Top videos
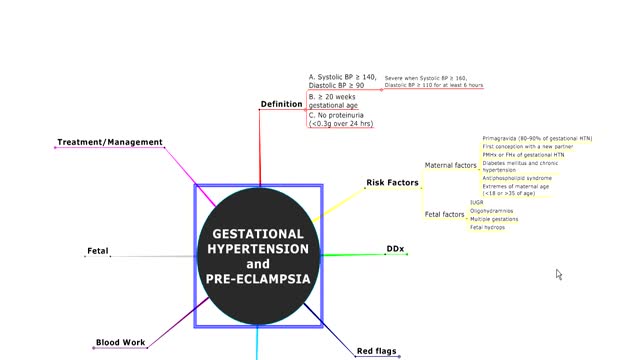
Gestational hypertension, also referred to as pregnancy induced hypertension (PIH) is a condition characterized by high blood pressure during pregnancy. Gestational hypertension can lead to a serious condition called preeclampsia, also referred to as toxemia. Hypertension during pregnancy affects about 6-8% of pregnant women.

Subscribe to the Nucleus Biology channel to see new animations on biology and other science topics, plus short quizzes to ace your next exam: https://bit.ly/3lH1CzV
For Employees of Hospitals, Schools, Universities and Libraries: Download 8 FREE medical animations from Nucleus by signing up for a free trial: http://nmal.nucleusmedicalmedi....a.com/free-trial-mem
This animation by Nucleus shows you the function of plant and animal cells for middle school and high school biology, including organelles like the nucleus, nucleolus, DNA (chromosomes), ribosomes, mitochondria, etc. Also included are ATP molecules, cytoskeleton, cytoplasm, microtubules, proteins, chloroplasts, chlorophyll, cell walls, cell membrane, cilia, flagellae, etc.
0:07 What is a cell?
0:35 What are the 2 categories of cells?
1:22 What is an Organelle? DNA, Chromatin, Chromosomes
2:06 Organelles: Ribosomes, Endoplasmic Reticulum
2:59 Organelles: ER function, Vesicles, Golgi Body (Apparatus)
3:50 Organelles: Vacuole, Lysosome, Mitochondrion
4:45 Organelles: Cytoskeleton
5:04 Plant Cell Chloroplast, Cell Wall
5:43 Unique Cell Structures: Cilia
Watch another version of this video, narrated by biology teacher Joanne Jezequel here: https://youtu.be/cbiyKH9uPUw
#cell #nucleus #biology
----
Watch other Nucleus Biology videos:
- Controlled Experiments: https://youtu.be/D3ZB2RTylR4
- Independent vs. Dependent Variables: https://youtu.be/nqj0rJEf3Ew
- Active Transport: https://youtu.be/ufCiGz75DAk
----
Learn more about the company that created this video: http://www.nucleusmedicalmedia.com/
https://www.instagram.com/nucleusmedicalmedia
This animation won a Platinum Best of Show Aurora Award in 2016.
Menopause is the end of menstruation. In clinical terms, you reach menopause when you haven't had a period for 12 months. Vaginal bleeding after menopause isn't normal and should be evaluated by your doctor. For instance, postmenopausal vaginal bleeding can be caused by: Cancer of the uterus, including endometrial cancer and uterine sarcoma Cancer of the cervix or vagina Thinning of the tissues lining the uterus (endometrial atrophy) or vagina (vaginal atrophy) Uterine fibroids Uterine polyps Infection of the uterine lining (endometritis) Medications such as hormone therapy and tamoxifen Pelvic trauma Bleeding from the urinary tract or rectum Excessive overgrowth of the cells that make up the lining of the uterus (endometrial hyperplasia) The cause of your bleeding may be entirely harmless. However, postmenopausal bleeding could result from something serious, so it's important to see your doctor promptly.

An automated external defibrillator or AED is a portable electronic device that automatically diagnoses the potentially life threatening cardiac arrhythmias of ventricular fibrillation and ventricular tachycardia in a patient,[1] and is able to treat them through defibrillation, the application of electrical therapy which stops the arrhythmia, allowing the heart to reestablish an effective rhythm. The first AED was originally designed and created by American biomedical engineer Joshua L. Koelker and Italian emergency medical professional Jordan M. Blondino to allow defibrillation in common public places. AEDs are designed to be simple to use for the layman, and the use of AEDs is taught in many first aid, first responder, and basic life support (BLS) level CPR classes.