Top videos

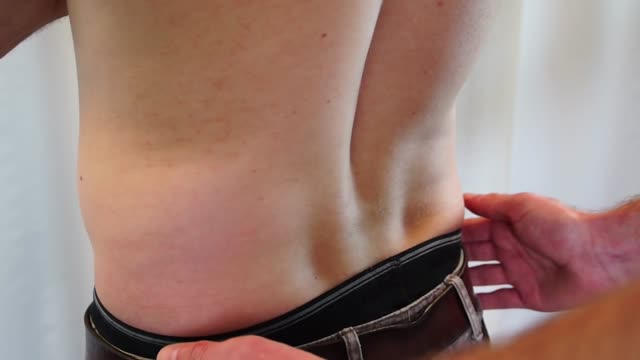
Knee replacement involves replacing a knee joint that has been damaged or worn away, usually by arthritis or injury. Find out more here: http://bit.ly/MAdfmE
The content is intended for general information only and does not replace the need for personal advice from a qualified health professional.

SSFTV is the official YouTube channel of the Seattle Science Foundation. Subscribe now to be updated on the latest videos: tinyurl.com/yt8kt8mg.
The Seattle Science Foundation is a not for profit organization dedicated to advancing the quality of patient care through education, research, innovation and technology. As a physician driven organization, we have created a trusted community of nationally recognized experts from the world’s best medical and academic institutions.
To join our upcoming meeting for CME credit, visit https://www.ssfcme.org.
Get Social With SSF:
On Instagram: https://www.instagram.com/seattlesciencefoundation
On Facebook: https://www.facebook.com/SeattleScienceFoundation
On Twitter: https://twitter.com/seattlescifdtn
On LinkedIn: https://www.linkedin.com/company/756824
On YouTube: http://www.ssfyoutube.org
Learn More at http://www.seattlesciencefoundation.org
Dr. Rod J. Oskouian, is a neurosurgeon who specializes in the diagnosis and treatment of complex spinal disorders. Dr. Oskouian is currently the Chief of Spine at the Swedish Neuroscience Institute and President and CEO of the Seattle Science Foundation. His research and clinical focus is on scoliosis, spinal deformities and anomalies, osteoporosis, spinal cord injury, degenerative disc disease, spinal oncology, stereotactic spinal radiosurgery, and minimally invasive spinal surgery. He has published in numerous medical journals and textbooks, including Neuroscience, Neurosurgery, Neurosurgical Clinics of North America, the Journal of Neurosurgery, Neurosurgical Focus and Spine.

There are many exciting milestones that accompany growing older with Down syndrome, old age can also bring unexpected challenges for which adults with Down syndrome, their families and caregivers.
www.homecareassistanceyork.com

This video shows Prof Dan Reinstein, MD MA(Cantab) FRCSC DABO FRCOphth FEBO performing a ReLEx SMILE keyhole LASIK procedure using the latest surgical instrument that he helped to develop (Malosa MMSU1297 - Reinstein Lenticule Separator: http://www.malosa.com/en/reinstein-le...). This instrument enables the procedure to be performed with one instrument, through one 2mm incision, using only one sweep per plane, and taking about 30 seconds to separate and withdraw the lenticule, improving day 1 uncorrected vision over other lenticule extraction techniques that require more corneal manipulation.
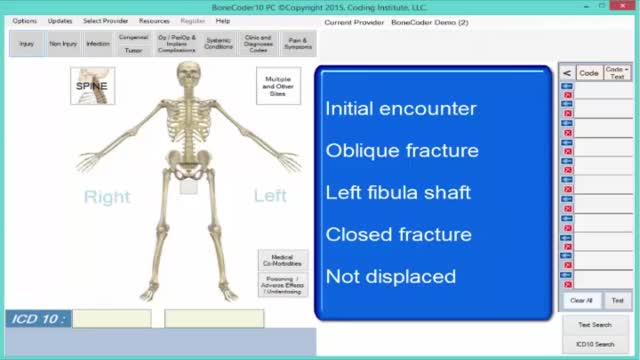
Learn to use SuperCoder’s intuitive online coding and billing tools by watching these step-by-step videos from experts. From learning how to use the ICD-10 Superbill Converter or the popular Physician Coder tool to understanding what SuperCoder’s latest launch – Intuitive Coder – is all about, our videos have you covered!
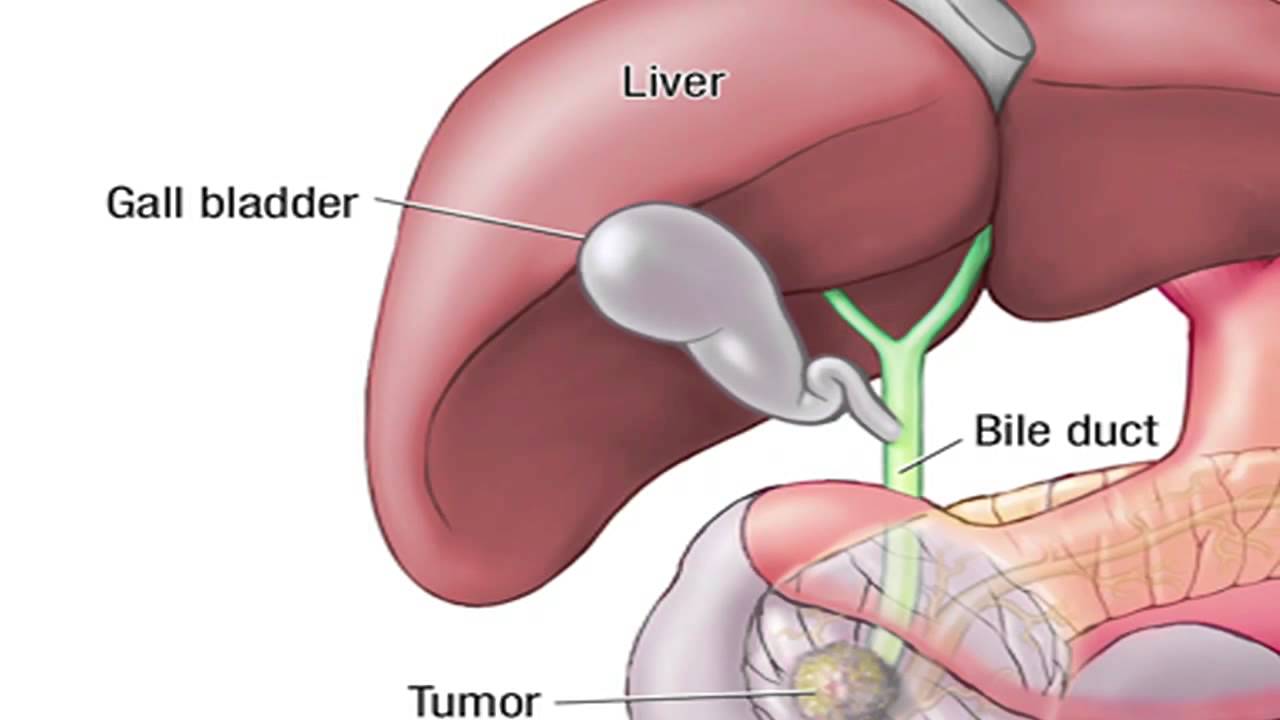
Dr. Horacio Asbun, Mayo Clinic in Florida, explains the Whipple procedure using this animated graphic of a pancreas. Cancer of the pancreas affects 45,000 people every year in the U.S., and it is the fourth leading cause of cancer-related deaths. The five-year overall survival rate if a tumor is detected early and surgically removed is 22 percent, versus 6 percent without early detection and surgery. To learn more, visit http://mayocl.in/2zk7FDi.
This video in Spanish/español: https://www.youtube.com/watch?v=N_zWboNMKWk
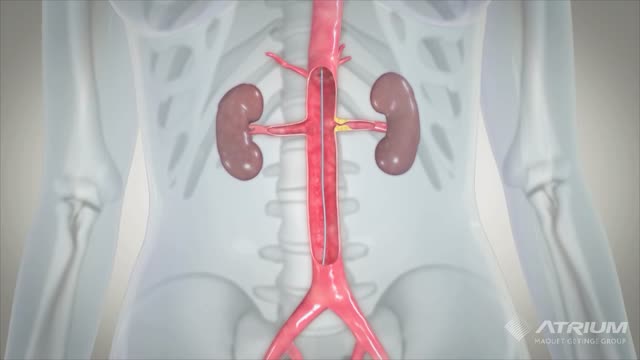
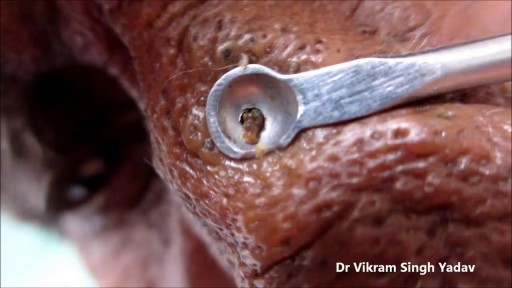
A ureteral stent, sometimes as well called ureteric stent, is a thin tube inserted into the ureter to prevent or treat obstruction of the urine flow from the kidney. The length of the stents used in adult patients varies between 24 to 30 cm.

Surgeons at The Children’s Hospital of Philadelphia were the first to perform a bilateral hand transplant on a child. Our research and work in this groundbreaking field of medicine led us to establish the Hand Transplantation Program. Combining the expertise of the Penn Transplant Institute and the Hospital’s Division of Plastic and Reconstructive Surgery and Division of Orthopedics, the program aims to improve quality of life for children who may benefit from this procedure.
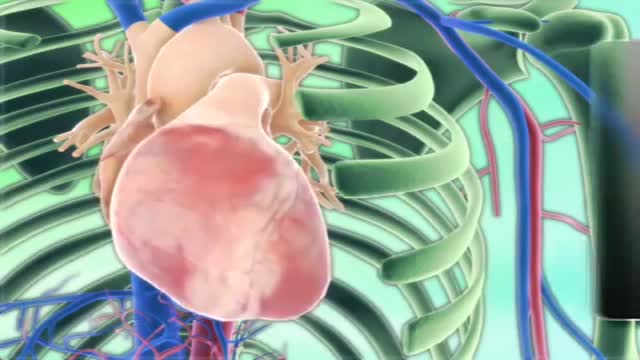
Cardiac tamponade Email this page to a friend Print Facebook Twitter Bookmark & Share Cardiac tamponade is pressure on the heart that occurs when blood or fluid builds up in the space between the heart muscle (myocardium) and the outer covering sac of the heart (pericardium). Causes In this condition, blood or fluid collects in the pericardium, the sac surrounding the heart. This prevents the heart ventricles from expanding fully. The excess pressure from the fluid prevents the heart from working properly. As a result, the body does not get enough blood. Cardiac tamponade can occur due to: Dissecting aortic aneurysm (thoracic) End-stage lung cancer Heart attack (acute MI) Heart surgery Pericarditis caused by bacterial or viral infections Wounds to the heart

Retropharyngeal abscess (RPA) produces the symptoms of sore throat, fever, neck stiffness, and stridor. RPA occurs less commonly today than in the past because of the widespread use of antibiotics for suppurative upper respiratory infections. The incidence of RPA in the United States is rising, however. Once almost exclusively a disease of children, RPA is observed with increasing frequency in adults. It poses a diagnostic challenge for the emergency physician because of its infrequent occurrence and variable presentation.