugs from forming in the hair follicles and promote more rapid turnover of skin cells. These medications are applied directly to your skin and can include tretinoin, tazarotene, or adapalene. Your doctor may also prescribe another type of topical medication that contains benzoyl peroxide and antibiotics. If you have pimples or acne cysts in addition to your blackheads, this type of medication may be particularly helpful. Manual removal Dermatologists or specially trained skin care professionals use a special instrument called a round loop extractor to remove the plug causing the blackhead. After a small opening is made in the plug, the doctor applies pressure with the extractor to remove the clog. Microdermabrasion During microdermabrasion, a doctor or skin care professional uses a special instrument that contains a rough surface to sand the top layers of your skin. Sanding the skin removes clogs that cause blackheads. Chemical peels Chemical peels also remove clogs and get rid of the dead skins cells that contribute to blackheads. During a peel, a strong chemical solution is applied to the skin. Over time, the top layers of the skin peel off, revealing smoother skin underneath. Mild peels are available over the counter, while stronger peels are performed by dermatologists or other skincare professionals. Laser and light therapy Laser and light therapies use tiny beams of intense light to decrease oil production or kill bacteria. Both lasers and light beams reach below the surface of the skin to treat blackheads and acne without damaging the top layers of the skin. How can blackheads be prevented? You can prevent blackheads without spending a lot of money by trying a few of the following ideas: Wash regularly Wash your face when you wake up and before you go to bed to remove oil buildup. Washing more than twice each day can irritate your skin and make your acne worse. Use a gentle cleanser that doesn’t make your skin red or irritated. Some acne cleansing products have antibacterial ingredients that kill P. acnes bacteria. Consider washing your hair every day, too, particularly if it’s oily. Hair oils can contribute to clogged pores. It’s also important to wash your face after you eat oily foods such as pizza, because oil from these foods can clog pores. Use oil-free products Any product that contains oil can contribute to new blackheads. Choose oil-free or noncomedogenic makeup, lotions, and sunscreens to avoid making your problem worse. Try an exfoliating product Exfoliating scrubs and masks remove dead skin cells from your face and can help reduce blackheads. Look for products that don’t irritate your skin.
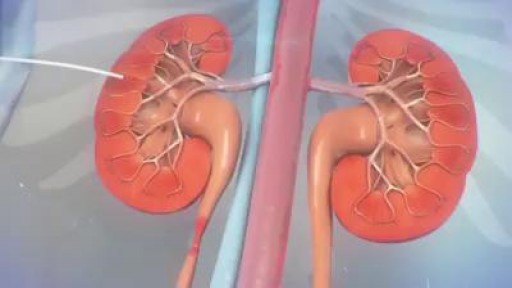
The ureter can become obstructed due to conditions such as kidney stones, tumors, infection, or blood clots. When this happens, physicians can use image guidance to place stents or tubes in the ureter to restore the flow of urine to the bladder. A ureteral stent is a thin, flexible tube threaded into the ureter.
A central venous catheter (CVC), also known as a central line, central venous line, or central venous access catheter, is a catheter placed into a large vein. Catheters can be placed in veins in the neck (internal jugular vein), chest (subclavian vein or axillary vein), groin (femoral vein), or through veins in the arms (also known as a PICC line, or peripherally inserted central catheters). It is used to administer medication or fluids that are unable to be taken by mouth or would harm a smaller peripheral vein, obtain blood tests (specifically the "central venous oxygen saturation"), and measure central venous pressure.
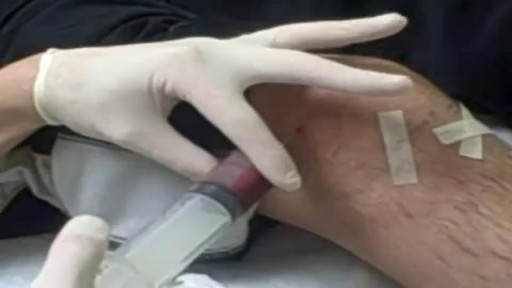
nee joint aspiration and injection are performed to aid in diagnosis and treatment of knee joint diseases. The knee joint is the most common and the easiest joint for the physician to aspirate. One approach involves insertion of a needle 1 cm above and 1 cm lateral to the superior lateral aspect of the patella at a 45-degree angle. Once the needle has been inserted 1 to 1½ inches, aspiration aided by local compression is performed. Local corticosteroid injections can provide significant relief and often ameliorate acute exacerbations of knee osteoarthritis associated with significant effusions. Among the indications for arthrocentesis are crystal-induced arthropathy, hemarthrosis, unexplained joint effusion, and symptomatic relief of a large effusion. Contraindications include bacteremia, inaccessible joints, joint prosthesis, and overlying infection in the soft tissue. Large effusions can recur and may require repeat aspiration. Anti-inflammatory medi

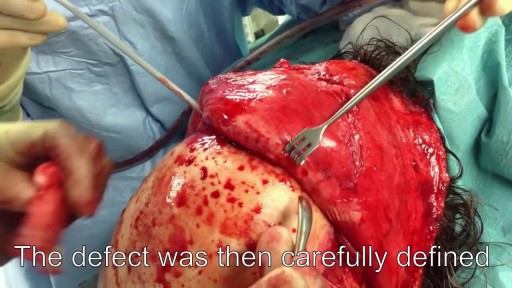
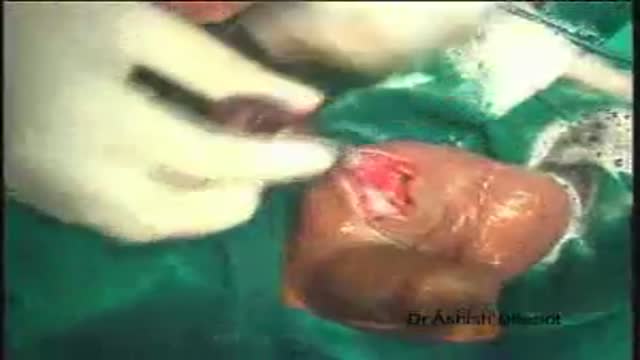
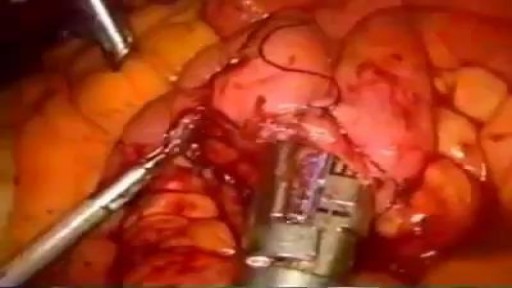
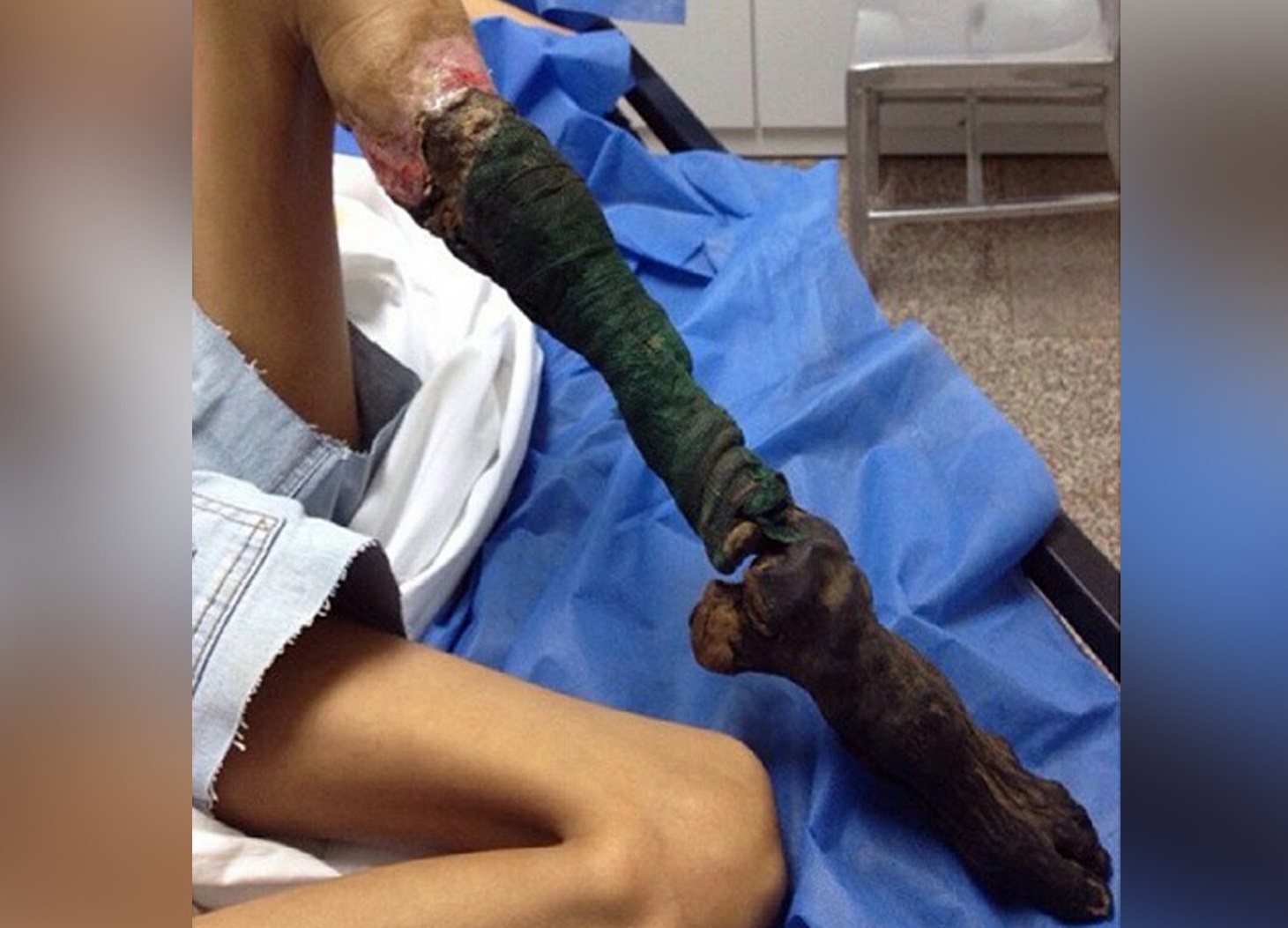
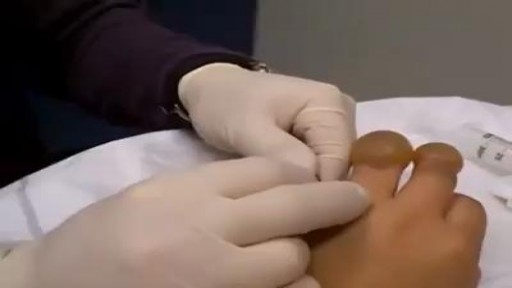
In this video a real case of the extremely rare disease "Fibrodysplasia ossificans progressiva" or what is called the "FOP" This disease is commonly misdiagnosed and usually end up by unnecessary surgery which exaggerate the disease. Children born with FOP characteristically have deformed great toes, possibly missing a joint or simply presenting with a notable lump at the minor joint. The first "flare-up" that leads to the formation of FOP bones usually occurs before the age of 10. FOP is a genetic disease. The bone growth progresses from the top downward, just as bones grow in fetuses. A child with FOP will typically develop bones starting at the neck, then on the shoulders, arms, chest area and finally on the feet. However it does not necessarily occur in this order due to injury-caused flare-ups. Often, the tumor-like lumps that characterize the disease appear suddenly. The gene that causes ossification is normally deactivated after a fetus' bones are formed in the womb, but in patients with FOP, the gene keeps working. Aberrant bone formation in patients with FOP occurs when injured connective tissue or muscle cells at the sites of injury or growth incorrectly express an enzyme for bone repair during apoptosis (self-regulated cell death), resulting in lymphocytes containing excess bone morphogenetic protein 4 (BMP4) provided during the immune system response. Since the incorrect enzyme remains unresolved within the immune response, the body continues providing the incorrect BMP4-containing lymphocytes. BMP4 is a product that contributes to the development of the skeleton in the normal embryo.

A man's age matters. As men get older, the chances of conceiving and having a healthy child decline. Male fertility starts to decline after 40 when sperm quality decreases. This means it takes longer for their partners to conceive and when they do, there's an increased risk of miscarriage.
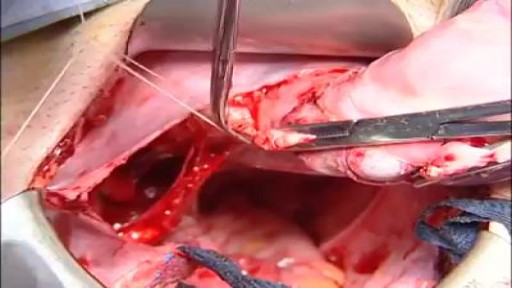
An abdominal hysterectomy is a surgical procedure that removes your uterus through an incision in your lower abdomen. Your uterus — or womb — is where a baby grows if you're pregnant. A partial hysterectomy removes just the uterus, leaving the cervix intact. A total hysterectomy removes the uterus and the cervix. Sometimes a hysterectomy includes removal of one or both ovaries and fallopian tubes, a procedure called a total hysterectomy with salpingo-oophorectomy (sal-ping-go-o-of-uh-REK-tuh-me). A hysterectomy can also be performed through an incision in the vagina (vaginal hysterectomy) or by a laparoscopic or robotic surgical approach — which uses long, thin instruments passed through small abdominal incisions.
Frostbite is an injury caused by freezing of the skin and underlying tissues. First your skin becomes very cold and red, then numb, hard and pale. Frostbite is most common on the fingers, toes, nose, ears, cheeks and chin. Exposed skin in cold, windy weather is most vulnerable to frostbite. But frostbite can occur on skin covered by gloves or other clothing. Frostnip, the first stage of frostbite, doesn't cause permanent skin damage. You can treat very mild frostbite with first-aid measures, including rewarming your skin. All other frostbite requires medical attention because it can damage skin, tissues, muscle and bones. Possible complications of severe frostbite include infection and nerve damage.

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.

Lip augmentation is a cosmetic procedure that can give you fuller, plumper lips. These days, an injectable dermal filler is the most commonly used method of lip augmentation. There are many types of dermal fillers that can be injected in your lips and around your mouth.

A brief description of the pathophysiology, clinical features, warning signs, diagnosis and management of Dengue fever. This description is based on the World Health Organisation guidelines of the management of Dengue fever.
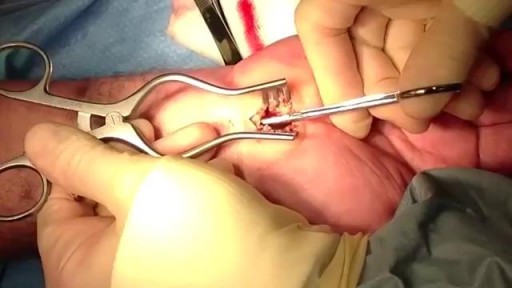
Carpal tunnel release is a surgery used to treat and potentially heal the painful condition known as carpal tunnel syndrome. Doctors used to think that carpal tunnel syndrome was caused by an overuse injury or a repetitive motion performed by the wrist or hand, often at work. They now know that it’s most likely a congenital predisposition (something that runs in families) – some people simply have smaller carpal tunnels than others. Carpal tunnel syndrome can also be caused by injury, such as a sprain or fracture, or repetitive use of a vibrating tool. It's also been linked to pregnancy, diabetes, thyroid disease, and rheumatoid arthritis.
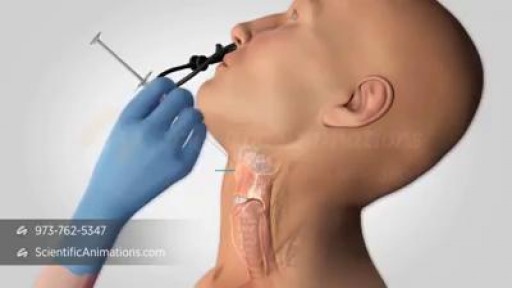
The voice box, or larynx, has three important functions. It is necessary for breathing, voice and swallowing. The vocal folds have two positions, open (apart) for breathing (picture I) and closed (together) for making sound, coughing and sealing off the lungs when swallowing (picture II). When one of the vocal folds are paralyzed, it usually rests in an in-between position (picture III), and neither opens for breathing, nor closes for voicing, coughing, or swallowing. Usually, the effects on the voice are the most dramatic. The voice becomes weak and breathy. People can only say a few words per breath, and are frequently out-of-breath, or physically tired when trying to speak for more than a few minutes straight. The voice may also get somewhat high and squeaky, with a diminished range. Swallowing may be affected as well, where you may notice some choking or coughing with certain liquids. Your cough is frequently different and very weak. This is a serious problem for patients with with vocal fold paralysis because one of the most important functions of the larynx is to keep liquids out of the lungs, and to be able to cough up mucus. When this does not happen, you are at risk for getting an "aspiration" pneumonia. The surgical procedure to restore these important functions is called "medialization laryngoplasty"