Top videos

When placement of a urethral catheter is contraindicated or unsuccessful, percutaneous suprapubic urinary bladder catheterization is a commonly performed procedure to relieve urinary retention. [1, 2] This topic describes the Catheter over needle technique. The Seldinger technique is described in the Clinical Procedures topic Suprapubic Aspiration.
Kirschner wires or K-wires or pins are sterilized, sharpened, smooth stainless steel pins. Introduced in 1909 by Martin Kirschner, the wires are now widely used in orthopaedics and other types of medical and veterinary surgery. They come in different sizes and are used to hold bone fragments together (pin fixation) or to provide an anchor for skeletal traction. The pins are often driven into the bone through the skin (percutaneous pin fixation) using a power or hand drill. They also form part of the Ilizarov apparatus.
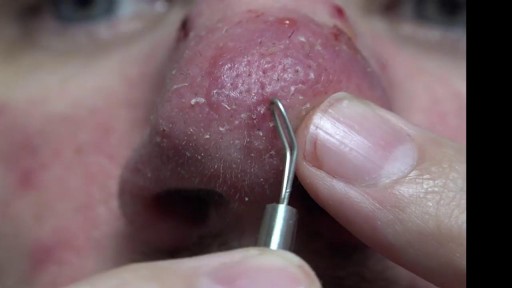
Cystic acne is a severe type of acne in which the pores in the skin become blocked, leading to infection and inflammation. The skin condition mainly affects the face, but also often affects the upper trunk and upper arms. Acne most often affects adolescents and young adults, with an estimated 80 percent of people between 11 and 30 years of age experiencing acne at some point. Cystic acne is the most severe form and affects far fewer people. In 2009, the Centers for Disease Control and Prevention (CDC) found that acne was the top reason people gave for visiting a dermatologist.

Atrial fibrillation (also called AFib or AF) is a quivering or irregular heartbeat (arrhythmia) that can lead to blood clots, stroke, heart failure and other heart-related complications. Some people refer to AF as a quivering heart. An estimated 2.7 million Americans are living with AF.

This patient presented to the ER for umbilical pain and had a history of umbilical hernia. He was concerned about the possibility of incarceration of the hernia.
In this video we explain how the clinical exam helps to differentiate a simple painful hernia from an incarcerated one.
***Thanks to the patient for sharing his history and exam with YouTube world***

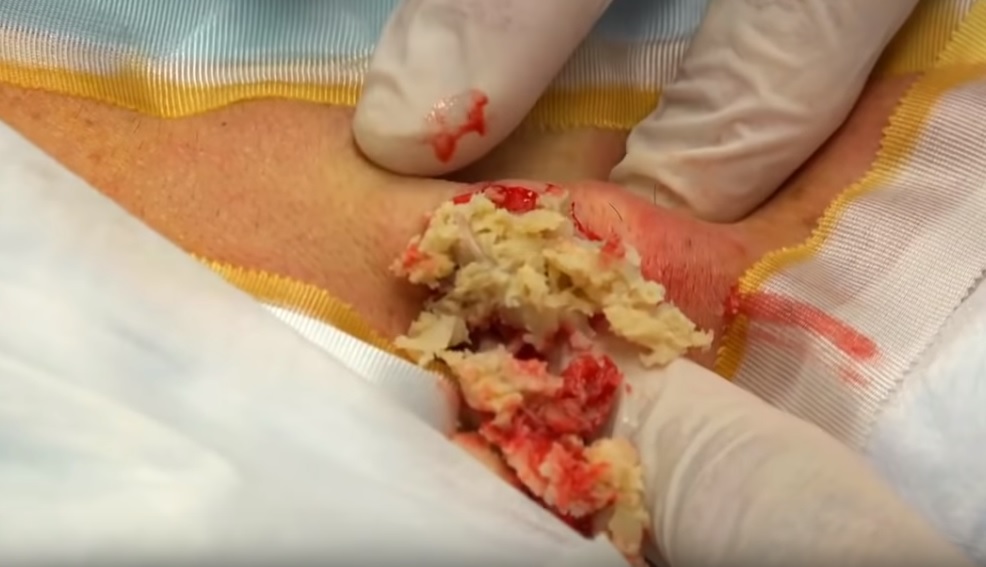
Lattrell Wells was a perfect candidate for the MACI procedure. Dr. Michael O'Malley is a sports medicine surgeon at Carilion Clinic, "It’s a two stage procedure. So what we do is we actually harvest a small portion of the patient's cartilage and bone cells and we send it to a lab where the lab then that grows additional cartilage cells. It comes back to us in a little sheet and six weeks after that initial surgery, we re-implant the cartilage in a second surgery where we implant that sheet depending on the size of lesion right where his defect. This the only option where there’s virtually no risk of any kind of graft rejection or anything of that nature.

This video: Pancreatic cancer begins in the tissues of your pancreas — an organ in your abdomen that lies horizontally behind the lower part of your stomach. Your pancreas secretes enzymes that aid digestion and hormones that help regulate the metabolism of sugars. Pancreatic cancer often has a poor prognosis, even when diagnosed early. Pancreatic cancer typically spreads rapidly and is seldom detected in its early stages, which is a major reason why it's a leading cause of cancer death. Signs and symptoms may not appear until pancreatic cancer is quite advanced and complete surgical removal isn't possible.
An abscess is an infectious process characterized by a collection of pus surrounded by inflamed tissue. [1, 2] Abscesses can form anywhere in the body, from a superficial skin (subcutaneous) abscess to deep abscesses in muscle, organs, or body cavities. Patients with subcutaneous skin abscesses present clinically as a firm, localized, painful, erythematous swelling that becomes fluctuant (see the image below).

► Get a free NCLEX NGN sample test today: http://lectur.io/nclexrnsampletestyt
► Create your free account today: http://lectur.io/nurseregisteryt
► If you’re an nursing educator or faculty member, visit: http://lectur.io/nursytb2u
In this video “How To Do An IM (Intramuscular) Injection” you will learn about:
►the steps in the administration of intramuscular medications
►the angle to position the syringe while administering an intramuscular injection
►the landmark to administer an intramuscular injection in the deltoid muscle
►5 tips for the safe administration of an intramuscular medication
►the steps of the Z-track method for intramuscular injections
►the role of aspirating blood during an intramuscular injection and evaluate whether this practice is currently in use
► This video is part of the Lecturio course “Fundamentals of Nursing: Clinical Skills”
► WATCH the complete course on http://lectur.io/njection
► THE PROF: Samantha Rhea MSN, RN has been a nurse since 2008 and a nursing faculty teacher since 2012. She has been recognized for clinical excellence as an interventional cardiology nurse and also led a Joint Commission Accredited Stroke Center. Ms. Rhea is an award-winning expert in clinical teaching and continues to maintain a current clinical practice and teaches at a University nursing program.
► LECTURIO is your smart tutor for nursing school: Learn the toughest NCLEX® topics with high-yield video lectures, integrated quiz questions, and more. Register now to study anytime and anywhere you want to: https://nursing.lecturio.com/#/
► CHECK OUT ALL NURSING COURSES:
Leadership Nursing: http://lectur.io/leadershipnursing
Dosage Calculation Nursing: http://lectur.io/dosagecalcnursing
Physiology Nursing: http://lectur.io/physiologynursing
Medical Surgical Nursing: http://lectur.io/medsurgnursing
Pharmacology Nursing: http://lectur.io/pharmacologynursing
NCLEX® Pharmacology Nursing: http://lectur.io/pharmnclexnursing
Pediatric Nursing: http://lectur.io/pediatricnursing
Study Skills Nursing: http://lectur.io/studyskillsnursing
Fundamentals of Nursing - Theory: http://lectur.io/fundamentalstheory
Fundamentals of Nursing - Clinical Skills: http://lectur.io/fundamentalsclinicalskills
Nursing Prerequisites: http://lectur.io/nursingprerequisites
Mental Health Nursing: http://lectur.io/mentalhealthnursing
Maternal-Newborn Nursing: http://lectur.io/maternalnewbornnursing
► INSTALL the free Lecturio app
iTunes Store: https://app.adjust.com/z21zrf
Play Store: https://app.adjust.com/b01fak
► SUBSCRIBE to our YouTube channel: http://lectur.io/subscribenursing
► WATCH MORE ON YOUTUBE: http://lectur.io/nursingplaylists
► LET’S CONNECT:
Facebook: www.facebook.com/lecturio.nursing
Instagram: www.instagram.com/lecturio_nursing
Join Discord Community: https://discord.gg/Ue95WDxCrp
TikTok: www.tiktok.com/@lecturio_nursing
LinkedIn: https://www.linkedin.com/company/lecturio-medical/
#nursingschool #nursingeducation #nursingclinicalskills #leadershipnursing #nclex #nursingfundamentals #nursingclinical #nursingskills

Dr. Ailawadi, M.D., the Chair of Cardiac Surgery at Michigan Medicine, specializes in minimally invasive valve surgery as well as complex cardiac operations. This video shows step by step footage of a Coronary Artery Bypass Graft (CABG) in a complex patient. In this case, CABG was performed through a sternotomy (through the breast bone) using the internal thoracic artery and saphenous leg veins to bypass obstructed coronary arteries. In this video, Dr. Ailawadi will perform a triple vessel bypass (CABG) which has been shown to minimize the risk of future heart attack and help patients live longer in the setting of complex coronary artery disease.
To learn more about cardiac surgery at Michigan Medicine, visit: https://medicine.umich.edu/dept/cardiac-surgery
To learn more about Frankel Cardiovascular Center, visit: https://www.umcvc.org/
To watch the full playlist, visit: https://www.youtube.com/playli....st?list=PLNxqP-XbH8B
-------------------------------------------------------
Subscribe to Michigan Medicine’s YouTube channel for upcoming videos and future live streams featuring our experts answering your questions.
-------------------------------------------------------
Follow Michigan Medicine on Social:
Twitter: https://twitter.com/umichmedicine
Instagram: https://www.instagram.com/umichmedicine/
Facebook: https://www.facebook.com/MichiganMedicine/
Follow the U-M Frankel Cardiovascular Center on Social:
Twitter: https://twitter.com/umichcvc
Facebook: https://www.facebook.com/Unive....rsityofMichiganCardi
#MichiganMedicine #MedEd #CardiacSurgery #UniversityOfMichiganHealth #FrankelCardiovascularCenter #Cardiology #CardiacSurgeon

The hepatitis E virus, responsible for major epidemics of viral hepatitis in subtropical and tropical countries, was cloned only 7 years ago.1 Hepatitis E was found to belong to the family of Caliciviridae, which includes the Norwalk virus—a common cause of gastroenteritis in humans—and consists of a single, plus-strand RNA genome of approximately 7.2 kb without an envelope (Fig. 1). The virus contains at least three open reading frames encoding viral proteins against which antibodies are made on exposure. These antibodies, especially those against the capsid protein derived from the second open reading frame2 and a protein of unknown function derived from the third open reading frame, are detected by currently available serologic assays. Retrospective studies on stored sera of past epidemics of viral hepatitis in Mexico, Africa, Afghanistan, Pakistan, India, Bangladesh, Burma, Nepal, and Borneo have revealed that all were caused by strains of hepatitis E. In addition, hepatitis E was found to be responsible for the hepatitis epidemic in the southern part of Xinjiang, China, in which 120,000 persons became infected between September 1986 and April 1988.3 Hepatitis E predominantly affects young adults (15 to 40 years old). The symptoms of hepatitis E are similar to those of hepatitis A. Frequently, a prodrome consisting of anorexia, nausea, low-grade fever, and right upper abdominal pain is present 3 to 7 days before jaundice develops. Aminotransferase levels peak (usually between 1,000 and 2,000 U/L) near the onset of symptoms; bilirubin levels (10 to 20 mg/dL) peak later. Jaundice usually resolves after 1 to 2 weeks. In about 10% of cases, the disease is fulminant—especially in pregnant women, among whom mortality rates as high as 20% due to hemorrhagic and thrombotic complications have been reported. No evidence has suggested that hepatitis E can cause chronic infection. Transmission is by the fecal-oral route, predominantly through fecally contaminated drinking water supplies. In addition, however, preliminary reports have suggested transmission of the hepatitis E virus through blood transfusions. Volunteer studies confirmed the presence of the virus in serum and feces before and during clinical disease.4 The virus is shed into feces approximately 1 week before symptoms develop. The incubation period varies from 2 to 9 weeks (mean duration, approximately 45 days). Until now, a few reports had described symptomatic hepatitis E acquired in Europe;5, 6 all patients with symptomatic hepatitis E in the United States were travelers returning from Mexico, Africa, or the Far East, in whom hepatitis E developed after their return home.7 In this issue of the Mayo Clinic Proceedings (pages 1133 to 1136), Kwo and associates describe a case of hepatitis E in a man who had not left the United States during the previous 10 years. Specific serologic tests for hepatitis E virus IgG (enzyme immunoassays and a fluorescent antibody blocking assay) and IgM8 (US strain-specific enzyme-linked immunosorbent assay with use of synthetic polypeptides deduced from the viral genome, as shown in Figure 1), developed at Abbott Laboratories (IgG and IgM) as well as at the Centers for Disease Control and Prevention (IgG), were used to prove that the patient indeed had acute hepatitis E. Researchers at Abbott Laboratories have prepared a report that describes most of the viral genome in this patient (Fig. I).8 Their results are interesting because this strain from the United States differs considerably from hepatitis E strains isolated in Mexico, Burma, Pakistan, or China. Furthermore, the sequence of the US strain is highly homologous (98% and 94% homology at the amino acid level to the second and third open reading frames, respectively) to a recently isolated hepatitis E strain from American swine.9 This finding suggests that, in the United States, hepatitis E is a zoonosis with the swine population as one of its hosts. This relationship would confirm earlier studies in Asia, where swine were also found to carry variants of the hepatitis E virus.10 Why are these two recent discoveries important for medicine in the United States? First, other sporadic, locally acquired cases of acute hepatitis may be caused by hepatitis E. Second, these back-to-back discoveries strongly suggest that a common natural host for hepatitis E is present in countries with more moderate climates. Because swine do not seem to experience any symptoms associated with infection and because symptoms in humans can be minor or absent, we now may also have an explanation for the 1 to 2% of positive hepatitis E serologic results in blood donors in the United States,11 Netherlands,12 and Italy,6 countries with large swine staples. Clearly, more research needs to be done to confirm this hypothesis. Third, in countries with more moderate climates, hepatitis E may often result in a subclinical infection. Is this variation in manifestation due to less virulent strains, and do sequence variations determine virulence? Fourth, swine may be used as an animal model for study of the disease as well as vaccine development.