Top videos
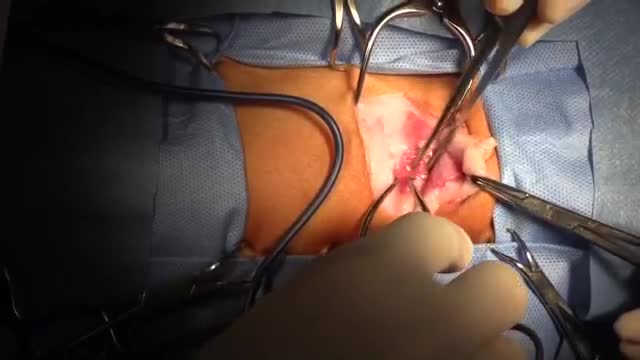
This video: Patent ductus arteriosus (PDA) is a persistent opening between two major blood vessels leading from the heart. The opening, called the ductus arteriosus, is a normal part of a baby's circulatory system before birth that usually closes shortly after birth. If it remains open, however, it's called a patent ductus arteriosus. A small patent ductus arteriosus often doesn't cause problems and might never need treatment. However, a large patent ductus arteriosus left untreated can allow poorly oxygenated blood to flow in the wrong direction, weakening the heart muscle and causing heart failure and other complications. Treatment options for a patent ductus arteriosus include monitoring, medications and closure by cardiac catheterization or surgery.

Patient Greg Grindley communicates with host Bryant Gumbel and his wife for the first time while undergoing deep brain stimulation surgery at University Hospital's Case Medical Center in Cleveland, Ohio.
➡ Subscribe: http://bit.ly/NatGeoSubscribe
About National Geographic:
National Geographic is the world's premium destination for science, exploration, and adventure. Through their world-class scientists, photographers, journalists, and filmmakers, Nat Geo gets you closer to the stories that matter and past the edge of what's possible.
Get More National Geographic:
Official Site: http://bit.ly/NatGeoOfficialSite
Facebook: http://bit.ly/FBNatGeo
Twitter: http://bit.ly/NatGeoTwitter
Instagram: http://bit.ly/NatGeoInsta
Greg's First In-Surgery Conversation | Brain Surgery Live
https://youtu.be/zvqV_2zncNU
National Geographic
https://www.youtube.com/natgeo
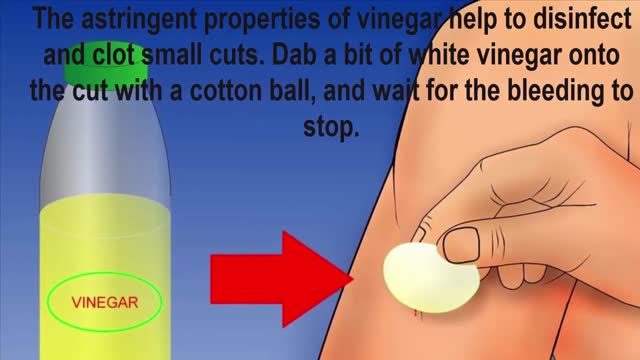
Injuries and certain medical conditions can result in bleeding. This can trigger anxiety and fear, but bleeding has a healing purpose. Still, you need to understand how to treat common bleeding incidents, like cuts and bloody noses, as well as when to seek medical help.

Erectile dysfunction (ED) is the inability to get or keep an erection firm enough for sexual function. It’s a common sexual problem, affecting as many as 30 million men in the United States. Most cases of ED have a physical cause, such as heart disease, diabetes, and obesity. Lifestyle choices like smoking and drinking excessive amounts of alcohol can also lead to ED. But for some men, psychological issues are the root of the problem.

the motor milestones expected in typically developing babies, from head control to walking and what pediatricians look for during a well-baby visit. She also explains the specific types of motor control a baby must master before the next milestone can be achieved
Sclerotherapy is a medical procedure used to eliminate varicose veins and veins. Sclerotherapy involves an injection of a solution (generally a salt solution) directly into the vein. The solution irritates the lining of the blood vessel, causing it to collapse and stick together and the blood to clot.

Medications are the most proven, effective way to treat gout symptoms. However, making certain lifestyle changes also may help, such as: Limiting alcoholic beverages and drinks sweetened with fruit sugar (fructose). Instead, drink plenty of nonalcoholic beverages, especially water. Limit intake of foods high in purines, such as red meat, organ meats and seafood. Exercising regularly and losing weight. Keeping your body at a healthy weight reduces your risk of gout.

our uterus (or womb) is normally held in place inside your pelvis with various muscles, tissue, and ligaments. Because of pregnancy, childbirth or difficult labor and delivery, in some women these muscles weaken. Also, as a woman ages and with a natural loss of the hormone estrogen, her uterus can drop into the vaginal canal, causing the condition known as a prolapsed uterus.

Renal artery stenosis is the narrowing of one or more arteries that carry blood to your kidneys (renal arteries). Narrowing of the arteries prevents normal amounts of oxygen-rich blood from reaching your kidneys. Your kidneys need adequate blood flow to help filter waste products and remove excess fluids. Reduced blood flow may increase blood pressure in your whole body (systemic blood pressure) and injure kidney tissue.
Screening is looking for cancer before a person has any symptoms. This can help find cancer at an early stage when it may be easier to treat. Lung cancer may have spread by the time a person has symptoms. One reason lung cancer is so serious is because it usually is not found until it has spread and is more difficult to treat. Screening may provide new hope for early detection and treatment of lung cancer. Scientists study screening tests to find those with the fewest risks and most benefits. They look at results over time to see if finding the cancer early decreases a person's chance of dying from the disease.

Like any syndrome, fetal alcohol syndrome (FAS) is a group of signs and symptoms that appear together and indicate a certain condition. In the case of FAS, the signs and symptoms are birth defects that result from a woman's use of alcohol during her pregnancy.
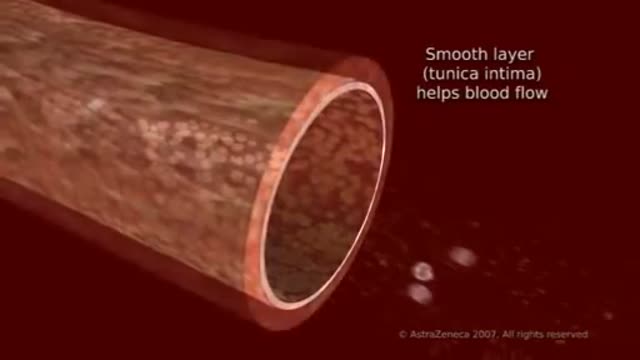
To understand high blood cholesterol (ko-LES-ter-ol), it helps to learn about cholesterol. Cholesterol is a waxy, fat-like substance that’s found in all cells of the body. Your body needs some cholesterol to make hormones, vitamin D, and substances that help you digest foods. Your body makes all the cholesterol it needs. However, cholesterol also is found in some of the foods you eat. Cholesterol travels through your bloodstream in small packages called lipoproteins (lip-o-PRO-teens). These packages are made of fat (lipid) on the inside and proteins on the outside. Two kinds of lipoproteins carry cholesterol throughout your body: low-density lipoproteins (LDL) and high-density lipoproteins (HDL). Having healthy levels of both types of lipoproteins is important. LDL cholesterol sometimes is called “bad” cholesterol. A high LDL level leads to a buildup of cholesterol in your arteries. (Arteries are blood vessels that carry blood from your heart to your body.) HDL cholesterol sometimes is called “good” cholesterol. This is because it carries cholesterol from other parts of your body back to your liver. Your liver removes the cholesterol from your body.
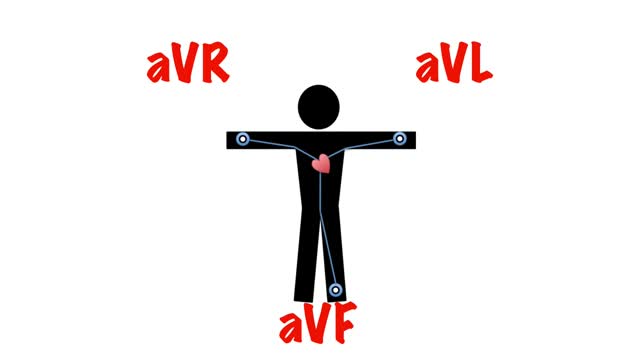
It then spreads down the bundle of his and then purkinje fibres to cause ventricular contraction. So when viewing the heart from the front, the direction of depolarisation is 11 o'clock to 5 o'clock. The general direction of depolarisation is known as the cardiac axis.
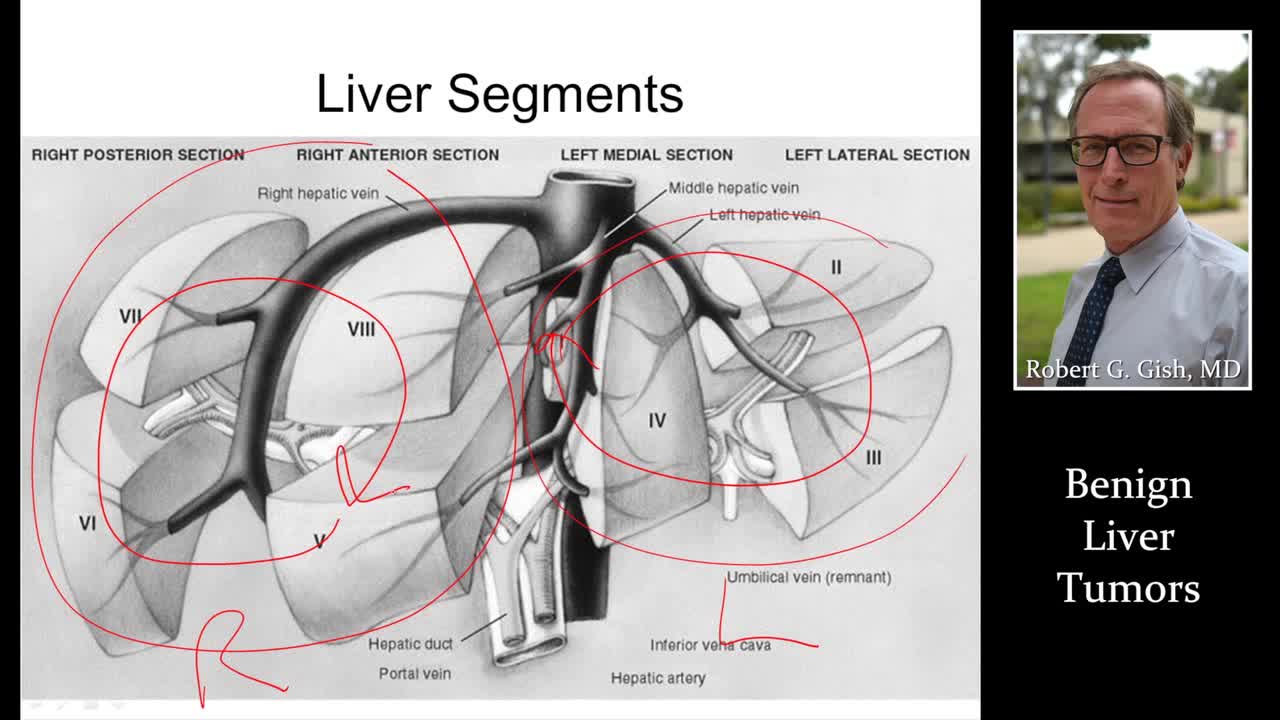
This form of liver cancer is called primary liver cancer. Noncancerous, or benign, liver tumors are common. They do not spread to other areas of the body, and they usually do not pose a serious health risk. In most cases, benign liver tumors are not detected because they cause no symptoms.

Bartter syndrome has traditionally been classified into three main clinical variants, as follows: Neonatal (or antenatal) Bartter syndrome Classic Bartter syndrome Gitelman syndrome Advances in molecular diagnostics have revealed that Bartter syndrome results from mutations in numerous genes that affect the function of ion channels and transporters that normally mediate transepithelial salt reabsorption in the distal nephron segments. Hundreds of mutations have been identified to date. Such advances may result in the development of new therapies (see the image below). [2] (See Pathophysiology and Etiology.)
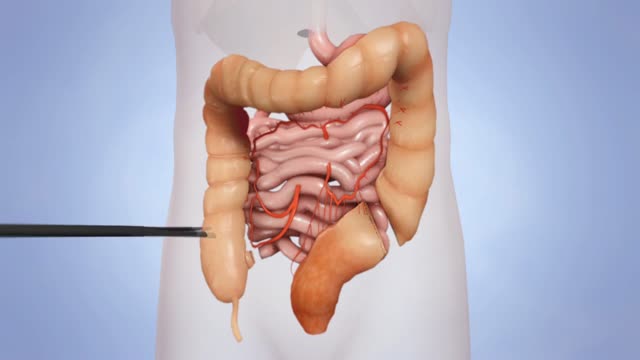
When the colon and rectum are removed (due to ulcerative colitis or familial adenomatous polyposis), another reservoir must be created for bowel contents (stool) to exit the body. Surgically creating a “J” shaped reservoir (called a J-pouch) is an option for selected patients to store and pass stool.
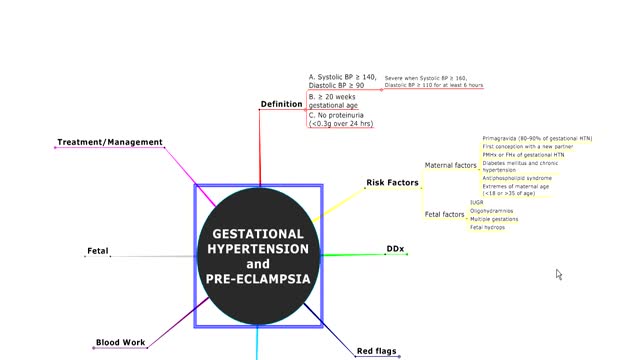
Gestational hypertension, also referred to as pregnancy induced hypertension (PIH) is a condition characterized by high blood pressure during pregnancy. Gestational hypertension can lead to a serious condition called preeclampsia, also referred to as toxemia. Hypertension during pregnancy affects about 6-8% of pregnant women.