Top videos
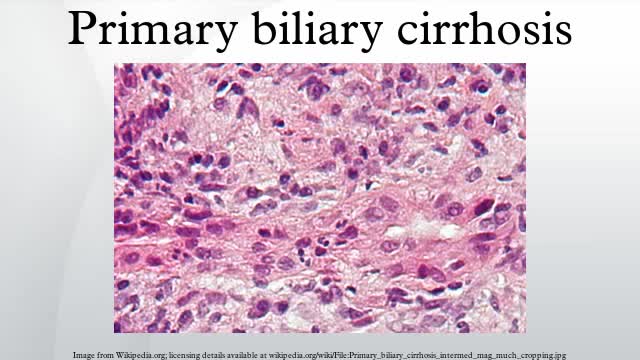
Primary biliary cirrhosis, sometimes called PBC, is a disease in which the bile ducts in your liver are slowly destroyed. Bile, a fluid produced in your liver, plays a role in digesting food and helps rid your body of worn-out red blood cells, cholesterol and toxins. When bile ducts are damaged, as in primary biliary cirrhosis, harmful substances can build up in your liver and sometimes lead to irreversible scarring of liver tissue (cirrhosis). Primary biliary cirrhosis is considered an autoimmune disease, in which the body turns against its own cells. Researchers think it is triggered by a combination of genetic and environmental factors. Primary biliary cirrhosis usually develops slowly and medication can slow its progression, especially if treatment begins early.

SSFTV is the official YouTube channel of the Seattle Science Foundation. Subscribe now to be updated on the latest videos: tinyurl.com/yt8kt8mg.
The Seattle Science Foundation is a not for profit organization dedicated to advancing the quality of patient care through education, research, innovation and technology. As a physician driven organization, we have created a trusted community of nationally recognized experts from the world’s best medical and academic institutions.
To join our upcoming meeting for CME credit, visit https://www.ssfcme.org.
Get Social With SSF:
On Instagram: https://www.instagram.com/seattlesciencefoundation
On Facebook: https://www.facebook.com/SeattleScienceFoundation
On Twitter: https://twitter.com/seattlescifdtn
On LinkedIn: https://www.linkedin.com/company/756824
On YouTube: http://www.ssfyoutube.org
Learn More at http://www.seattlesciencefoundation.org
Dr. Rod J. Oskouian, is a neurosurgeon who specializes in the diagnosis and treatment of complex spinal disorders. Dr. Oskouian is currently the Chief of Spine at the Swedish Neuroscience Institute and President and CEO of the Seattle Science Foundation. His research and clinical focus is on scoliosis, spinal deformities and anomalies, osteoporosis, spinal cord injury, degenerative disc disease, spinal oncology, stereotactic spinal radiosurgery, and minimally invasive spinal surgery. He has published in numerous medical journals and textbooks, including Neuroscience, Neurosurgery, Neurosurgical Clinics of North America, the Journal of Neurosurgery, Neurosurgical Focus and Spine.

There's a small area called the Grafenberg spot, or G-spot, inside the vagina. It's located about an inch or so inside the vaginal opening on the upper vaginal wall — closest to the bellybutton. The G-spot is sexually sensitive and swells slightly during arousal and feels raised or bumpy
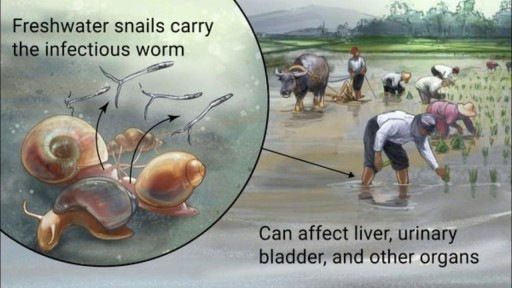
Schistosomiasis is a parasitic disease caused by flukes (trematodes) of the genus Schistosoma. After malaria and intestinal helminthiasis, schistosomiasis is the third most devastating tropical disease in the world, being a major source of morbidity and mortality for developing countries in Africa, South America, the Caribbean, the Middle East, and Asia. (See Epidemiology and Prognosis.) [1] More than 207 million people, 85% of who live in Africa, are infected with schistosomiasis, [1] and an estimated 700 million people are at risk of infection in 76 countries where the disease is considered endemic, as their agricultural work, domestic chores, and recreational activities expose them to infested water. [1, 2] Globally, 200,000 deaths are attributed to schistosomiasis annually. [3] Transmission is interrupted in some countries. [2] (See Etiology and Epidemiology.)
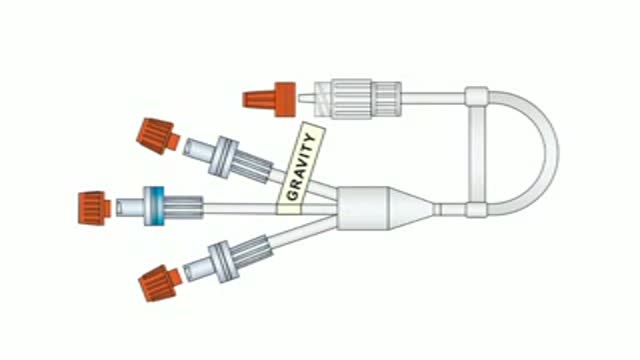
To facilitate the delivery of fluids during labour, obstetric anaesthetists from Coventry designed a triple IV peripheral connector with a central high-flow anti-reflux valve. This connector, now rightly known as the Coventry valve, can be used for all theatre settings and is especially useful in obstetrics, ICU, HDU and orthopaedics. More details on www.mediplus.co.uk
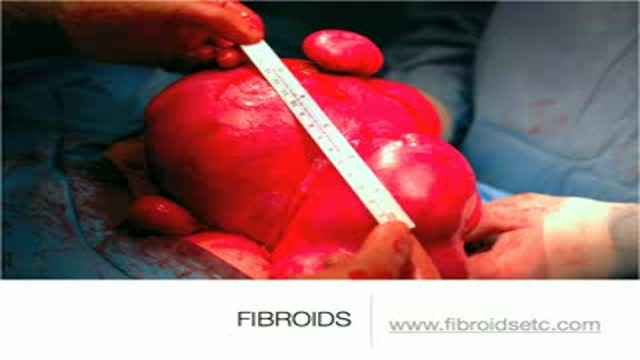
A uterine fibroid (also uterine leiomyoma, myoma, fibromyoma, leiofibromyoma, fibroleiomyoma, and fibroma) (plural of ... myoma is ...myomas or ...myomata) is a benign (non-cancerous) tumor that originates from the smooth muscle layer (myometrium) and the accompanying connective tissue of the uterus. Fibroids are the most common benign tumors in females and typically found during the middle and later reproductive years. While most fibroids are asymptomatic, they can grow and cause heavy and painful menstruation, painful sexual intercourse, and urinary frequency and urgency. Uterine fibroids is the major indication for hysterectomy in the US.[2] Fibroids are often multiple and if the uterus contains too many leiomyomatas to count, it is referred to as uterine leiomyomatosis. The malignant version of a fibroid is uncommon and termed a leiomyosarcoma.
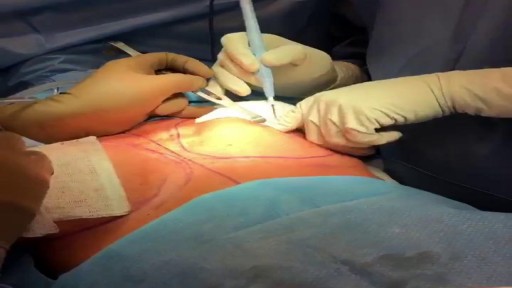
This anatomical implant was originally placed in 1997. Due to the dark yellow color inside the implant it is clear the implant has been ruptured for quite some time. When implants rupture, it is important to have them replaced as soon as possible to avoid excessive scarring in the breasts. If too much scar tissue has accumulated around the deflated implant, it becomes difficult to create a normal breast shape in the future. Therefor its important to know the signs of a ruptured implant such as, painful to touch, visible asymmetry or loss of integrity to the bag. Dr. Stuart Linder 9675 Brighton Way Suite 420 Beverly Hills, CA 90210

Otto Placik MD. a board certified Chicago Illinois based plastic surgeon presents instructional video on post genital surgery (labia minora reduction aka labiaplasty or labioplasty or clitoral hood reduction) massage exercises for treatment of labum minora psot surgical fibrosis or hypersensitivity. Photos pictures and video of anatomic models are reviewed . Great for patients thinking about or planning labiaplasty or vaginal cosmetic surgery

What is a brain aneurysm? A brain (cerebral) aneurysm is a bulging, weak area in the wall of an artery that supplies blood to the brain. In most cases, a brain aneurysm causes no symptoms and goes unnoticed. In rare cases, the brain aneurysm ruptures, releasing blood into the skull and causing a stroke. When a brain aneurysm ruptures, the result is called a subarachnoid hemorrhage. Depending on the severity of the hemorrhage, brain damage or death may result.
In caring for patients who are critically ill, access to the central venous circulation is important. Central venous access allows the placement of various types of intravenous (IV) lines to facilitate the infusion of fluids, blood products, and drugs and to obtain blood for laboratory analysis. It is also an essential procedure in patients in whom placement of a line in a peripheral vein is impossible. A central line may be the only means of venous access in such cases.