Top videos

Acute sinusitis can be triggered by a cold or allergies and may resolve on its own. Chronic sinusitis lasts up to eight weeks and may be caused by an infection or growths. Symptoms include headache, facial pain, runny nose, and nasal congestion. Acute sinusitis usually doesn't require any treatment beyond symptomatic relief with pain medications, nasal decongestants, and nasal saline rinses. Chronic sinusitis may require antibiotics.
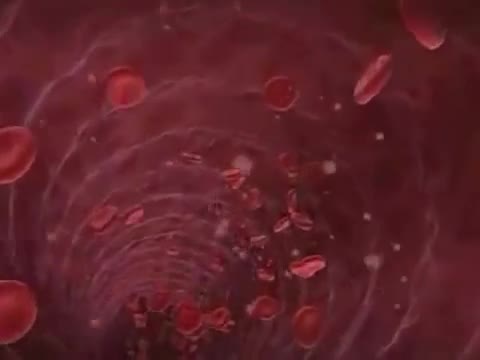
Sickle cell anemia (sickle cell disease) is a disorder of the blood caused by an inherited abnormal hemoglobin (the oxygen-carrying protein within the red blood cells). The abnormal hemoglobin causes distorted (sickled) red blood cells.
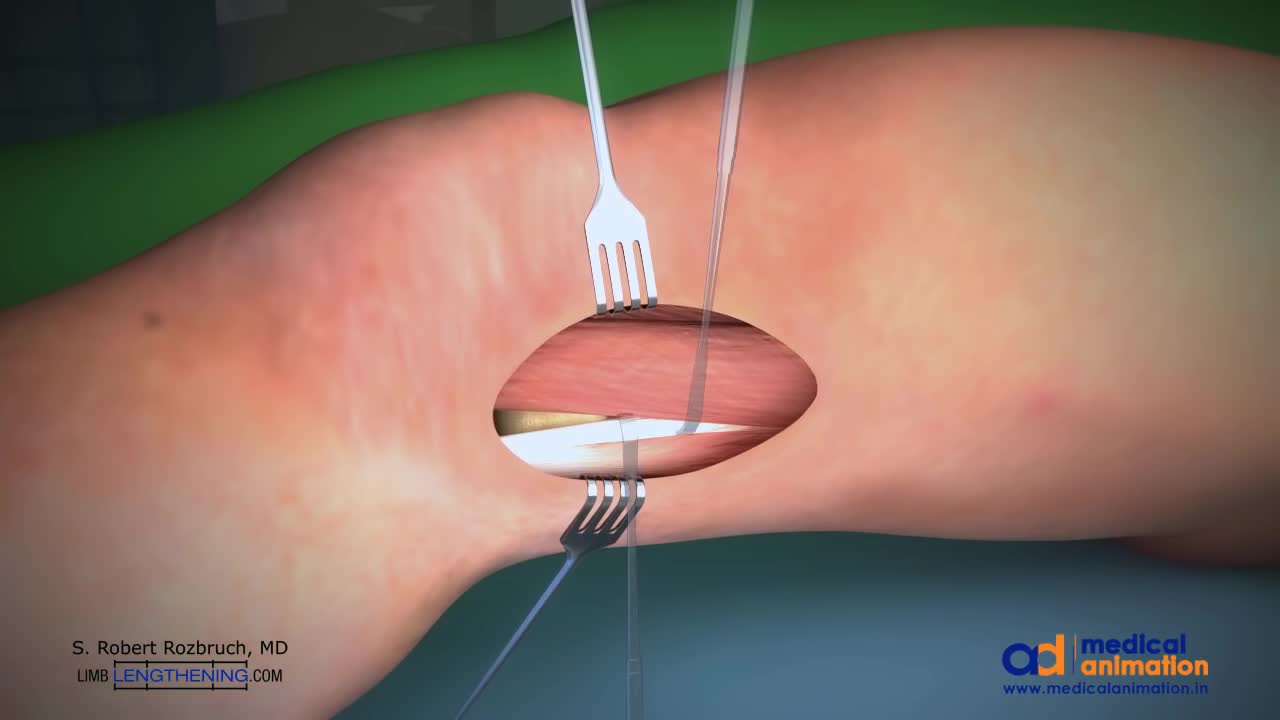
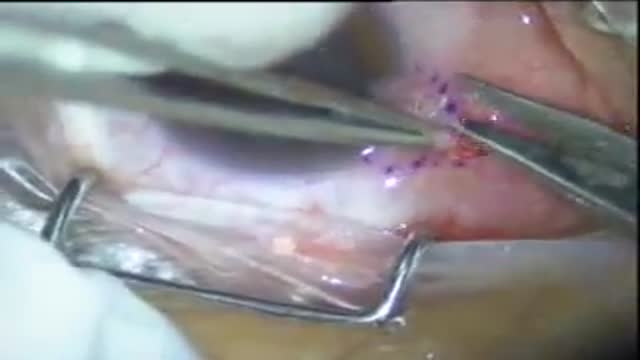
The Distal Femoral Osteotomy System utilizes the same principles of design featured in the Tibial Osteotomy System. Specifically designed femoral osteotomy plates take into account the anatomical differences between the distal femur and proximal tibia.
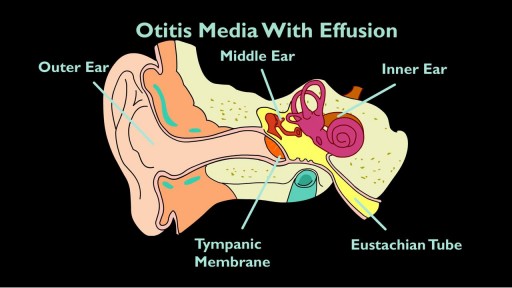
The eustachian tube drains fluid from your ears to the back of your throat. If it clogs, otitis media with effusion (OME) can occur. If you have OME, the middle part of your ear fills with fluid, which can increase the risk of ear infection. OME is very common. According to the Agency of Healthcare Research and Quality, about 90 percent of children will have OME at least once by the age of 10.

http://yoursnoringcures.plus101.com
--Your Snoring Cures...How to Cure Snoring Naturally without Using Any Medication or Ridiculous Device!
How to Cure Snoring Naturally and Easily without Undertaking any Dangerous Surgery, Nor using any Medication or Ridiculous Device ! Doctors and Pharmaceutical Companies have tried to have my guide BANNED ...
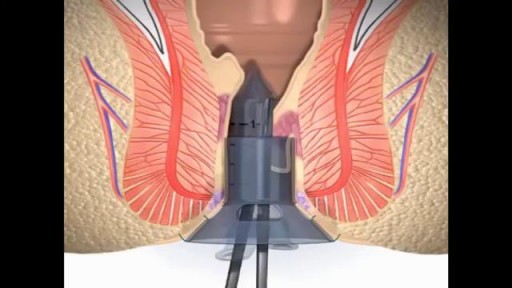
Stapling is used to treat prolapsed hemorrhoids. A surgical staple fixes the prolapsed hemorrhoid back into place inside your rectum and cuts off the blood supply so that the tissue will shrink and be reabsorbed. Stapling recovery takes less time and is less painful than recovery from a hemorrhoidectomy.
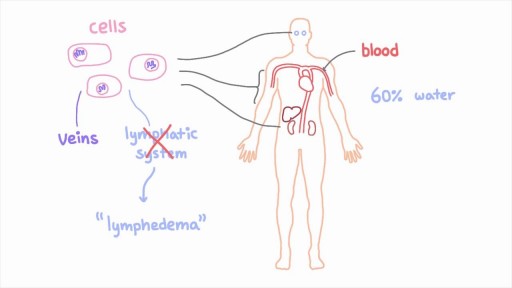
The lymphatic system is a network of specialized vessels (lymph vessels) throughout the body whose purpose is to collect excess lymph fluid with proteins, lipids, and waste products from the tissues. This fluid is then carried to the lymph nodes, which filter waste products and contain infection-fighting cells called lymphocytes. The excess fluid in the lymph vessels is eventually returned to the bloodstream. When the lymph vessels are blocked or unable to carry lymph fluid away from the tissues, localized swelling (lymphedema) is the result.

Current treatment is a combination of pegylated interferon-alpha-2a or pegylated interferon-alpha-2b (brand names Pegasys or PEG-Intron) and the antiviral drug ribavirin for a period of 24 or 48 weeks, depending on hepatitis C virus genotype. In a large multicenter randomized control study among genotype 2 or 3 infected patients (NORDymanIC),[35] patients achieving HCV RNA below 1000 IU/mL by day 7 who were treated for 12 weeks demonstrated similar cure rates as those treated for 24 weeks.[36][37]
Pegylated interferon-alpha-2a plus ribavirin may increase sustained virological response among patients with chronic hepatitis C as compared to pegylated interferon-alpha-2b plus ribavirin according to a systematic review of randomized controlled trials .[38] The relative benefit increase was 14.6%. For patients at similar risk to those in this study (41.0% had sustained virological response when not treated with pegylated interferon alpha 2a plus ribavirin), this leads to an absolute benefit increase of 6%. About 16.7 patients must be treated for one to benefit (number needed to treat = 16.7; click here [39] to adjust these results for patients at higher or lower risk of sustained virological response). However, this study's results may be biased due to uncertain temporality of association, selective dose response.
Treatment is generally recommended for patients with proven hepatitis C virus infection and persistently abnormal liver function tests.
Treatment during the acute infection phase has much higher success rates (greater than 90%) with a shorter duration of treatment; however, this must be balanced against the 15-40% chance of spontaneous clearance without treatment (see Acute Hepatitis C section above).
Those with low initial viral loads respond much better to treatment than those with higher viral loads (greater than 400,000 IU/mL). Current combination therapy is usually supervised by physicians in the fields of gastroenterology, hepatology or infectious disease.
The treatment may be physically demanding, particularly for those with a prior history of drug or alcohol abuse. It can qualify for temporary disability in some cases. A substantial proportion of patients will experience a panoply of side effects ranging from a 'flu-like' syndrome (the most common, experienced for a few days after the weekly injection of interferon) to severe adverse events including anemia, cardiovascular events and psychiatric problems such as suicide or suicidal ideation. The latter are exacerbated by the general physiological stress experienced by the patient.

Visit http://www.nasalcleanse.com/index.html after watching our video on nasal irrigation as a natural sinus infection remedy. Learn how & why this natural sinus remedy really works! Unlike the messy, old-fashioned neti pot or competitors with badly-designed, backflow-prone squeeze bottles that can cause sinus infection, NasalCare’s patented NasalCare® Nasal Rinse System ensures comfortable and effective delivery throughout the nasal passages, preventing sinus infection, allergy and post nasal drip. A soothing mix of sea salt and Aloe Vera extract washes away nasal irritants and the common causes of colds and flu while providing nasal congestion relief via our nasal wash. NasalCare also acts as a sinus rinse for allergy treatment. Though used for centuries in the Orient as a natural remedy and preventative measure for all sinus conditions, nasal irrigation is just catching on here. Catch us now and stop catching colds and the flu! Learn more at: http://www.nasalcleanse.com/index.html.

Visit http://www.nasalcleanse.com/index.php after watching our video on NasalCare nasal irrigation versus sinus sprays for sinusitis & sinus congestion relief. Learn how & why this natural sinus remedy really works! Unlike the temporary relief offered by chemical-laden nasal sprays, our patented NasalCare® Nasal Rinse System ensures comfortable and effective delivery throughout the nasal passages, preventing sinus infection, allergy and post nasal drip. A soothing mix of sea salt and Aloe Vera extract washes away nasal irritants and the common causes of colds and flu without the potential addiction that comes with nasal spray use. NasalCare also acts as a sinus wash for allergy treatment. Used for centuries in the Orient as a preventative measure for all sinus conditions, nasal irrigation is just catching on here. Catch us now and stop catching colds and the flu – the natural way! Order online at: http://www.nasalcleanse.com/index.php.
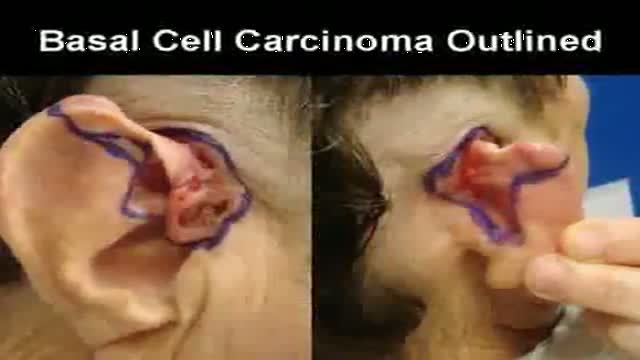
Graphic images focusing on the reconstruction of an ear after the removal of a long-standing skin cancer that this patient allowed to slowly grow over many years because he was afraid of what the surgery to remove might entail. Go to www.skincancercentre.com to learn more about the importance of the early diagnosis of skin cancer. BTW, when you put on your sunscreen, don't forget your ears, and wear a broad brimmed hat to cover this very vulnerable area of your anatomy. www.skincancercentre.com