Top videos

http://permanently-cure-your-ulcer.info-pro.co/ Symptoms Of An Ulcer, H Pylori Natural Treatment, H Pylori Treatment Natural, Diet For H Pylori. Are You Sure You Have An Ulcer? There are many symptoms that are associated with ulcers. Some ulcer sufferers only experience mild symptoms while others experience more severe. The more common symptoms of an ulcer are listed below. Abdominal discomfort is the most common symptom of an ulcer. This discomfort usually: is a dull, gnawing ache. • comes and goes for several days or weeks. • occurs 2 to 3 hours after a meal. • occurs in the middle of the night (when the stomach is empty). • is relieved by eating. • is relieved by antacid medications. Other symptoms include: • weight loss • poor appetite • bloating • burping • nausea • vomiting If you have some or all of these symptoms, it’s a good indicator that you may have an ulcer or be developing an ulcer. Discover my 100% natural cure for ulcers. click here. http://permanently-cure-your-ulcer.info-pro.co/
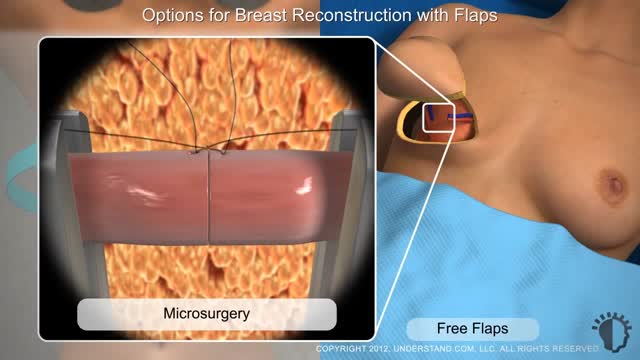
Typically, breast reconstruction takes place during or soon after mastectomy, and in some cases, lumpectomy. Breast reconstruction also can be done many months or even years after mastectomy or lumpectomy. During reconstruction, a plastic surgeon creates a breast shape using an artificial implant (implant reconstruction), a flap of tissue from another place on your body (autologous reconstruction), or both.

Pharyngitis is caused by swelling in the back of the throat (pharynx) between the tonsils and the voice box (larynx). Most sore throats are caused by colds, the flu, coxsackie virus or mono (mononucleosis). Bacteria that can cause pharyngitis in some cases: Strep throat is caused by group A streptococcus.
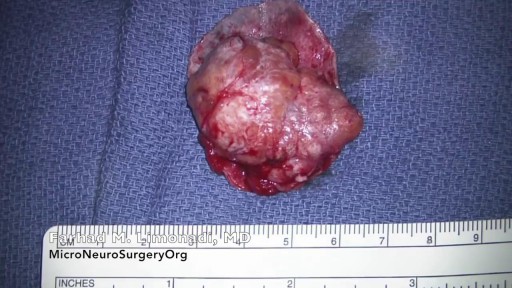
A meningioma is a tumor that arises from the meninges — the membranes that surround your brain and spinal cord. Most meningiomas are noncancerous (benign), though rarely a meningioma may be cancerous (malignant). Some meningiomas are classified as atypical, meaning they're neither benign nor malignant but, rather, something in between.
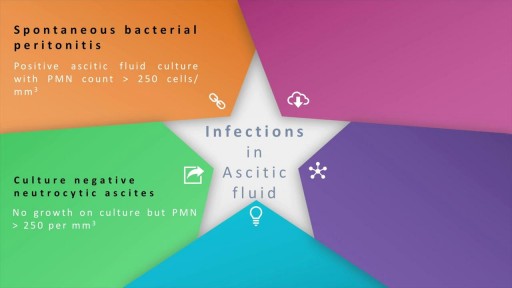
Ascites, the collection of fluid within the peritoneal space is caused due to a variety of causes including cirrhosis, cardiac causes, sinusoidal obstruction syndrome, tubercular peritonitis and pancreatitis, amongst others. Most commonly, the cause of ascots may be cirrhosis , which in turn, is most frequently causes by alcohol use, hepatitis C and non-alcoholic steatohepatitis. At the heart of the ascitic fluid analysis is the serum albumin ascitic gradient, the differential diagnosis of which has been discussed in detail in this presentation. Both low SAAG and high SAAG ascites have been dealt with in some depth, with a brief overview of the management of these conditions

When your child needs surgery, it can be overwhelming and sometimes scary. At Mayo Clinic Children’s Center, our highly skilled surgeons apply deep experience and specialized training to offer individualized care for your child and your family.

Claudication, which is defined as reproducible ischemic muscle pain, is one of the most common manifestations of peripheral arterial occlusive disease (PAOD) caused by atherosclerosis. Claudication occurs during physical activity and is relieved after a short rest. Pain develops because of inadequate blood flow. Examination of a patient with claudication should include a complete lower-extremity evaluation and pulse examination, including measuring segmental pressures. Attempt to palpate pulses from the abdominal aorta to the foot, with auscultation for bruits in the abdominal and pelvic regions. When palpable pulses are not present, a handheld Doppler device may be used to assess circulation.

A torn meniscus is one of the most common knee injuries. Any activity that causes you to forcefully twist or rotate your knee, especially when putting the pressure of your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You also might have trouble extending your knee fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and give the injury time to heal on its own. In other cases, however, a torn meniscus requires surgical repair.

Thank you so much for watching❤
If you enjoyed this video ▶Please leave a LIKE👍 ▶SHARE this video ▶【SUBSCRIBE】my channel for more new videos And click the BELL 🔔so you don't miss any of my videos HERE
https://www.youtube.com/c/nurs....eminder?sub_confirma
You can support my work by purchasing your NurseMinder Merch https://teespring.com/stores/nurseminder-nation (or click on merch pics under the video)
Or simply do your Amazon shopping after clicking on one of the links below
-------------------------------------------------------------------------
Thank you so much! I appreciate you!♥♥
------------------------------------------------------------------------
Nurses often prime IV lines with the hopes that there are no air bubbles. In this video, I will share a couple of tips to help reduce the risk or frequency of air bubbles during line priming. I will also talk about how to troubleshoot the air bubbles when they appear during an infusion
Providing patient care and influencing safe patient outcomes requires that registered nurses and licensed practice nurses maintain air free IV lines. Learn the strategies and tips to decrease the risk of air bubbles appearing in your primary or secondary medication line as well as troubleshooting tips to remove those alarming bubbles. Your patients will thank you!
Whether you are providing normal saline, a medication, or a combination, ensure that all fluids are compatible.
Supplies used in this video include the Alaris Primary Infusion line, alcohol swabs and a sterile 10 cc syringe ... and a nail in the wall :)
------------------------------------------------------------------------
❤️ ~ You may also be interested in watching ~ ❤️
PICC line assessment https://youtu.be/tnKClpU-J1g
How To Access a PICC line https://youtu.be/SCF6bmk8KWc
Putting on Sterile Gloves https://youtu.be/xNwkKLqDJn4
Organizational Plans for Nursing https://youtu.be/_NATxwPwHzc
Medication Conversions https://youtu.be/TCPBXg2TYCs
------------------------------------------------------------------------
💻COMMENT in the description box below and share your ideas
👍 LIKE the video
🗣 SHARE with your friends
📥 SUBSCRIBE ... hit the BELL 🔔
Subscribe to NurseMinder https://www.youtube.com/c/nurs....eminder?sub_confirma
------------------------------------------------------------------------
Amazon Affiliate Links
------------------------------------------------------------------------
Want to support me in another way? Enter Amazon through my links and continue to do your shopping. Simple and Easy Way to support the work I do.
The following list is the equipment I use (or if my version is no longer sold, a close replica).
📱 Phone 11 Cell Phone https://amzn.to/2WpOJfz
💻 MacBook Pro https://amzn.to/2YyxQC1
👉 Final Cut Video Editing software https://amzn.to/3fqlAd9
🎙️ Rode NT USB microphone (Audio Recording) for post-production voiceover https://amzn.to/2W2RJj1
👉 Neewer Professional Recording Stand – mount microphone and adjust positioning to keep it close but out of the camera’s view: https://amzn.to/3fjB4zs
👉 Manfrotto Tripod (hold cell phone) https://amzn.to/2YKGYUz
💡 Neewer Ring Light to reduce shadows and improve lighting. https://amzn.to/3dk5OP5
Disclaimer: I recommend only products that I know and trust to be of high quality. Links are provided for quick access. Some of the links contained in this checklist are affiliate links and I may receive a commission if make a purchase from the affiliate. This helps me to keep creating and offering free content.
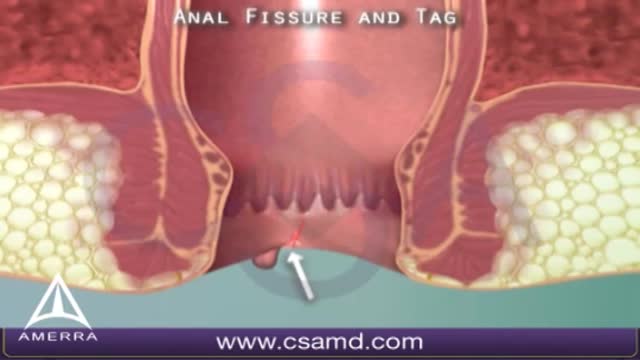
An anal fissure is a small tear in the thin, moist tissue (mucosa) that lines the anus. An anal fissure may occur when you pass hard or large stools during a bowel movement. Anal fissures typically cause pain and bleeding with bowel movements. You also may experience spasms in the ring of muscle at the end of your anus (anal sphincter). Anal fissures are very common in young infants but can affect people of any age. Most anal fissures get better with simple treatments, such as increased fiber intake or sitz baths. Some people with anal fissures may need medication or, occasionally, surgery.
How do you know if you have pneumonia? They may include: Cough. You will likely cough up mucus (sputum) from your lungs. ... Fever. Fast breathing and feeling short of breath. Shaking and "teeth-chattering" chills. Chest pain that often feels worse when you cough or breathe in. Fast heartbeat. Feeling very tired or very weak. Nausea and vomiting.

If you are tired of dealing with glasses or squinting to read signs in the distance, then you should consider LASIK Eye Surgery. In this outpatient refractive procedure, lasers are used to correct vision issues by changing the structure of the cornea. This may entirely eliminate reliance upon glasses or contacts. In this interactive LASIK Eye Surgery, you will assist in numbing the patient’s eye and cleaning the area for the procedure. With a speculum, you will hold the eye open, mark the cornea using a water-soluble ink, then attach a suction ring to it. After that, a specialized blade device is used to cut into the corneal flap and peel it back so that the laser can clear away corneal tissue underneath. This process corrects the shape of the cornea in less than a minute before putting the corneal flap back in place. After the procedure, we will go over LASIK Eye Surgery recovery instructions. Scrub in and let’s get started!

There are two main purposes of an arterial line. Firstly when patients are very sick an arterial line is inserted to provide constant monitoring and recording of the patient's blood pressure. Secondly some patients require frequent blood tests and the arterial line provides easy access to a patient's blood.