Top videos

t’s the brain, after all, that devises experiments and interprets their results. How the brain perceives, how it makes decisions and judgments, and how those judgments can go awry are at least as important to science as knowing the intricacies of nonbiotic experimental machinery. And as any brain scientist will tell you, there’s still a long way to go before understanding the brain will get crossed off science’s to-do list. But there has been progress. A recent special issue of the journal Neuron offers a convenient set of “perspective” papers exploring the current state of understanding of the brain’s inner workings. Those papers show that a lot is known. But at the same time they emphasize that there’s a lot we don’t know.

Medical providers divide the spinal cord into four distinct regions. Knowing the region in which the injury is located is often the key to understanding diagnosis and treatment. The four spinal cord regions are: The cervical spinal cord: This is the topmost portion of the spinal cord, where the brain connects to the spinal cord, and the neck connects to the back. This region consists of eight vertebrae, commonly referred to as C1-C8. All spinal cord numbers are descending, so C1 is the highest vertebra, while C8 is the lowest in this region. The thoracic spinal cord: This section forms the middle of the spinal cord, containing twelve vertebrae numbered T1-T12. The lumbar spinal cord: This is a lower region of the spinal cord, where your spinal cord begins to bend. If you put your hand in your lower back, where your back bends inward, you're feeling your lumbar region. There are five lumbar vertebrae, numbered L1-L5.

http://yoursnoringcures.plus101.com
--Your Snoring Cures...How to Cure Snoring Naturally without Using Any Medication or Ridiculous Device!
How to Cure Snoring Naturally and Easily without Undertaking any Dangerous Surgery, Nor using any Medication or Ridiculous Device ! Doctors and Pharmaceutical Companies have tried to have my guide BANNED ...
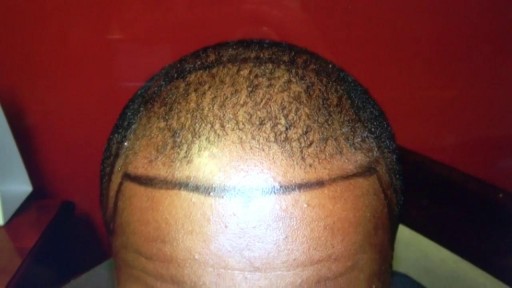
on bald hair loss man at 408-356-8600 by Dr. Diep with photos, of middle eastern man, Asian, Caucasian, Hispanic & Black, most advance hair treatment, treating male pattern baldness, bald head hair loss, receding hairline.

Current treatment is a combination of pegylated interferon-alpha-2a or pegylated interferon-alpha-2b (brand names Pegasys or PEG-Intron) and the antiviral drug ribavirin for a period of 24 or 48 weeks, depending on hepatitis C virus genotype. In a large multicenter randomized control study among genotype 2 or 3 infected patients (NORDymanIC),[35] patients achieving HCV RNA below 1000 IU/mL by day 7 who were treated for 12 weeks demonstrated similar cure rates as those treated for 24 weeks.[36][37]
Pegylated interferon-alpha-2a plus ribavirin may increase sustained virological response among patients with chronic hepatitis C as compared to pegylated interferon-alpha-2b plus ribavirin according to a systematic review of randomized controlled trials .[38] The relative benefit increase was 14.6%. For patients at similar risk to those in this study (41.0% had sustained virological response when not treated with pegylated interferon alpha 2a plus ribavirin), this leads to an absolute benefit increase of 6%. About 16.7 patients must be treated for one to benefit (number needed to treat = 16.7; click here [39] to adjust these results for patients at higher or lower risk of sustained virological response). However, this study's results may be biased due to uncertain temporality of association, selective dose response.
Treatment is generally recommended for patients with proven hepatitis C virus infection and persistently abnormal liver function tests.
Treatment during the acute infection phase has much higher success rates (greater than 90%) with a shorter duration of treatment; however, this must be balanced against the 15-40% chance of spontaneous clearance without treatment (see Acute Hepatitis C section above).
Those with low initial viral loads respond much better to treatment than those with higher viral loads (greater than 400,000 IU/mL). Current combination therapy is usually supervised by physicians in the fields of gastroenterology, hepatology or infectious disease.
The treatment may be physically demanding, particularly for those with a prior history of drug or alcohol abuse. It can qualify for temporary disability in some cases. A substantial proportion of patients will experience a panoply of side effects ranging from a 'flu-like' syndrome (the most common, experienced for a few days after the weekly injection of interferon) to severe adverse events including anemia, cardiovascular events and psychiatric problems such as suicide or suicidal ideation. The latter are exacerbated by the general physiological stress experienced by the patient.

Visit http://www.nasalcleanse.com/index.html after watching our video on nasal irrigation as a natural sinus infection remedy. Learn how & why this natural sinus remedy really works! Unlike the messy, old-fashioned neti pot or competitors with badly-designed, backflow-prone squeeze bottles that can cause sinus infection, NasalCare’s patented NasalCare® Nasal Rinse System ensures comfortable and effective delivery throughout the nasal passages, preventing sinus infection, allergy and post nasal drip. A soothing mix of sea salt and Aloe Vera extract washes away nasal irritants and the common causes of colds and flu while providing nasal congestion relief via our nasal wash. NasalCare also acts as a sinus rinse for allergy treatment. Though used for centuries in the Orient as a natural remedy and preventative measure for all sinus conditions, nasal irrigation is just catching on here. Catch us now and stop catching colds and the flu! Learn more at: http://www.nasalcleanse.com/index.html.

Visit http://www.nasalcleanse.com/index.php after watching our video on NasalCare nasal irrigation versus sinus sprays for sinusitis & sinus congestion relief. Learn how & why this natural sinus remedy really works! Unlike the temporary relief offered by chemical-laden nasal sprays, our patented NasalCare® Nasal Rinse System ensures comfortable and effective delivery throughout the nasal passages, preventing sinus infection, allergy and post nasal drip. A soothing mix of sea salt and Aloe Vera extract washes away nasal irritants and the common causes of colds and flu without the potential addiction that comes with nasal spray use. NasalCare also acts as a sinus wash for allergy treatment. Used for centuries in the Orient as a preventative measure for all sinus conditions, nasal irrigation is just catching on here. Catch us now and stop catching colds and the flu – the natural way! Order online at: http://www.nasalcleanse.com/index.php.
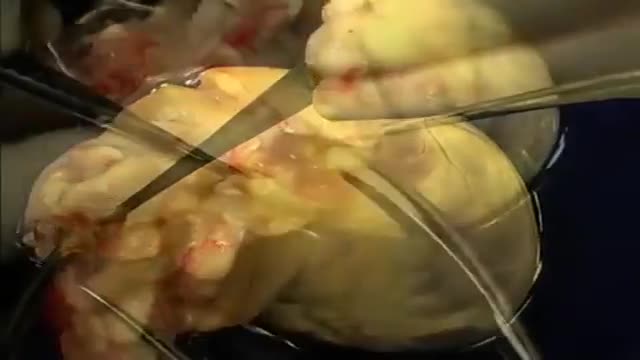
The first operation is harvesting the heart from the donor. The donor is usually an unfortunate person who has suffered irreversible brain injury, called "brain death". Very often these are patients who have had major trauma to the head, for example, in an automobile accident. The victim's organs, other than the brain, are working well with the help of medications and other "life support" that may include a respirator or other devices. A team of physicians, nurses, and technicians goes to the hospital of the donor to remove donated organs once brain death of the donor has been determined. The removed organs are transported on ice to keep them alive until they can be implanted. For the heart, this is optimally less than six hours. So, the organs are often flown by airplane or helicopter to the recipient's hospital.
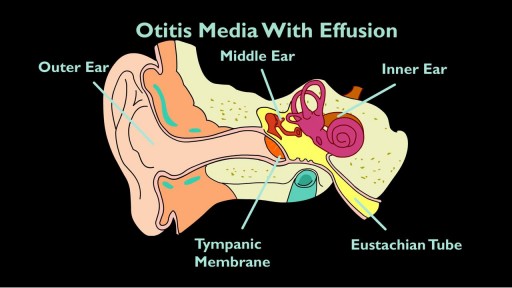
The eustachian tube drains fluid from your ears to the back of your throat. If it clogs, otitis media with effusion (OME) can occur. If you have OME, the middle part of your ear fills with fluid, which can increase the risk of ear infection. OME is very common. According to the Agency of Healthcare Research and Quality, about 90 percent of children will have OME at least once by the age of 10.
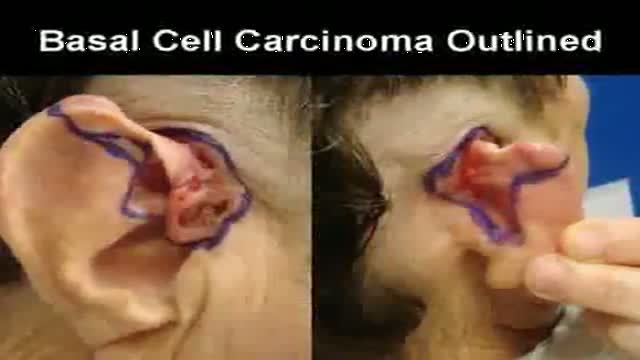
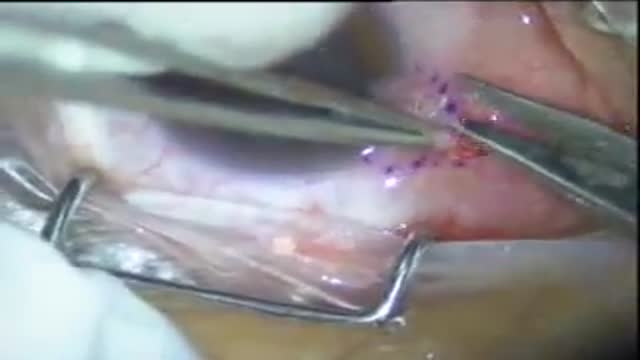
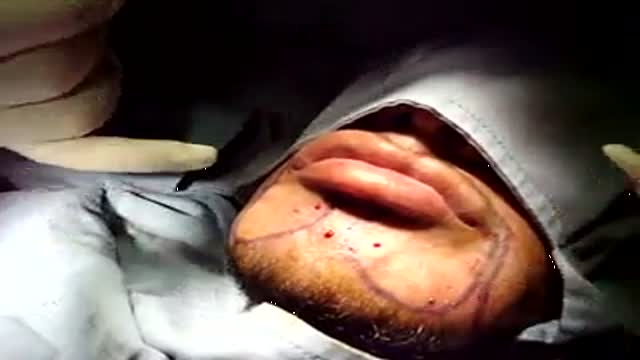
Graphic images focusing on the reconstruction of an ear after the removal of a long-standing skin cancer that this patient allowed to slowly grow over many years because he was afraid of what the surgery to remove might entail. Go to www.skincancercentre.com to learn more about the importance of the early diagnosis of skin cancer. BTW, when you put on your sunscreen, don't forget your ears, and wear a broad brimmed hat to cover this very vulnerable area of your anatomy. www.skincancercentre.com

Everyone feels sad or low sometimes, but these feelings usually pass with a little time. Depression—also called “clinical depression” or a “depressive disorder”—is a mood disorder that causes distressing symptoms that affect how you feel, think, and handle daily activities, such as sleeping, eating, or working. To be diagnosed with depression, symptoms must be present most of the day, nearly every day for at least 2 weeks.
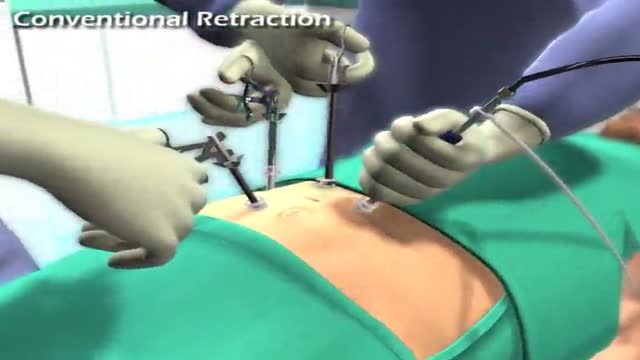
Virtual Ports, Ltd. (http://www.virtual-ports.com) is a medical device company developing and marketing instruments to improve minimally invasive laparoscopic procedures.
The EndoGrab retraction system reduces the number of ports needed for surgery by eliminating the need for traditional hand held retraction. For the surgeon, this simple solution results in the need for less auxiliary personnel, a decreased overall surgery cost, and more control over the surgery. The EndoGrab also offers added benefit to the patient who will experience less post-operative discomfort and scarring.
The EndoGrab is an internally anchored, hands-free retracting device that is introduced at the start of surgery through a 5mm trocar by means of a proprietary Applier tool. The Surgeon uses the Applier to attach the EndoGrab to both the organ requiring retraction and to the internal abdominal wall, thereby removing the organ from the operative field. The Applier is then removed and the port is free for use by other instruments.
3D video animation produced by Virtual Point Multimedia (http://virtual-point.com)

Piles Treatment
contact : drjamil79@yahoo.com
Rubber band application around the pile is a pain free procedure.Patient is put to sleep for a few minutes and can go home after a few hours.In this procedure anal fissure was also treated with the transparent anoscope that comes with the PPH gun set.
Piles Treatment piles: HAL Hemorrhoidal Artery Ligation new fast and painless treatment of haemorrhoids dr jamil ahmad hashmi -PainlessRubber band application around the pile is pain free procedure.Patient put to sleep for few minutes can go home after hours.In this procedure anal fissure was also treated with transparent anoscope that comes PPH gun set. Category: health