Top videos
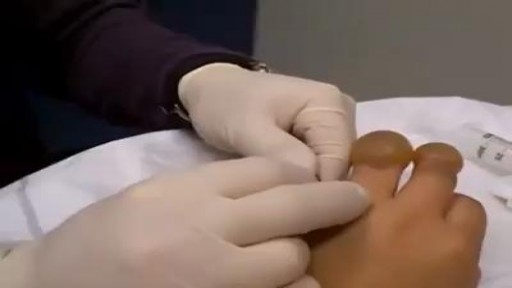
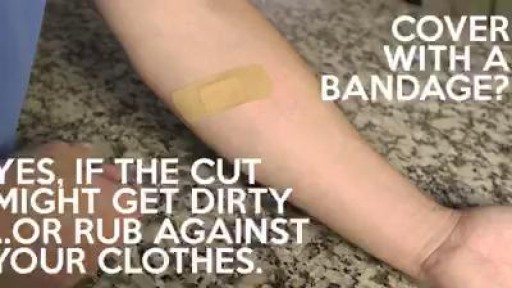
Frostbite is an injury caused by freezing of the skin and underlying tissues. First your skin becomes very cold and red, then numb, hard and pale. Frostbite is most common on the fingers, toes, nose, ears, cheeks and chin. Exposed skin in cold, windy weather is most vulnerable to frostbite. But frostbite can occur on skin covered by gloves or other clothing. Frostnip, the first stage of frostbite, doesn't cause permanent skin damage. You can treat very mild frostbite with first-aid measures, including rewarming your skin. All other frostbite requires medical attention because it can damage skin, tissues, muscle and bones. Possible complications of severe frostbite include infection and nerve damage.

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.
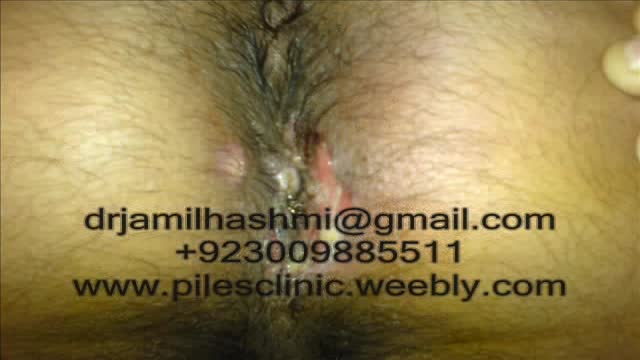
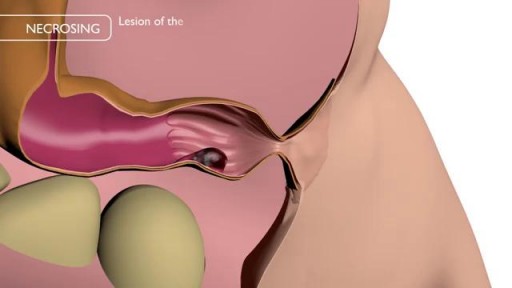
Treatment for Piles,Fistula,hemorrhoids, Hydrocele Without Operation or surgery in pakistan Dr Jamil Ahmad Hashmi ( haripur hazar pakistan )... +923009885511 --- drjamil79@gmail.com
Treatment for Piles,Fistula,Hydrocele Without Operation piles treatment with 60 days Quickly! pain free treatment full life Piles Medicine dr jamil ahmad hashmi ( haripur hazar pakistan ) drjamil79@yahoo.com +923009885511 piles treatment with 60 days Quickly! pain free treatment full life Piles Medicine dr jamil ahmad hashmi...
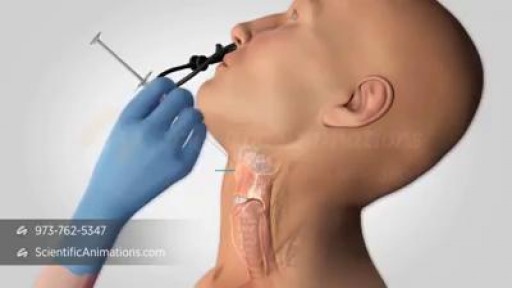
The voice box, or larynx, has three important functions. It is necessary for breathing, voice and swallowing. The vocal folds have two positions, open (apart) for breathing (picture I) and closed (together) for making sound, coughing and sealing off the lungs when swallowing (picture II). When one of the vocal folds are paralyzed, it usually rests in an in-between position (picture III), and neither opens for breathing, nor closes for voicing, coughing, or swallowing. Usually, the effects on the voice are the most dramatic. The voice becomes weak and breathy. People can only say a few words per breath, and are frequently out-of-breath, or physically tired when trying to speak for more than a few minutes straight. The voice may also get somewhat high and squeaky, with a diminished range. Swallowing may be affected as well, where you may notice some choking or coughing with certain liquids. Your cough is frequently different and very weak. This is a serious problem for patients with with vocal fold paralysis because one of the most important functions of the larynx is to keep liquids out of the lungs, and to be able to cough up mucus. When this does not happen, you are at risk for getting an "aspiration" pneumonia. The surgical procedure to restore these important functions is called "medialization laryngoplasty"
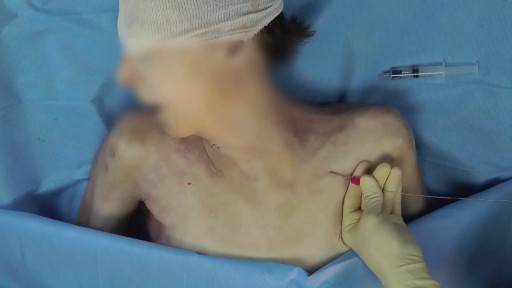
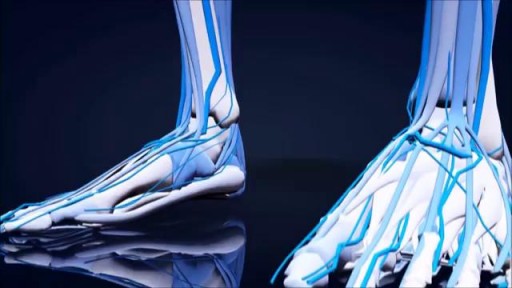
First described by Aubaniac in 1952, central venous catheterization, or central line placement, is a time-honored and tested technique of quickly accessing the major venous system. Benefits over peripheral access include greater longevity without infection, line security in situ, avoidance of phlebitis, larger lumens, multiple lumens for rapid administration of combinations of drugs, a route for nutritional support, fluid administration, and central venous pressure (CVP) monitoring. Central vein catheterization is also referred to as central line placement. Overall complication rates are as high as 15%, [1, 2, 3, 4] with mechanical complications reported in 5-19% of patients, [5, 6, 7] infectious complications in 5-26%, [1, 2, 4] and thrombotic complications in 2-26%. [1, 8] These complications are all potentially life-threatening and invariably consume significant resources to treat. Placement of a central vein catheter is a common procedure, and house staff require substantial training and supervision to become facile with this technique. A physician should have a thorough foreknowledge of the procedure and its complications before placing a central vein catheter. The supraclavicular approach was first put into clinical practice in 1965 and is an underused method for gaining central access. It offers several advantages over the infraclavicular approach to the subclavian vein. At the insertion site, the subclavian vein is closer to the skin, and the right-side approach offers a straighter path into the subclavian vein. In addition, this site is often more accessible during cardiopulmonary resuscitation (CPR) and during active surgical cases. Finally, in patients who are obese, this anatomic area is less distorted.
A Beautiful Smile at Lake Pointe is Sugar Land premier dentistry practice. Dr. Lance Jue has been serving patients' preventive, restorative and cosmetic dental needs here in Sugar Land for over 19 years. Book an appointment online now with Dr. Lance Jue
http://natural-breast-increase.plus101.com
---How To Make Bigger Breast. Can You Really Increase You Breast Size Naturally Without Surgery, Pills, Creams Etc Etc
Well a new website call natural-breast-increase.plus101.com says you can and thousands of women have already used there strategies.
And the best part about the this method is that you don't have to go through any expensive and painful surgery.
If you'd like to increase your own cup size then just visit the site below. I recommend the methods 100%
http://natural-breast-increase.plus101.com
How To Make Bigger Breast
http://www.youtube.com/watch?v=0cTQ3SZ4JIk
How To Make Bigger Breast,
can fenugreek increase breast size,
can i increase my breast size,
can i increase my breast size without surgery,
can i naturally increase breast size,
can we increase breast size naturally,
can women increase breast size naturally,
can you increase breast size,
can you increase breast size naturally,
can you make your breasts bigger,
cheap breast augmentation,
cheap breast implants,
cost of breast implants,
cream for breast enlargement,
cream to increase breast size,
curves breast enhancers,