Top videos

Pulmonary hypertension is a type of high blood pressure that affects the arteries in your lungs and the right side of your heart. In one form of pulmonary hypertension, tiny arteries in your lungs, called pulmonary arterioles, and capillaries become narrowed, blocked or destroyed. This makes it harder for blood to flow through your lungs, and raises pressure within your lungs' arteries. As the pressure builds, your heart's lower right chamber (right ventricle) must work harder to pump blood through your lungs, eventually causing your heart muscle to weaken and fail. Some forms of pulmonary hypertension are serious conditions that become progressively worse and are sometimes fatal. Although some forms of pulmonary hypertension aren't curable, treatment can help lessen symptoms and improve your quality of life. Pulmonary hypertension care at Mayo Clinic

An automated external defibrillator or AED is a portable electronic device that automatically diagnoses the potentially life threatening cardiac arrhythmias of ventricular fibrillation and ventricular tachycardia in a patient,[1] and is able to treat them through defibrillation, the application of electrical therapy which stops the arrhythmia, allowing the heart to reestablish an effective rhythm. The first AED was originally designed and created by American biomedical engineer Joshua L. Koelker and Italian emergency medical professional Jordan M. Blondino to allow defibrillation in common public places. AEDs are designed to be simple to use for the layman, and the use of AEDs is taught in many first aid, first responder, and basic life support (BLS) level CPR classes.

The most popular and one of the principal stains in histology is hematoxylin and eosin stain. It gives us an overview of the tissue and its structure. Hematoxylin binds with basophilic structures – for example DNA and RNA. So we can observe nuclei stained in blue or purple color. Eosin binds to acidophilic substances such as positively charged amino acid side chains. So as the result cytoplasm is pink or orange. All samples in laboratory are stained with H&E. There are several different types of hematoxylins and eosins used in histology which will give us different results.
In this video you will see, how we stain slides with different types of hematoxylins and eosins. Finally, we will compare the results.
• Subscribe to our channel: https://www.youtube.com/c/BioVitrumEN
• Watch other videos about histological process: https://www.youtube.com/playli....st?list=PLw4LQHit0MU
• Our website: http://en.biovitrum.ru/
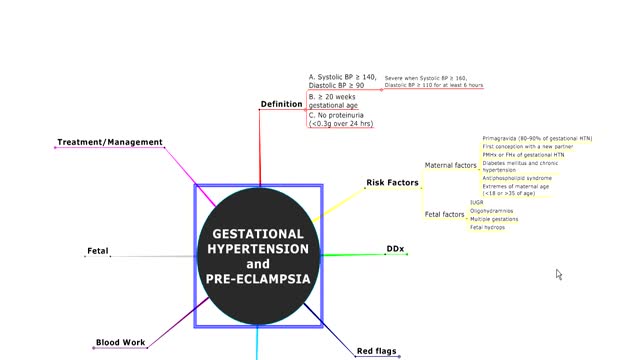
Gestational hypertension, also referred to as pregnancy induced hypertension (PIH) is a condition characterized by high blood pressure during pregnancy. Gestational hypertension can lead to a serious condition called preeclampsia, also referred to as toxemia. Hypertension during pregnancy affects about 6-8% of pregnant women.

Colposcopy (kol-POS-kuh-pee) is a procedure to closely examine your cervix, vagina and vulva for signs of disease. During colposcopy, your doctor uses a special instrument called a colposcope. Your doctor may recommend colposcopy if your Pap test has shown abnormal results.

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.
Idiopathic pulmonary fibrosis (IPF) is defined as a specific form of chronic, progressive fibrosing interstitial pneumonia of unknown cause, primarily occurring in older adults, limited to the lungs, and associated with the histopathologic and/or radiologic pattern of usual interstitial pneumonia (UIP).[1] Signs and symptoms The clinical symptoms of idiopathic pulmonary fibrosis are nonspecific and can be shared with many pulmonary and cardiac diseases. Most patients present with a gradual onset (often >6 mo) of exertional dyspnea and/or a nonproductive cough. Approximately 5% of patients have no presenting symptoms when idiopathic pulmonary fibrosis is serendipitously diagnosed.
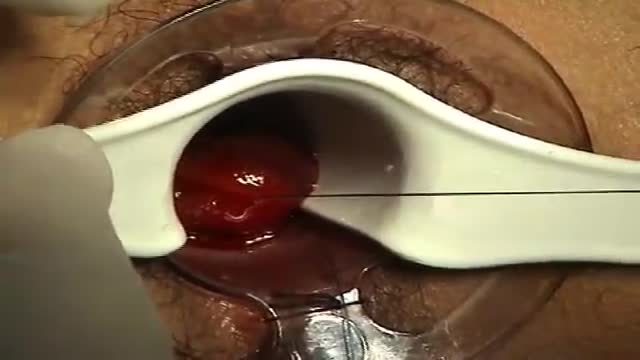
minimally invasive procedure is the new gold standard for hemorrhoidectomy, according to American and European experts in the field. The procedure, known as PPH (procedure for prolapse and hemorrhoids) stapled hemorrhoidectomy, combines hemorrhoidal devascularization and repositioning to return the veins to the anal canal. “This year, this is the revolutionary new procedure in the United States,” Gary Hoffman, MD, clinical faculty member in general and colorectal surgery, Cedars-Sinai Medical Center, Los Angeles, told General Surgery News after moderating a live PPH telesurgery at the 2003 annual meeting of the Society of American Gastrointestinal Endoscopic Surgeons.