Top videos

Visit our website to learn more about using Nucleus content for patient engagement and content marketing: http://www.nucleushealth.com/
#LaparoscopicColectomy #ColonSurgery #LargeIntestine
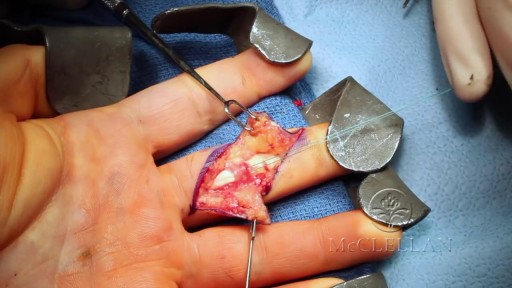
A colectomy is usually done to treat diseases that inflame your colon, a bowel obstruction, colon cancer, or a damaged or injured colon. The anatomy of the colon, and the laparoscopic procedure done to remove a portion of the colon, are depicted.
ANH18221

Contact us to find out more http://www.londonvisionclinic.com/contact-us/ Glenn Carp talks about how both distance and some of the reading can be treated via laser eye surgery for hyperopia
The core features of migraine are headache, which is usually throbbing and often unilateral, and associated features of nausea, sensitivity to light, sound, and exacerbation with head movement. Migraine has long been regarded as a vascular disorder because of the throbbing nature of the pain.

Linen Changes (with Patient in Bed)- Nursing Skills
FREE Nursing School Cheat Sheets at: http://www.NURSING.com
Get the full lesson on Patient Linen Changes here:
https://nursing.com/lesson/ski....lls-01-02-linen-chan
Get the full lesson on Bed Baths here:
https://nursing.com/lesson/skills-01-01-bed-bath/
Check out our new Nurse Care Plan Lessons here:
https://bit.ly/3BPRfPL
Get Access to Thousands of Lessons here:
https://nursing.com/courses/
Welcome to the NURSING Family, we call it the most supportive nursing cohort on the planet.
At NURSING.com, we want to help you remove the stress and overwhelm of nursing school so that you can focus on becoming an amazing nurse.
Check out our freebies and learn more at: (http://www.nursing.com)
Linen Changes (with Patient in Bed)- Nursing Skills
In this video, we’re going to show you how to change the linens with a patient in the bed. This might be after a bed bath or during incontinence care. So check out the bed bath video to see what got us up to this point. We love you guys! Go out and be your best selves today! And, as always, happy nursing!
Bookmarks:
0.05 Linen change introduction
0.16 Linen change supplies
0.30 Adjusting the patient/ sheet removal
1.00 Secure new fitted sheet
1.12 Pro tip
1.40 Roll patient back over
1.50 Repeat linen removal
2.02 Linen disposal
2.20 Wrinkle check
2.31 Reposition the patient for comfort
2.40 Covering the patient/ tuck-in
2.48 Pillowcase change (trick)
3.30 Making the patient comfortable
3.40 Linen change outro
Visit us at https://nursing.com/medical-disclaimer/ for disclaimer information.
NCLEX®, NCLEX-RN® are registered trademarks of the National Council of State Boards of Nursing, INC. and hold no affiliation with NURSING.com.

Ever heard medical terms like MRI or EKG? Funny speaker for nurses and doctors and all-around healthcare speaker Dr. Brad Nieder discusses the funny medical jargon he's encountered during his medical career.
He jokes about medical acronyms and big healthcare terms. His funny medical humor makes the conference attendees burst with laughter and he reads the medical definition for "laugh."
As an experienced physician and keynote speaker, he's perfect for any in-person or virtual conference or event. He's also a great healthcare speaker to bring in for continuing medical education (cme) units!
Learn more about Brad's keynote and virtual speaking, and book him for your next conference or virtual event: https://www.HealthyHumorist.com
Find Dr. Brad on social media:
https://www.facebook.com/HealthyHumor...
https://www.linkedin.com/in/BradNieder
https://twitter.com/HealthyHumorist
https://www.youtube.com/c/BradNiederMD
https://vimeo.com/BradNieder
Brad Nieder, MD, CSP*
The Healthy Humorist
Doctor, Keynote Speaker, Clean Comedian
*CSP=Certified Speaking Professional
"Medical Lingo"
From the DVD "The Healthy Humorist in Orlando: Laughter is the Best Medicine"
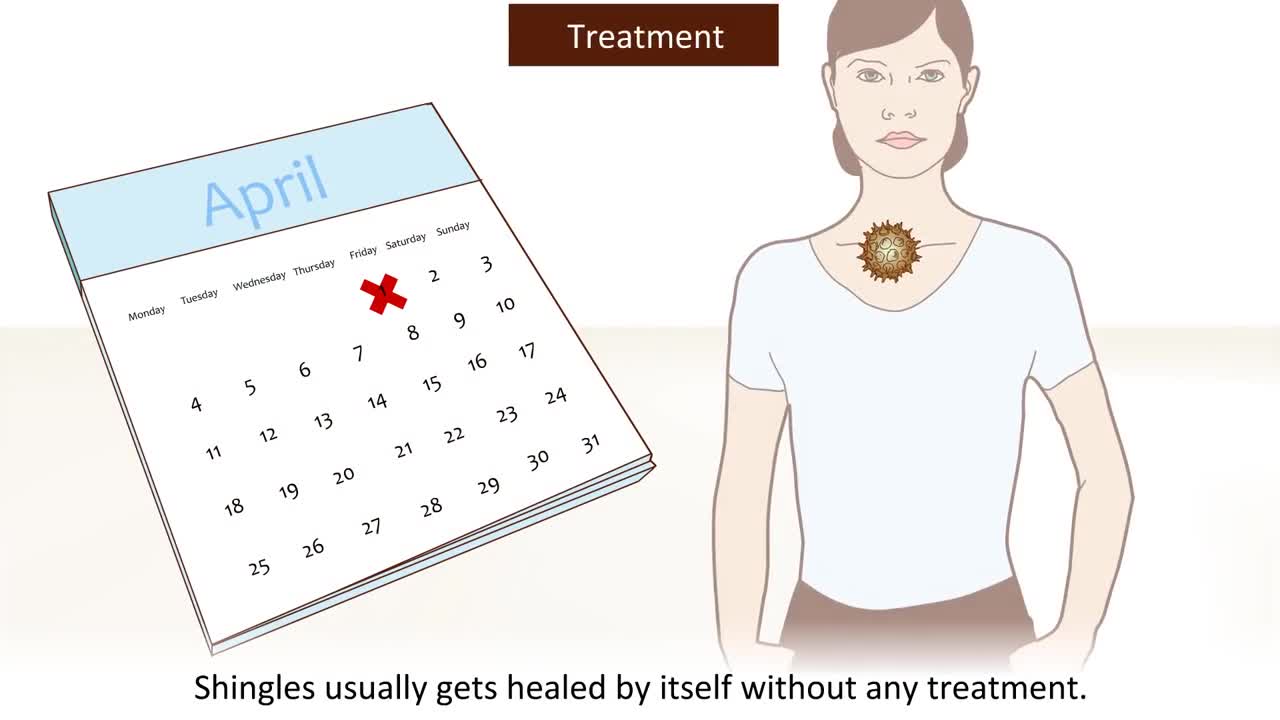
Shingles is a painful skin rash camera.gif. It is caused by the varicella zoster virus. Shingles usually appears in a band, a strip, or a small area on one side of the face or body. It is also called herpes zoster. Shingles is most common in older adults and people who have weak immune systems because of stress, injury, certain medicines, or other reasons. Most people who get shingles will get better and will not get it again. But it is possible to get shingles more than once.
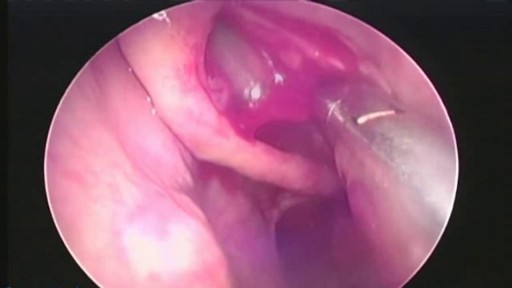
Nasal polyps are linked to allergic rhinitis, asthma, aspirin allergy, sinus infections, acute and chronic infections, something stuck in the nose, and cystic fibrosis. But many times the cause is unknown. Sometimes, people get them before they develop asthma or sinusitis

This particular video is intended as a demonstration of Neurologic Examination. This demonstration is intended as an example of a neurologic exam which may be used as part of the initial evaluation of patients with complaints that may have an underlying neurologic origin. This video is solely for educational purposes and intended for use to prepare for OSCEs incorporating standardized patient encounters. It is not intended as a demonstration of a comprehensive neurologic examination and is not intended as medical advice or medical guidelines.
It is not intended as a complete instructional video and should not be considered a source of complete physical examination instruction.
Instead, it should be treated as a supplement to independent learning using primary Osteopathic Clinical Skills instructional resources. Clinical skills are best learned and developed with support from faculty in the context of a complete Osteopathic Medical School Curriculum.
Osteopathic Clinical Skills is a channel dedicated to discussing and exploring Osteopathic Clinical Skills concepts for medical students, residents, and clinicians and presenting them in an easy to understand manner.
Attributions:
Many thanks to the University of North Texas Health Science Center Texas College of Osteopathic Medicine (UNTHSC - TCOM) for permitting use of the Simulation facilities and equipment during the production of this video.
Additional thanks to the UNTHSC-TCOM standardized patient and faculty volunteers who participated in this production and provided permission for the use of their image in this video.

Thought a snake in your boot was bad? That old 19th-century idiom is nothing compared to one in your ear.
Shocking footage captured the alleged moment that a “surgeon” tried to remove a live snake that infiltrated a woman’s ear. Video of the herpetological surgery has racked up more than 125,000 views as viewers speculate whether or not the squirm-inducing footage is authentic.
“The snake has gone in the ear,” reads the caption to the bizarre Facebook clip, which was posted Sept. 1 by an India-based social media star named Chandan Singh to his 20,126 followers. However, it’s unclear where, when or how this unfortunate event transpired, local outlet the Economic Times reported.
In the nearly four-minute clip, an alleged medical practitioner can be seen using tweezers in a desperate attempt to extract a black and yellow serpent that’s peeking its head out from a female patient’s ear.
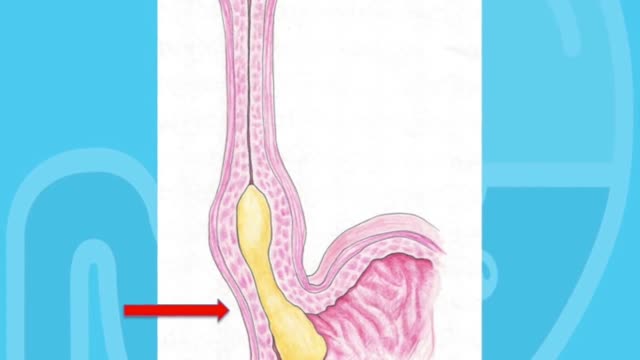
Achalasia is a neurogenic esophageal motility disorder characterized by impaired esophageal peristalsis and a lack of lower esophageal sphincter relaxation during swallowing. Symptoms are slowly progressive dysphagia, usually to both liquids and solids, and regurgitation of undigested food. Evaluation typically includes manometry, barium swallow, and endoscopy. Treatments include dilation, chemical denervation, surgical myotomy, and peroral endoscopic myotomy.
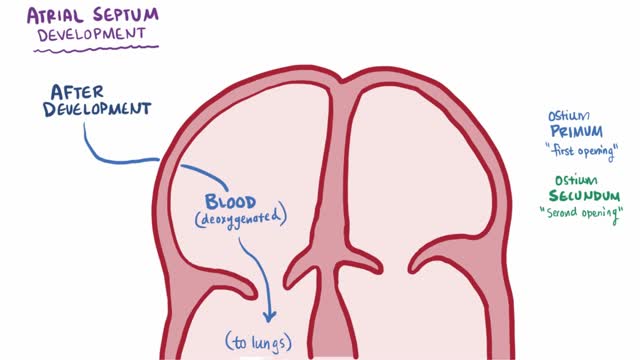
An atrial septal defect (ASD) is a hole in the wall between the two upper chambers of your heart (atria). The condition is present from birth (congenital). Small atrial septal defects may close on their own during infancy or early childhood. Large and long-standing atrial septal defects can damage your heart and lungs. Small defects may never cause a problem and may be found incidentally. An adult who has had an undetected atrial septal defect for decades may have a shortened life span from heart failure or high blood pressure that affects the arteries in the lungs (pulmonary hypertension). Surgery may be necessary to repair atrial septal defects to prevent complications.
Possible causes are a blocked milk duct or bacteria entering the breast. It usually occurs within the first three months of breast-feeding. Symptoms include breast pain, swelling, warmth, fever, and chills. Antibiotics are required. Mild pain relievers can help with discomfort.