Top videos
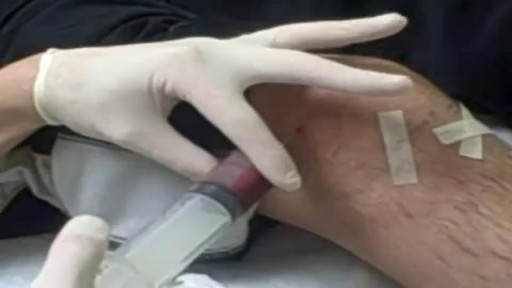
nee joint aspiration and injection are performed to aid in diagnosis and treatment of knee joint diseases. The knee joint is the most common and the easiest joint for the physician to aspirate. One approach involves insertion of a needle 1 cm above and 1 cm lateral to the superior lateral aspect of the patella at a 45-degree angle. Once the needle has been inserted 1 to 1½ inches, aspiration aided by local compression is performed. Local corticosteroid injections can provide significant relief and often ameliorate acute exacerbations of knee osteoarthritis associated with significant effusions. Among the indications for arthrocentesis are crystal-induced arthropathy, hemarthrosis, unexplained joint effusion, and symptomatic relief of a large effusion. Contraindications include bacteremia, inaccessible joints, joint prosthesis, and overlying infection in the soft tissue. Large effusions can recur and may require repeat aspiration. Anti-inflammatory medi
Frostbite is an injury caused by freezing of the skin and underlying tissues. First your skin becomes very cold and red, then numb, hard and pale. Frostbite is most common on the fingers, toes, nose, ears, cheeks and chin. Exposed skin in cold, windy weather is most vulnerable to frostbite. But frostbite can occur on skin covered by gloves or other clothing. Frostnip, the first stage of frostbite, doesn't cause permanent skin damage. You can treat very mild frostbite with first-aid measures, including rewarming your skin. All other frostbite requires medical attention because it can damage skin, tissues, muscle and bones. Possible complications of severe frostbite include infection and nerve damage.

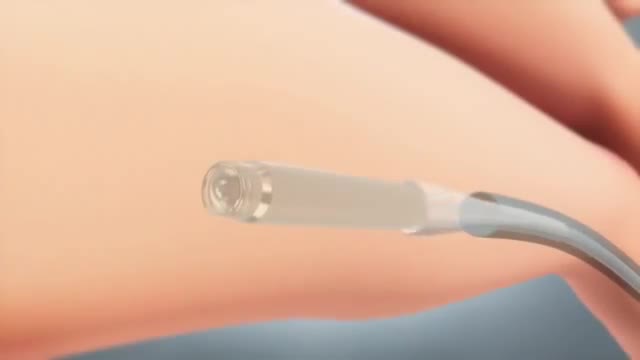
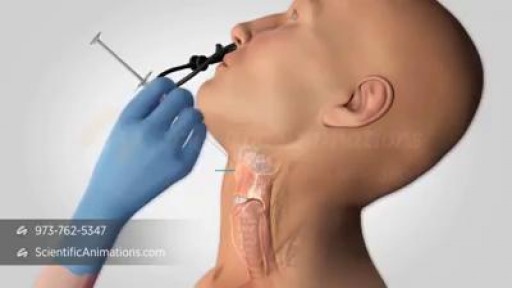
Lip augmentation is a cosmetic procedure that can give you fuller, plumper lips. These days, an injectable dermal filler is the most commonly used method of lip augmentation. There are many types of dermal fillers that can be injected in your lips and around your mouth.

In breastfeeding, the latch is the moment everything comes together: Your baby takes a big mouthful of your nipple and areola (or "latches on"), begins to suck, and draws out your milk. When your baby has established a good latch, your nipple soreness is minimized and your little one gets the nourishment he needs. How do you pull all that off? First and most important, have faith in yourself and your baby. "Babies are designed to breastfeed," says Emily Pease, R.N., international board certified lactation consultant (IBCLC), of Swedish Hospital's Breastfeeding Center in Seattle. "They are born with instincts that help them find Mom's breast and latch on often with very little assistance. And if problems do come up, there are lots of ways to troubleshoot." Here are more steps to get a good latch right from the start.

There is no sure way for women to avoid their most common type of cancer. But when breast cancer is found early, the survival chances are the greatest. Here is October’s survivor story:
It has been 25 years since a woman very dear to us here at CBS 11 News found out she was a living cliché. Following in her birth mother’s footsteps, she discovered breast cancer on her own. Today she’s alive, urging every woman she can reach to do a self-check.
We here at CBS 11 News have come to know Juneil Jones-Flemming’s soft, warm greeting.
Some of you may have too

A man's age matters. As men get older, the chances of conceiving and having a healthy child decline. Male fertility starts to decline after 40 when sperm quality decreases. This means it takes longer for their partners to conceive and when they do, there's an increased risk of miscarriage.

A brief description of the pathophysiology, clinical features, warning signs, diagnosis and management of Dengue fever. This description is based on the World Health Organisation guidelines of the management of Dengue fever.

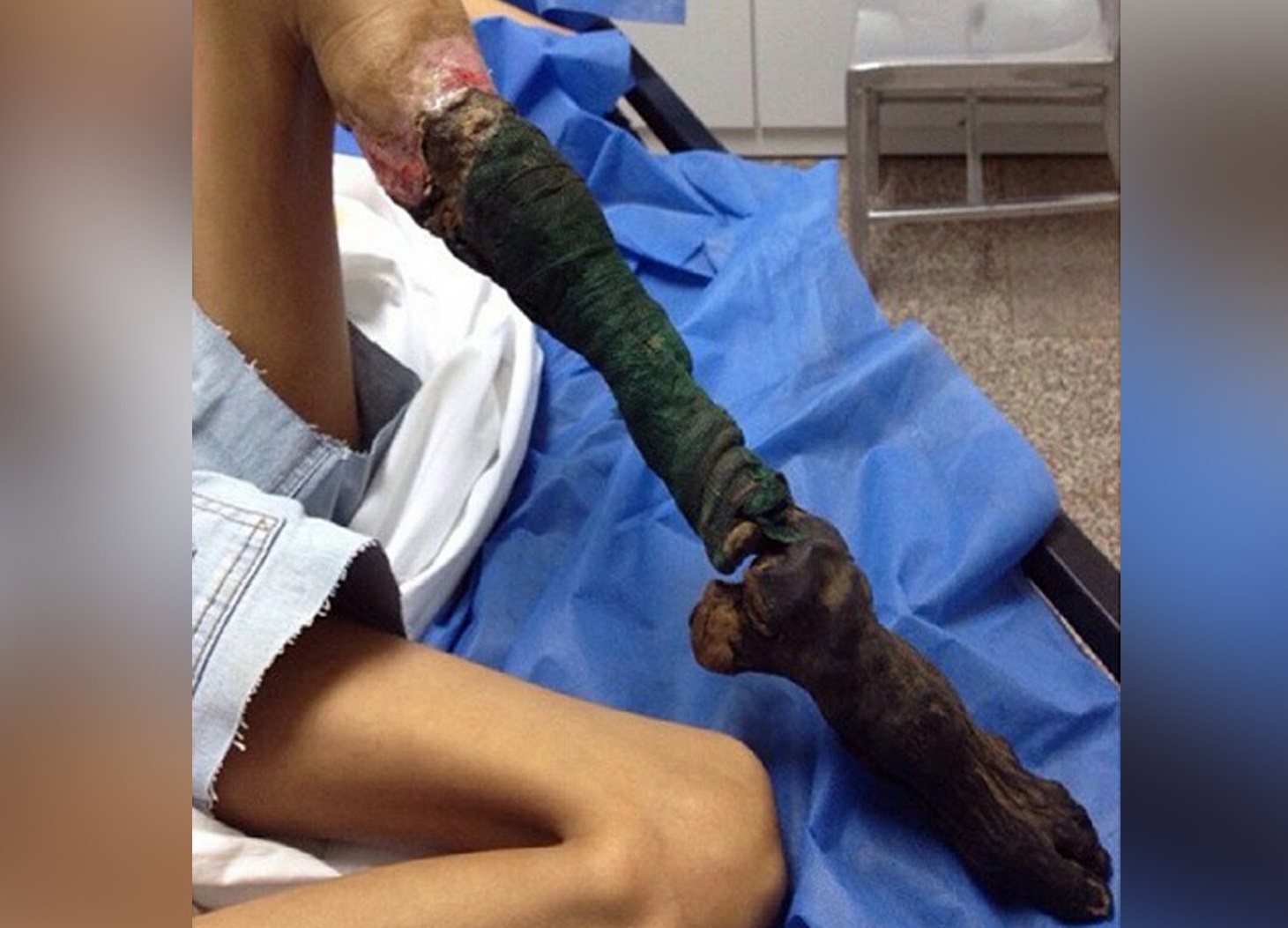
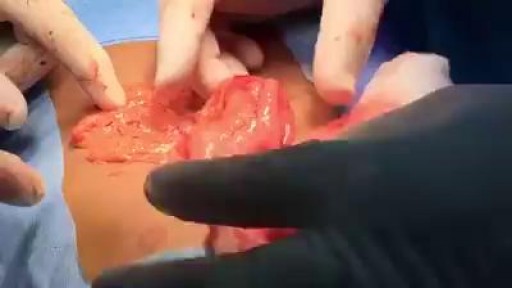
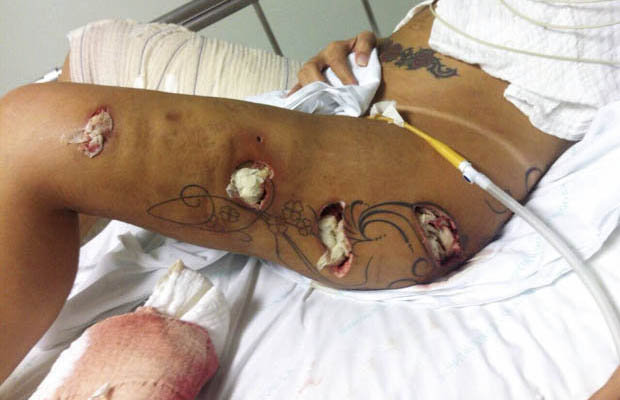
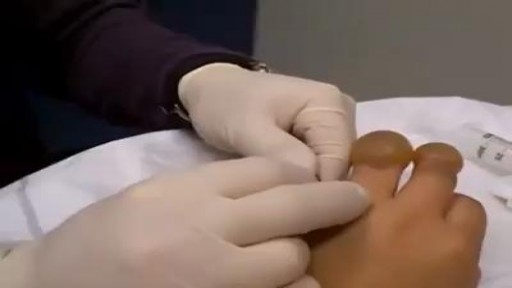
In this video a real case of the extremely rare disease "Fibrodysplasia ossificans progressiva" or what is called the "FOP" This disease is commonly misdiagnosed and usually end up by unnecessary surgery which exaggerate the disease. Children born with FOP characteristically have deformed great toes, possibly missing a joint or simply presenting with a notable lump at the minor joint. The first "flare-up" that leads to the formation of FOP bones usually occurs before the age of 10. FOP is a genetic disease. The bone growth progresses from the top downward, just as bones grow in fetuses. A child with FOP will typically develop bones starting at the neck, then on the shoulders, arms, chest area and finally on the feet. However it does not necessarily occur in this order due to injury-caused flare-ups. Often, the tumor-like lumps that characterize the disease appear suddenly. The gene that causes ossification is normally deactivated after a fetus' bones are formed in the womb, but in patients with FOP, the gene keeps working. Aberrant bone formation in patients with FOP occurs when injured connective tissue or muscle cells at the sites of injury or growth incorrectly express an enzyme for bone repair during apoptosis (self-regulated cell death), resulting in lymphocytes containing excess bone morphogenetic protein 4 (BMP4) provided during the immune system response. Since the incorrect enzyme remains unresolved within the immune response, the body continues providing the incorrect BMP4-containing lymphocytes. BMP4 is a product that contributes to the development of the skeleton in the normal embryo.
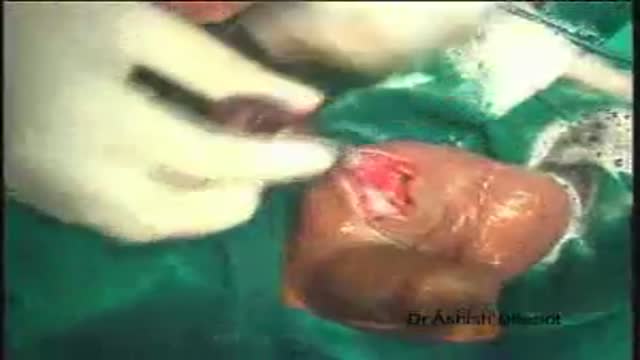
The voice box, or larynx, has three important functions. It is necessary for breathing, voice and swallowing. The vocal folds have two positions, open (apart) for breathing (picture I) and closed (together) for making sound, coughing and sealing off the lungs when swallowing (picture II). When one of the vocal folds are paralyzed, it usually rests in an in-between position (picture III), and neither opens for breathing, nor closes for voicing, coughing, or swallowing. Usually, the effects on the voice are the most dramatic. The voice becomes weak and breathy. People can only say a few words per breath, and are frequently out-of-breath, or physically tired when trying to speak for more than a few minutes straight. The voice may also get somewhat high and squeaky, with a diminished range. Swallowing may be affected as well, where you may notice some choking or coughing with certain liquids. Your cough is frequently different and very weak. This is a serious problem for patients with with vocal fold paralysis because one of the most important functions of the larynx is to keep liquids out of the lungs, and to be able to cough up mucus. When this does not happen, you are at risk for getting an "aspiration" pneumonia. The surgical procedure to restore these important functions is called "medialization laryngoplasty"
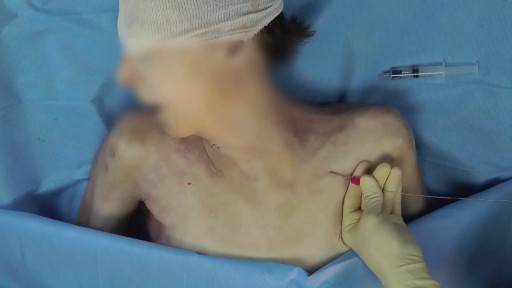
First described by Aubaniac in 1952, central venous catheterization, or central line placement, is a time-honored and tested technique of quickly accessing the major venous system. Benefits over peripheral access include greater longevity without infection, line security in situ, avoidance of phlebitis, larger lumens, multiple lumens for rapid administration of combinations of drugs, a route for nutritional support, fluid administration, and central venous pressure (CVP) monitoring. Central vein catheterization is also referred to as central line placement. Overall complication rates are as high as 15%, [1, 2, 3, 4] with mechanical complications reported in 5-19% of patients, [5, 6, 7] infectious complications in 5-26%, [1, 2, 4] and thrombotic complications in 2-26%. [1, 8] These complications are all potentially life-threatening and invariably consume significant resources to treat. Placement of a central vein catheter is a common procedure, and house staff require substantial training and supervision to become facile with this technique. A physician should have a thorough foreknowledge of the procedure and its complications before placing a central vein catheter. The supraclavicular approach was first put into clinical practice in 1965 and is an underused method for gaining central access. It offers several advantages over the infraclavicular approach to the subclavian vein. At the insertion site, the subclavian vein is closer to the skin, and the right-side approach offers a straighter path into the subclavian vein. In addition, this site is often more accessible during cardiopulmonary resuscitation (CPR) and during active surgical cases. Finally, in patients who are obese, this anatomic area is less distorted.