Top videos

Thoracentesis is a minimally invasive procedure used to diagnose and treat pleural effusions, a condition in which there is excess fluid in the pleural space, also called the pleural cavity. This space exists between the outside of the lungs and the inside of the chest wall.

A water birth means at least part of your labor, delivery, or both happen while you’re in a birth pool filled with warm water. It can take place in a hospital, a birthing center, or at home. A doctor, nurse-midwife, or midwife helps you through it. In the U.S., some birthing centers and hospitals offer water births. Birthing centers are medical facilities that offer a more homelike setting than a hospital and more natural options for women having babies. The use of a birthing pool during the first stage of labor might: Help ease pain Keep you from needing anesthesia Speed up your labor The American College of Obstetricians and Gynecologists (ACOG), which sets guidelines for pregnancy and childbirth care in the U.S., says a water birth during the first stage of labor may have some benefits but delivering your baby underwater should be considered an experimental procedure with risks. The first stage is from when contractions start until your cervix is fully dilated.
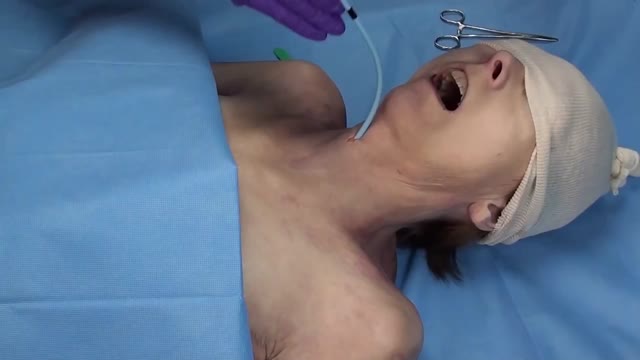
A cricothyrotomy (also called crike, thyrocricotomy, cricothyroidotomy, inferior laryngotomy, intercricothyrotomy, coniotomy or emergency airway puncture) is an incision made through the skin and cricothyroid membrane to establish a patent airway during certain life-threatening situations, such as airway obstruction by ...

What is a brain aneurysm? A brain (cerebral) aneurysm is a bulging, weak area in the wall of an artery that supplies blood to the brain. In most cases, a brain aneurysm causes no symptoms and goes unnoticed. In rare cases, the brain aneurysm ruptures, releasing blood into the skull and causing a stroke. When a brain aneurysm ruptures, the result is called a subarachnoid hemorrhage. Depending on the severity of the hemorrhage, brain damage or death may result.
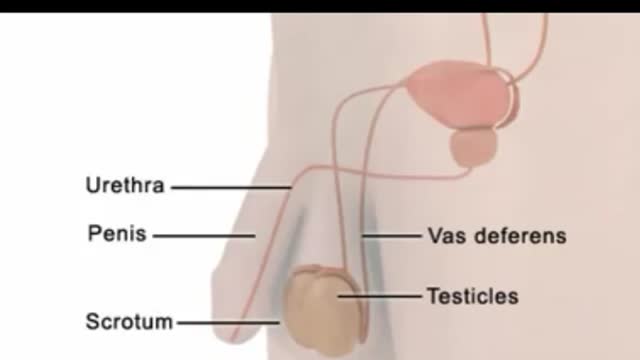
An egg cannot be fertilized when there are no sperm in the semen. The testicles continue to produce sperm, but the sperm are reabsorbed by the body. (This also happens to sperm that are not ejaculated after a while, regardless of whether you have had a vasectomy.) Sperm are made in the testicles. They pass through two tubes called the vasa deferentia to other glands and mix with seminal fluids to form semen. Vasectomy blocks each vas deferens and keeps sperm out of the seminal fluid. The sperm are absorbed by the body instead of being ejaculated.
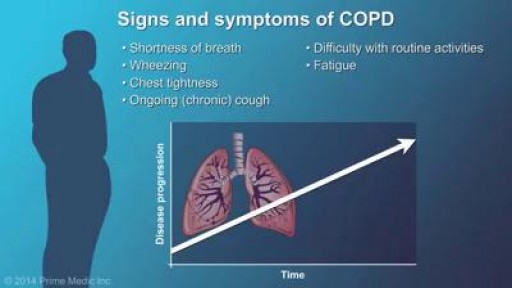
COPD stands for chronic obstructive pulmonary (lung) disease. COPD is a term applied to a family of diseases that includes emphysema, chronic bronchitis, and emphysema due to alpha-1 antitrypsin deficiency. COPD usually progresses gradually, causing limited airflow in and out of the lungs. COPD adds to the work of the heart. Diseased lungs might reduce the amount of oxygen that goes to the blood. High blood pressure in blood vessels from the heart to the lungs makes it difficult for the heart to pump. Lung disease can also cause the body to produce too many red blood cells, which might make the blood thicker and harder to pump.
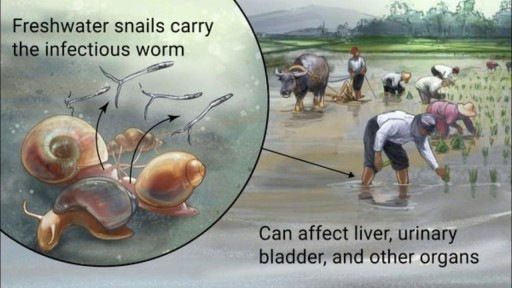
Schistosomiasis is a parasitic disease caused by flukes (trematodes) of the genus Schistosoma. After malaria and intestinal helminthiasis, schistosomiasis is the third most devastating tropical disease in the world, being a major source of morbidity and mortality for developing countries in Africa, South America, the Caribbean, the Middle East, and Asia. (See Epidemiology and Prognosis.) [1] More than 207 million people, 85% of who live in Africa, are infected with schistosomiasis, [1] and an estimated 700 million people are at risk of infection in 76 countries where the disease is considered endemic, as their agricultural work, domestic chores, and recreational activities expose them to infested water. [1, 2] Globally, 200,000 deaths are attributed to schistosomiasis annually. [3] Transmission is interrupted in some countries. [2] (See Etiology and Epidemiology.)
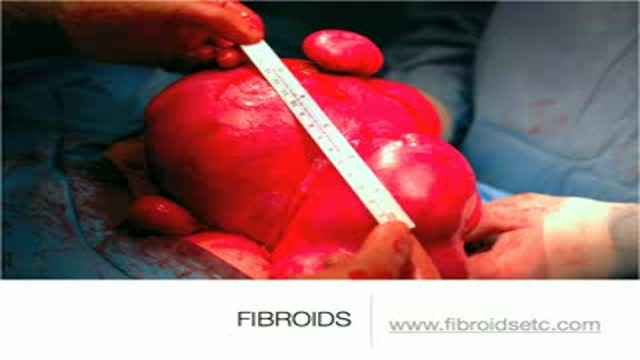
A uterine fibroid (also uterine leiomyoma, myoma, fibromyoma, leiofibromyoma, fibroleiomyoma, and fibroma) (plural of ... myoma is ...myomas or ...myomata) is a benign (non-cancerous) tumor that originates from the smooth muscle layer (myometrium) and the accompanying connective tissue of the uterus. Fibroids are the most common benign tumors in females and typically found during the middle and later reproductive years. While most fibroids are asymptomatic, they can grow and cause heavy and painful menstruation, painful sexual intercourse, and urinary frequency and urgency. Uterine fibroids is the major indication for hysterectomy in the US.[2] Fibroids are often multiple and if the uterus contains too many leiomyomatas to count, it is referred to as uterine leiomyomatosis. The malignant version of a fibroid is uncommon and termed a leiomyosarcoma.