Top videos
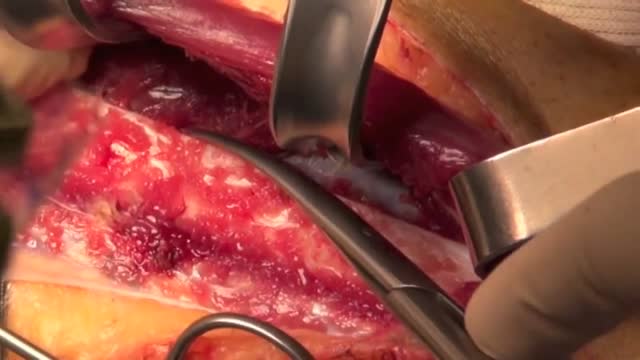
The peroneal artery is closely positioned to the fibula. The artery arises from the tibioperoneal trunk, distal to the takeoff of the anterior tibial artery (seen in the illustration below perforating the interosseous membrane). The peroneal artery sends perforators laterally to the skin of the lower leg, sometimes in a septocutaneous fashion via the lateral intermuscular septum, but often with muscular perforators. The length of the pedicle is usually short, but can be increased substantially by dissecting the peroneal artery and its venae from the fibula and using the distal bone for reconstruction.
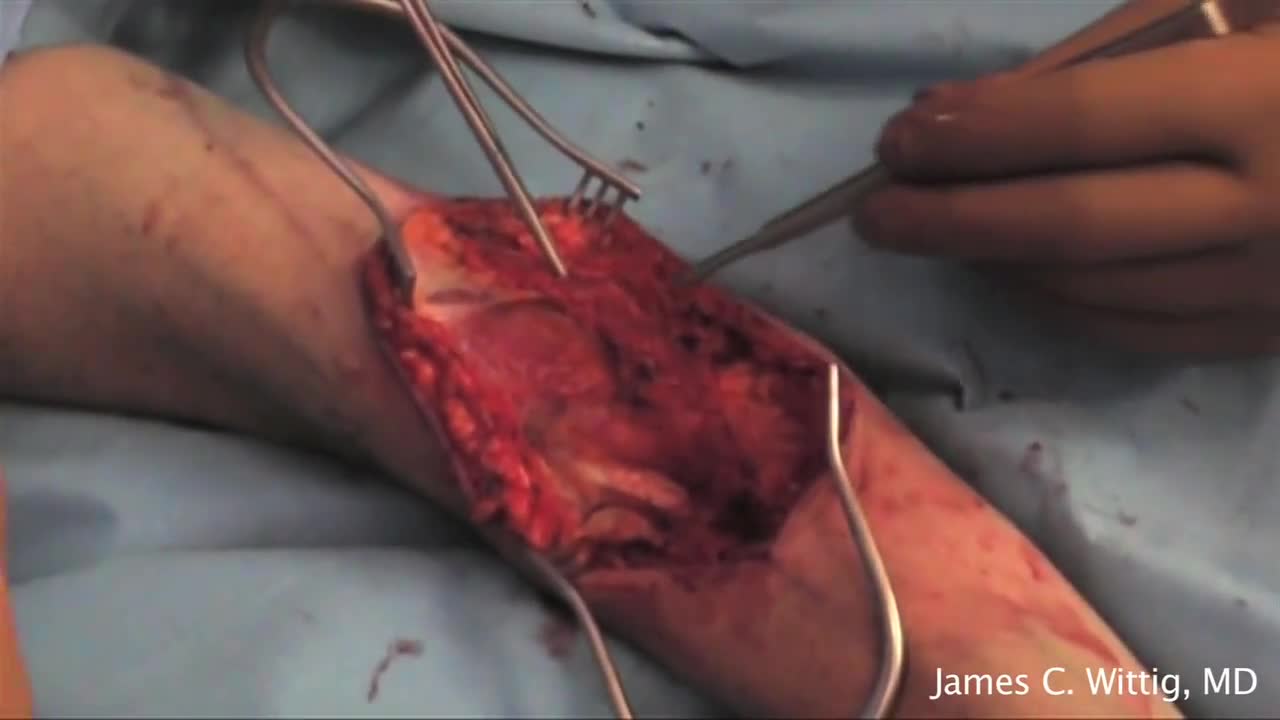
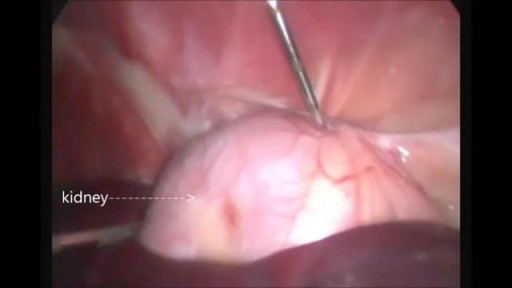
Giant cell tumour is a locally aggressive primary bone tumour, located eccentrically in the metaphysis and epiphysis of a long bone. It commonly affects distal end of Femur, proximal end of Tibia and distal end of Radius. It is occasionally reported in small bones of hand and foot[1], spine[2] and pelvis[3]. Though it occurs in 20 - 35 year old individuals commonly, it can also be seen in children as young as 2 years[4] and also in older individuals

Alcoholic hepatitis is inflammation of the liver caused by drinking alcohol. Alcoholic hepatitis is most likely to occur in people who drink heavily over many years. However, the relationship between drinking and alcoholic hepatitis is complex. Not all heavy drinkers develop alcoholic hepatitis, and the disease can occur in people who drink only moderately. If you're diagnosed with alcoholic hepatitis, you must stop drinking alcohol. People who continue to drink alcohol face a high risk of serious liver damage and death.

Use warm water and sea salt. Soak the wart for 10 to 15 minutes in warm salt water to moisten the skin. Scrape the dead skin layers off the wart using a nail file, pumice stone or mild sandpaper. You could also use your fingers, but wash them thoroughly before and after, as warts can easily spread.
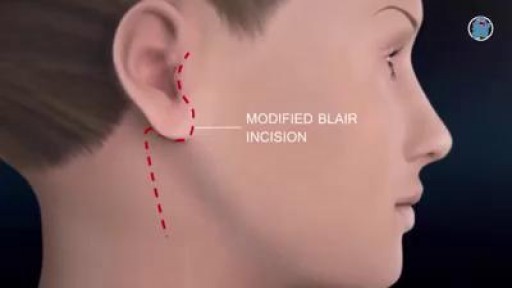
Minimally invasive parotid surgery techniques are currently utilized here in Atlanta by our practice to allow the same operation to be performed with no permanent visible incision on the face or the neck. In addition to being more cosmetically appealing, this approach is less painful and allows the procedure to be performed as an outpatient. Most patients take pain medication for only a day or two after surgery.

A sleep disorder, or somnipathy, is a medical disorder of the sleep patterns of a person or animal. Some sleep disorders are serious enough to interfere with normal physical, mental, social and emotional functioning. Polysomnography and actigraphy are tests commonly ordered for some sleep disorders.
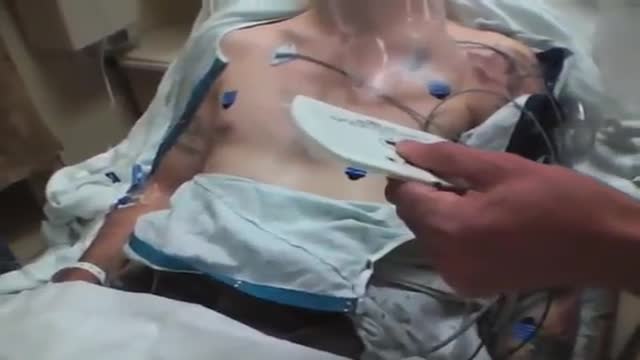
Electrical cardioversion is a procedure in which an electric current is used to reset the heart's rhythm back to its regular pattern (normal sinus rhythm). The low-voltage electric current enters the body through metal paddles or patches applied to the chest wall.

Subscribe to the Nucleus Biology channel to see new animations on biology and other science topics, plus short quizzes to ace your next exam: https://bit.ly/3lH1CzV
For Employees of Hospitals, Schools, Universities and Libraries: Download 8 FREE medical animations from Nucleus by signing up for a free trial: http://nmal.nucleusmedicalmedi....a.com/free-trial-mem
This animation by Nucleus shows you the function of plant and animal cells for middle school and high school biology, including organelles like the nucleus, nucleolus, DNA (chromosomes), ribosomes, mitochondria, etc. Also included are ATP molecules, cytoskeleton, cytoplasm, microtubules, proteins, chloroplasts, chlorophyll, cell walls, cell membrane, cilia, flagellae, etc.
0:07 What is a cell?
0:35 What are the 2 categories of cells?
1:22 What is an Organelle? DNA, Chromatin, Chromosomes
2:06 Organelles: Ribosomes, Endoplasmic Reticulum
2:59 Organelles: ER function, Vesicles, Golgi Body (Apparatus)
3:50 Organelles: Vacuole, Lysosome, Mitochondrion
4:45 Organelles: Cytoskeleton
5:04 Plant Cell Chloroplast, Cell Wall
5:43 Unique Cell Structures: Cilia
Watch another version of this video, narrated by biology teacher Joanne Jezequel here: https://youtu.be/cbiyKH9uPUw
#cell #nucleus #biology
----
Watch other Nucleus Biology videos:
- Controlled Experiments: https://youtu.be/D3ZB2RTylR4
- Independent vs. Dependent Variables: https://youtu.be/nqj0rJEf3Ew
- Active Transport: https://youtu.be/ufCiGz75DAk
----
Learn more about the company that created this video: http://www.nucleusmedicalmedia.com/
https://www.instagram.com/nucleusmedicalmedia
This animation won a Platinum Best of Show Aurora Award in 2016.
James Burke Fine DMD by James Burke Fine DMD Periodontal disease is a gum condition caused by the buildup of bacteria along and below the teeth's gumline. Acute forms are usually associated with pain from oral tissue gone bad – also known as necrotizing gingivitis or trench mouth – whereas chronic forms are painless but have a more long-term impact on your overall, systemic health. The most common chronic form is gingivitis, whose bleeding, puffiness and redness comes from an organized mass of bacteria called plaque. You may know it can advance into a form called periodontitis. If these conditions are left untreated, however, it can also lead to infections within other parts of the body, such as the lungs.