Top videos
We are looking for 5 patients with knee pain who want to get significantly better in the next 30 days. Click this link to let me know you're interested and learn more.
https://www.drdavidgeier.com/work-with-me/contact/
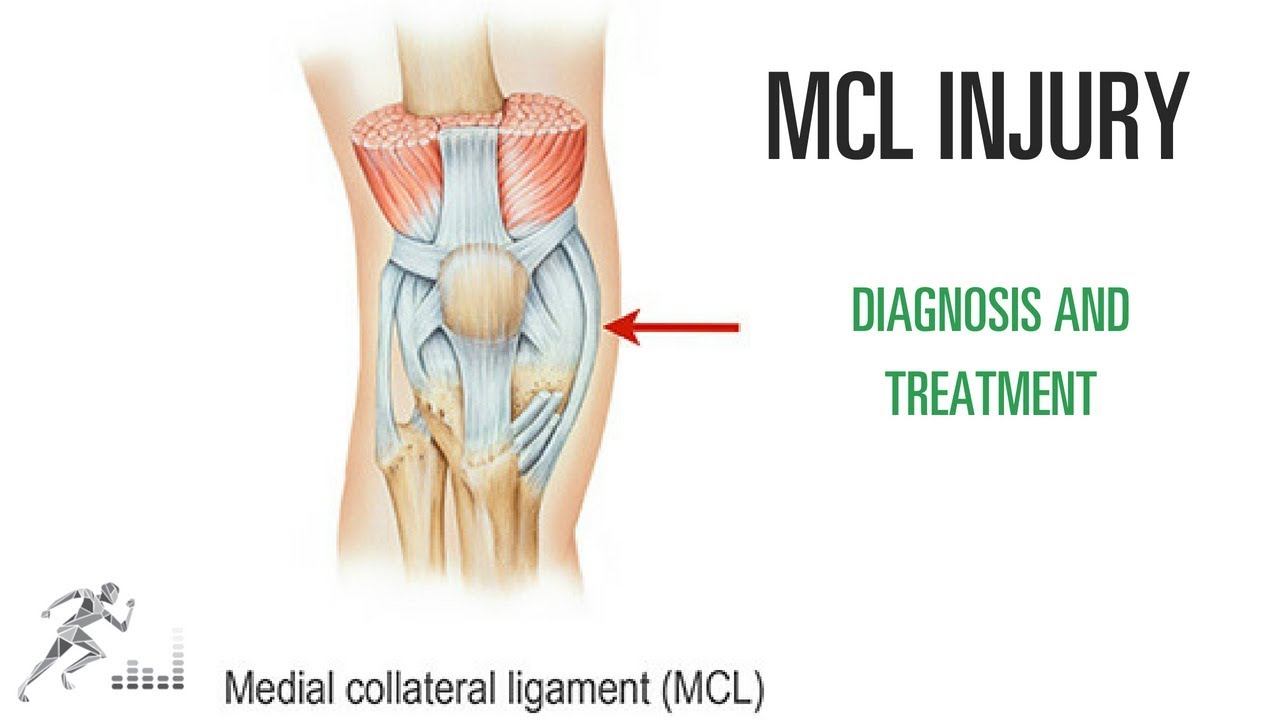
One of the most common knee injuries in contact and collision sports is a medial collateral ligament (MCL) injury. This is a ligament on the medial (side closest to the midline) side of your knee that provides stability against side-to-side stress to the knee. You might injure it by cutting maneuvers in sports like soccer or hockey. You can also suffer an MCL injury if another player hits you on the outside of your knee.
Please note: I don't respond to questions and requests for specific medical advice left in the comments to my videos. I receive too many to keep up (several hundred per week), and legally I can't offer specific medical advice to people who aren't my patients (see below). If you want to ask a question about a specific injury you have, leave it in the comments below, and I might answer it in an upcoming Ask Dr. Geier video. If you need more detailed information on your injury, go to my Resources page: https://www.drdavidgeier.com/resources/
The content of this YouTube Channel, https://www.youtube.com/user/drdavidgeier (“Channel”) is for INFORMATIONAL PURPOSES ONLY. The Channel may offer health, fitness, nutritional and other such information, but such information is intended for educational and informational purposes only. This content should not be used to self-diagnose or self-treat any health, medical, or physical condition. The content does not and is not intended to convey medical advice and does not constitute the practice of medicine. YOU SHOULD NOT RELY ON THIS INFORMATION AS A SUBSTITUTE FOR, NOR DOES IT REPLACE, PROFESSIONAL MEDICAL ADVICE, DIAGNOSIS, OR TREATMENT. You should consult with your healthcare professional before doing anything contained on this Channel. You agree that Dr. Geier is not responsible for any actions or inaction on your part based on the information that is presented on the Channel. Dr. David Geier Enterprises, LLC makes no representations about the accuracy or suitability of the content. USE OF THE CONTENT IS AT YOUR OWN RISK.
Unlike tears of the ACL, MCL injuries most often heal without surgery. You might need to wear a hinged knee brace for 2-6 weeks. The length of time you miss from sports or exercise varies depending on the location and severity of the injury.
In this video, I share my thoughts on the nature of an MCL injury, the diagnosis, the treatment options and return to sports.
Please remember, while I appreciate your questions, I cannot and will not offer specific medical advice by email, online, on my show, or in the comments at the end of these posts. My responses are meant to provide general medical information and education. Please consult your physician or health care provider for your specific medical concerns.

During your menstrual period, your uterus contracts to help expel its lining. Hormonelike substances (prostaglandins) involved in pain and inflammation trigger the uterine muscle contractions. Higher levels of prostaglandins are associated with more-severe menstrual cramps.
This video: Blisters caused by friction or minor burns do not require a doctor's care. New skin will form underneath the affected area and the fluid is simply absorbed. Do not puncture a blister unless it is large, painful, or likely to be further irritated. The fluid-filled blister keeps the underlying skin clean, which prevents infection and promotes healing.
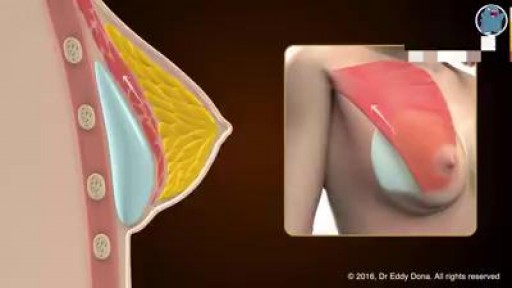
Endoscopy of Mammary Ducts with Micro-Endoscope called Mammary Ductoscopy. Indication:- Nipple Discharge. In this case Papilloma seen quite clearly. Biopsy can also be possible with Ductoscopy. Mammary Ductoscopy is very useful for diagnosis of Breast Cancer in early stage.

This video clip shows an upper track endoscopy of A 75 year-old female, presented with severe adominal pain since three days. Endoscopy displays a deep ulcer at the lesser curvature of the stomach. This patient has a klatskin´s tumor (bile duct bifurcation).

Following Dr. Eric Skarsgard on his grueling 19-hour day at BC Children's Hospital, we meet several of his patients -- some of who need surgery that day, and some who have chronic conditions and need regular check-ups with him -- and learn how he works with medical students and on research projects as time allows.

This covers some of the benefits, side effects and potential complications of LASIK Eye Surgery! Learn about the pros and cons of laser eye surgery and some pro tools to help you along the way.
📒 Show Notes and Resources 📒
LASIK Affordability Calculator
http://www.refractivealliance.....com/lasik-affordabil
Patient Guide to Refractive Surgery
https://www.aao.org/Assets/e89....0eb55-9bfa-465a-8422
Some Reference Articles for you folks who like to read
https://www.healio.com/ophthal....mology/journals/jrs/
Dry Eye Playlist
https://www.youtube.com/playli....st?list=PLzi60fSuOmP
---------My Cameras and Video Gear -------
https://kit.co/DoctorEyeHealth
DISCLAIMER: Some of the links in this description are "affiliate links", a link with a special tracking code. This means if you click on an affiliate link and purchase the item, I may receive an affiliate commission. Regardless, I only recommend products or services I believe will add value to viewers.
======================================================
Let’s Connect! Dr. Allen on Social Media:
https://instagram.com/doctoreyehealth
https://www.facebook.com/doctoreyehealth
https://twitter.com/doctoreyehealth
For Collaborations please email me: DoctorEyehealth@gmail.com
MEDICAL ADVICE DISCLAIMER: All content in this video and description including: information, opinions, content, references and links is for informational purposes only. The Author does not provide any medical advice on the Site. Accessing, viewing, reading or otherwise using this content does NOT create a physician-patient relationship between you and it’s author. Providing personal or medical information to the Principal author does not create a physician-patient relationship between you and the Principal author or authors. Nothing contained in this video or it’s description is intended to establish a physician-patient relationship, to replace the services of a trained physician or health care professional, or otherwise to be a substitute for professional medical advice, diagnosis, or treatment. You should consult a licensed physician or appropriately-credentialed health care worker in your community in all matters relating to your health.
About:
In this video you will find a laser eye surgery review. We cover the laser eye surgery procedure and how lasik eye surgery works. A large emphasis is on the benefits of laser eye surgery as well as potential side effects and complications. We even touch on the topic of lasik eye surgery gone wrong.
#lasikeyesurgery #lasiksurgery #lasik

If you have an active lifestyle or are often on the go with work, travel or family, then peritoneal dialysis at home may be the right choice. Home peritoneal dialysis offers additional freedom and flexibility as a treatment option that’s closest to natural kidney function and may require fewer dietary restrictions and medications. To learn more about Home PD, visit https://www.FreseniusKidneyCar....e.com/ckd-treatment/
Subscribe to Our YouTube Channel
Subscribe Here: https://www.youtube.com/c/Fres....eniusKidneyCareOffic
Find Fresenius Kidney Care Online at:
Website: https://www.freseniuskidneycare.com/
Facebook:@FreseniusKidneyCare
https://www.facebook.com/FreseniusKidneyCare/
Twitter: @FreseniusKC
https://twitter.com/freseniuskc
Pinterest: Fresenius Kidney Care
https://www.pinterest.com/FreseniusKidneyCarePins/