Top videos

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.
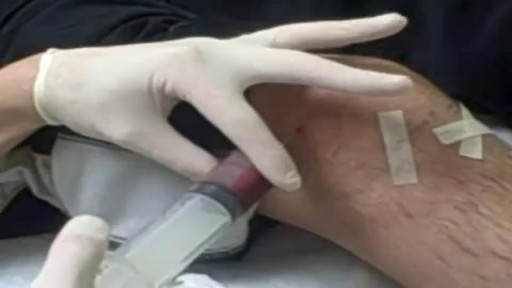
nee joint aspiration and injection are performed to aid in diagnosis and treatment of knee joint diseases. The knee joint is the most common and the easiest joint for the physician to aspirate. One approach involves insertion of a needle 1 cm above and 1 cm lateral to the superior lateral aspect of the patella at a 45-degree angle. Once the needle has been inserted 1 to 1½ inches, aspiration aided by local compression is performed. Local corticosteroid injections can provide significant relief and often ameliorate acute exacerbations of knee osteoarthritis associated with significant effusions. Among the indications for arthrocentesis are crystal-induced arthropathy, hemarthrosis, unexplained joint effusion, and symptomatic relief of a large effusion. Contraindications include bacteremia, inaccessible joints, joint prosthesis, and overlying infection in the soft tissue. Large effusions can recur and may require repeat aspiration. Anti-inflammatory medi
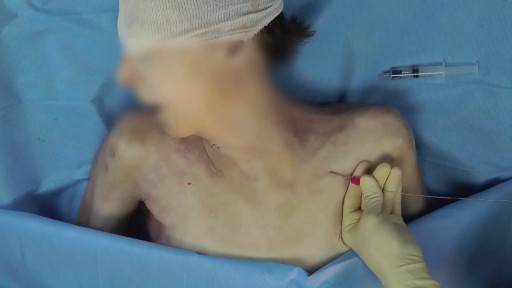
First described by Aubaniac in 1952, central venous catheterization, or central line placement, is a time-honored and tested technique of quickly accessing the major venous system. Benefits over peripheral access include greater longevity without infection, line security in situ, avoidance of phlebitis, larger lumens, multiple lumens for rapid administration of combinations of drugs, a route for nutritional support, fluid administration, and central venous pressure (CVP) monitoring. Central vein catheterization is also referred to as central line placement. Overall complication rates are as high as 15%, [1, 2, 3, 4] with mechanical complications reported in 5-19% of patients, [5, 6, 7] infectious complications in 5-26%, [1, 2, 4] and thrombotic complications in 2-26%. [1, 8] These complications are all potentially life-threatening and invariably consume significant resources to treat. Placement of a central vein catheter is a common procedure, and house staff require substantial training and supervision to become facile with this technique. A physician should have a thorough foreknowledge of the procedure and its complications before placing a central vein catheter. The supraclavicular approach was first put into clinical practice in 1965 and is an underused method for gaining central access. It offers several advantages over the infraclavicular approach to the subclavian vein. At the insertion site, the subclavian vein is closer to the skin, and the right-side approach offers a straighter path into the subclavian vein. In addition, this site is often more accessible during cardiopulmonary resuscitation (CPR) and during active surgical cases. Finally, in patients who are obese, this anatomic area is less distorted.

Blood type (or blood group) is determined, in part, by the ABO blood group antigens present on red blood cells. A blood type (also called a blood group) is a classification of blood based on the presence or absence of inherited antigenic substances on the surface of red blood cells (RBCs).
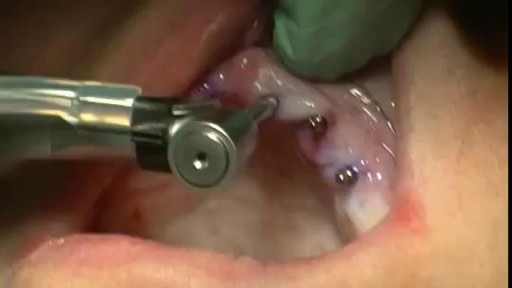
A Beautiful Smile at Lake Pointe is Sugar Land premier dentistry practice. Dr. Lance Jue has been serving patients' preventive, restorative and cosmetic dental needs here in Sugar Land for over 19 years. Book an appointment online now with Dr. Lance Jue

Demystify knee pain and discover nine of the most common causes of pain in this complex joint. Join Burke Selbst PT as we work through our simple screening for the most common types of problems.
Burke is the founder and clinical director of Focus Physical Therapy in Bend Oregon.
Find him:
https://focusptbend.com
https://facebook.com/focusphysio
Intro Song Credit
Adventures by A Himitsu https://www.youtube.com/channel/UCgFw...
Creative Commons — Attribution 3.0 Unported— CC BY 3.0
http://creativecommons.org/licenses/b...
Music released by Argofox https://youtu.be/8BXNwnxaVQE
Music provided by Audio Library https://youtu.be/MkNeIUgNPQ8
For more information please visit: https://www.yalemedicine.org/c....onditions/acl-injury
Serious injuries, by and large, cause a lot of swelling in the knee. Especially in younger patients. Now, someone could be arthritic and they overdo it going for a big long hike and they get some swelling the next day. But rapid onset of swelling, it's like hard to make out where your kneecap is, is a pretty big cardinal sign that there's something serious that's happened to your knee. Rapid onset swelling is usually due to blood in the joint. "A meniscus that really tears and flips in the front. You tear your quad or your patellar tendon, your kneecap dislocates, you tear a little blood vessel, your ACL tears, a piece of cartilage in bone gets knocked off and causes bleeding. So a lot of the really significant injuries, people get rapid onset swelling within three to four hours and they should seek attention There's always exceptions to rules, but if your knee looks like a grapefruit, you should go get it checked.