Top videos
Types of multiple myeloma. Multiple myeloma is the most common type of plasma cell cancer. The bones and bone marrow are the main sites where myeloma cells (abnormal plasma cells) are produced. The myeloma cells can form tumours, called plasmacytomas, in many bones in the body.

According to a recent study, most people's sexual romps last about 1.5–7 minutes. But, as Dr. Harry Fisch writes in his new book The New Naked: The Ultimate Sex Education for Grownups, 45 percent of men come in two minutes or less, leaving their female partners orgasmless. Here are some ways to extend your man's sexual stamina, and more likely have an orgasm yourself in the process.
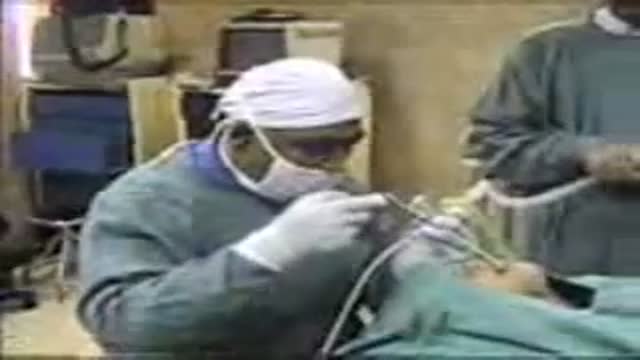
Foreign Body(FB) Airway (Whistle) was inhailed by a child causing intermitent stridor & respiratory distress.FForeign Body was removed successfully by rigid endoscopy under General Anesthesia (G/A).The relevant steps of procedure are shown
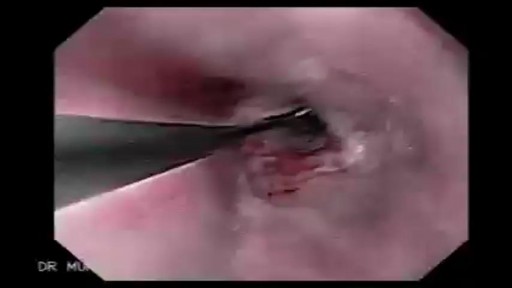
What is Esophageal Dilation?Esophageal dilation is a procedure that allows your doctor to dilate, or stretch, a narrowed area of your esophagus [swallowing tube]. Doctors can use various techniques for this procedure. Your doctor might perform the procedure as part of a sedated endoscopy. Alternatively, your doctor might apply a local anesthetic spray to the back of your throat and then pass a weighted dilator through your mouth and into your esophagus. Why is it Done? The most common cause of narrowing of the esophagus, or stricture, is scarring of the esophagus from reflux of acid occurring in patients with heartburn.

What is peripheral neuropathy? Your peripheral nervous system connects the nerves from your brain and spinal cord, or central nervous system, to the rest of your body. This includes your: arms hands feet legs internal organs mouth face The job of these nerves is to deliver signals about physical sensations back to your brain.
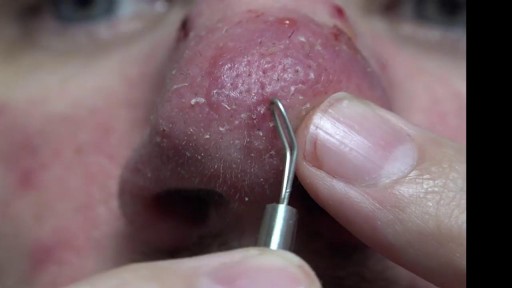
Cystic acne is a severe type of acne in which the pores in the skin become blocked, leading to infection and inflammation. The skin condition mainly affects the face, but also often affects the upper trunk and upper arms. Acne most often affects adolescents and young adults, with an estimated 80 percent of people between 11 and 30 years of age experiencing acne at some point. Cystic acne is the most severe form and affects far fewer people. In 2009, the Centers for Disease Control and Prevention (CDC) found that acne was the top reason people gave for visiting a dermatologist.

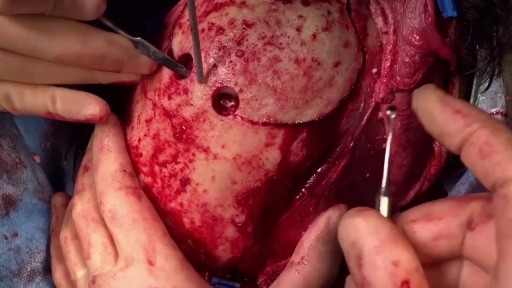
Lattrell Wells was a perfect candidate for the MACI procedure. Dr. Michael O'Malley is a sports medicine surgeon at Carilion Clinic, "It’s a two stage procedure. So what we do is we actually harvest a small portion of the patient's cartilage and bone cells and we send it to a lab where the lab then that grows additional cartilage cells. It comes back to us in a little sheet and six weeks after that initial surgery, we re-implant the cartilage in a second surgery where we implant that sheet depending on the size of lesion right where his defect. This the only option where there’s virtually no risk of any kind of graft rejection or anything of that nature.

Pulmonary fibrosis is a condition in which the tissue deep in your lungs becomes scarred over time. This tissue gets thick and stiff. That makes it hard for you to catch your breath, and your blood may not get enough oxygen. Causes of pulmonary fibrosis include environmental pollutants, some medicines, some connective tissue diseases, and interstitial lung disease. Interstitial lung disease is the name for a large group of diseases that inflame or scar the lungs. In most cases, the cause cannot be found. This is called idiopathic pulmonary fibrosis

An animation of blood flow inside the hollow fiber of a hemofilter, or a dialyzer, and the flow of the dialysate in an opposite direction with increased extraction of waste and small molecules from the blood as the concentration of these molecules is reduced downstream and exposed to new dialysate.
To learn about Hemodialysis..
https://www.thevirtualnephrolo....gist.com/specialties
The Virtual Nephrologist is your gateway to optimal health.
To learn more about Hypertension, Kidney Disease and Dialysis:
https://thevirtualnephrologist.com/
About Dr. Rifai:
Dr. Ahmad Oussama Rifai is certified by the American Board of Internal Medicine (ABIM) in the specialty of Internal Medicine and the sub-specialty of Nephrology.
MEET DR. RIFAI
https://www.thevirtualnephrologist.com/rifai/
Follow The Virtual Nephrologist on SOCIAL MEDIA:
-Facebook: https://www.facebook.com/thevirtualnephrologist
-Instagram: https://www.instagram.com/thevirtualnephrologist/
-Twitter: https://twitter.com/VNephrologist
-TikTok: https://www.tiktok.com/@thevirtualnephrologist
Schedule a virtual consult:
https://www.thevirtualnephrolo....gist.com/schedule-a-
Best wishes for great health | The Virtual Nephrologist

Warning: This video contains actual surgical footage, which may not be suitable for all viewers.
To learn more about coronary artery bypass surgery, please visit http://cle.clinic/3b7dqpE
Cardiothoracic surgeon Faisal Bakaeen, MD, discusses how he does single and bilateral internal mammary arteries, and the benefits of doing this type of coronary artery bypass.
If you liked the video hit like and subscribe for more!
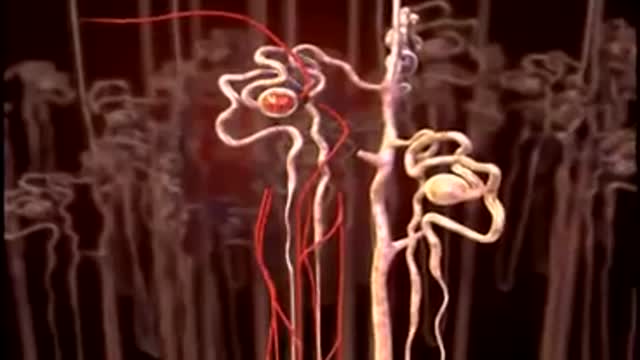
The Urinary System is a group of organs in the body concerned with filtering out excess fluid and other substances from the bloodstream. The substances are filtered out from the body in the form of urine. Urine is a liquid produced by the kidneys, collected in the bladder and excreted through the urethra.