Top videos
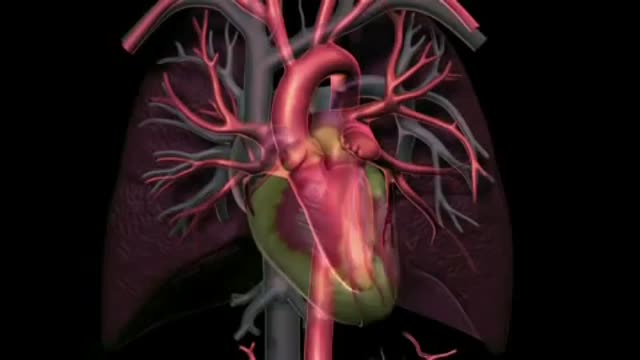
Catheter ablation is a minimally invasive procedure to treat atrial fibrillation. It can relieve symptoms and improve quality of life. During an ablation, the doctor destroys tiny areas in the heart that are firing off abnormal electrical impulses and causing atrial fibrillation. You will be given medicine to help you relax. A local anesthetic will numb the site where the catheter is inserted. Sometimes, general anesthesia is used. The procedure is done in a hospital where you can be watched carefully. Thin, flexible wires called catheters are inserted into a vein, typically in the groin or neck, and threaded up into the heart. There is an electrode at the tip of the wires. The electrode sends out radio waves that create heat. This heat destroys the heart tissue that causes atrial fibrillation or the heart tissue that keeps it happening. Another option is to use freezing cold to destroy the heart tissue. Sometimes, abnormal impulses come from inside a pulmonary vein and cause atrial fibrillation. (The pulmonary veins bring blood back from the lungs to the heart.) Catheter ablation in a pulmonary vein can block these impulses and keep atrial fibrillation from happening. View a slideshow of catheter ablation to see how the heart's electrical system works, how atrial fibrillation happens, and how ablation is done. Atrial Fibrillation: Should I Have Catheter Ablation? AV node ablation AV node ablation is a slightly different type of ablation procedure for atrial fibrillation. AV node ablation can control symptoms of atrial fibrillation in some people. It might be right for you if medicine has not worked, catheter ablation did not stop your atrial fibrillation, or you cannot have catheter ablation. With AV node ablation, the entire atrioventricular (AV) node is destroyed. After the AV node is destroyed, it can no longer send impulses to the lower chambers of the heart (ventricles). This controls atrial fibrillation symptoms. After AV node ablation, a permanent pacemaker is needed to regulate your heart rhythm. Nodal ablation can control your heart rate and reduce your symptoms, but it does not prevent or cure atrial fibrillation. AV node ablation helps about 9 out of 10 people.1 The procedure has a low risk of serious problems.2 View a slideshow of AV node ablation to see how the heart's electrical system works, how atrial fibrillation happens, and how AV node ablation is performed.

Ventricular tachycardia is a type of heart rhythm disorder (arrhythmia) in which the lower chambers of your heart (ventricles) beat very quickly because of a problem in your heart's electrical system. In ventricular tachycardia, your heart may not be able to pump enough blood to your body and lungs because the chambers are beating so fast that they don't have time to properly fill. Ventricular tachycardia may be brief — lasting for just seconds and often not causing symptoms — or it can last for much longer, and you can develop symptoms such as dizziness or lightheadedness, or you can even pass out. This condition usually occurs in people with other heart conditions, such as coronary artery disease, cardiomyopathy and some types of valvular heart disease. Ventricular tachycardia may lead to a condition in which your lower heart chambers quiver (ventricular fibrillation), which may cause your heart to stop (sudden cardiac arrest) and lead to death if not treated immediately. Ventricular tachycardia can also cause your heart to stop, especially if the heart is beating very quickly, if it's lasting for a long period, and if you have an underlying heart condition.
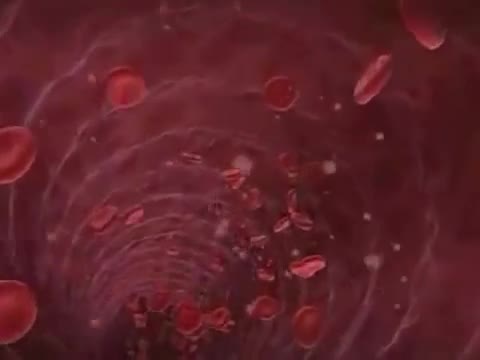
Sickle cell anemia (sickle cell disease) is a disorder of the blood caused by an inherited abnormal hemoglobin (the oxygen-carrying protein within the red blood cells). The abnormal hemoglobin causes distorted (sickled) red blood cells.
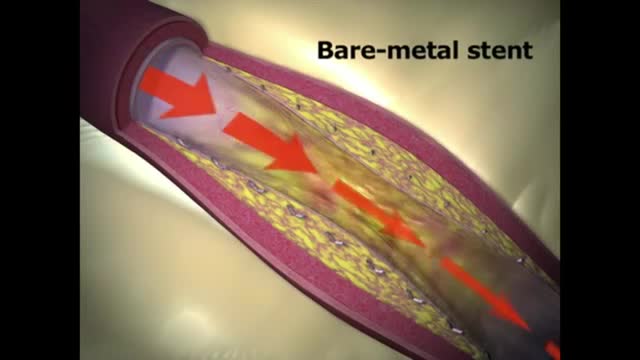
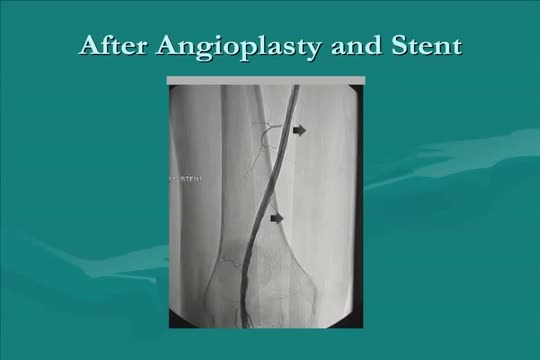
INDICATIONS The Absorb GT1 Bioresorbable Vascular Scaffold (BVS) is a temporary scaffold that will fully resorb over time and is indicated for improving coronary luminal diameter in patients with ischemic heart disease due to de novo native coronary artery lesions (length ≤ 24 mm) with a reference vessel diameter of ≥ 2.5 mm and ≤ 3.75 mm WHAT ARE THE POTENTIAL RISKS AND COMPLICATIONS? Treatment options for CAD have become increasingly common but, as with any invasive procedure, there are potential risk factors and complications. Serious complications do not occur often, and research is ongoing to make these procedures even safer and more effective. The risk of complications from percutaneous treatment methods may be higher for individuals: 75 years of age and older Who are women Who have kidney disease or diabetes Who have serious heart disease Who have had prior cardiac interventions
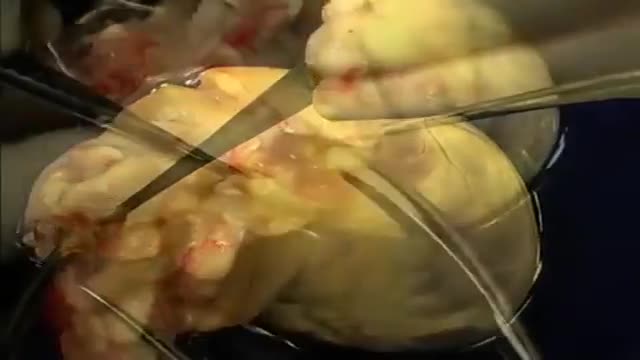
The first operation is harvesting the heart from the donor. The donor is usually an unfortunate person who has suffered irreversible brain injury, called "brain death". Very often these are patients who have had major trauma to the head, for example, in an automobile accident. The victim's organs, other than the brain, are working well with the help of medications and other "life support" that may include a respirator or other devices. A team of physicians, nurses, and technicians goes to the hospital of the donor to remove donated organs once brain death of the donor has been determined. The removed organs are transported on ice to keep them alive until they can be implanted. For the heart, this is optimally less than six hours. So, the organs are often flown by airplane or helicopter to the recipient's hospital.

Bell's palsy is a form of facial paralysis resulting from damage or trauma to the facial nerves. The facial nerve-also called the 7th cranial nerve-travels through a narrow, bony canal (called the Fallopian canal) in the skull, beneath the ear, to the muscles on each side of the face. For most of its journey, the nerve is encased in this bony shell. Each facial nerve directs the muscles on one side of the face, including those that control eye blinking and closing, and facial expressions such as smiling and frowning. Additionally, the facial nerve carries nerve impulses to the lacrimal or tear glands, the saliva glands, and the muscles of a small bone in the middle of the ear called the stapes. The facial nerve also transmits taste sensations from the tongue. When Bell's palsy occurs, the function of the facial nerve is disrupted, causing an interruption in the messages the brain sends to the facial muscles. This interruption results in facial weakness or paralysis. Bell's palsy is named for Sir Charles Bell, a 19th century Scottish surgeon who described the facial nerve and its connection to the condition. The disorder, which is not related to stroke, is the most common cause of facial paralysis. Generally, Bell's palsy affects only one of the paired facial nerves and one side of the face, however, in rare cases, it can affect both sides.

A central venous catheter, also called a central line, is a long, thin, flexible tube used to give medicines, fluids, nutrients, or blood products over a long period of time, usually several weeks or more. A catheter is often inserted in the arm or chest through the skin into a large vein.
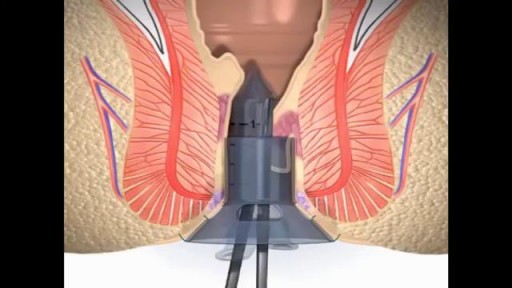
Stapling is used to treat prolapsed hemorrhoids. A surgical staple fixes the prolapsed hemorrhoid back into place inside your rectum and cuts off the blood supply so that the tissue will shrink and be reabsorbed. Stapling recovery takes less time and is less painful than recovery from a hemorrhoidectomy.
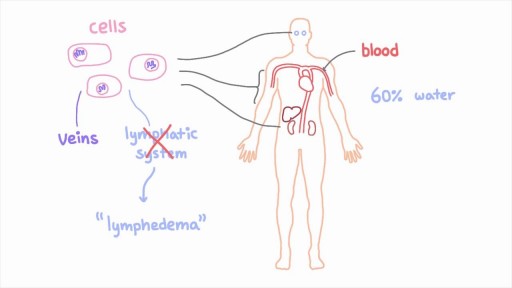
The lymphatic system is a network of specialized vessels (lymph vessels) throughout the body whose purpose is to collect excess lymph fluid with proteins, lipids, and waste products from the tissues. This fluid is then carried to the lymph nodes, which filter waste products and contain infection-fighting cells called lymphocytes. The excess fluid in the lymph vessels is eventually returned to the bloodstream. When the lymph vessels are blocked or unable to carry lymph fluid away from the tissues, localized swelling (lymphedema) is the result.

Alcoholic hepatitis can occur in people who drink heavily for many years. Symptoms include yellow skin and eyes along with increasing belly size due to fluid accumulation. Treatment involves hydration, nutritional care, and stopping alcohol use. Steroid drugs can help reduce liver inflammation.

An undescended testicle (cryptorchidism) is a testicle that hasn't moved into its proper position in the bag of skin hanging below the penis (scrotum) before birth. Usually just one testicle is affected, but about 10 percent of the time both testicles are undescended. An undescended testicle is uncommon in general, but common among baby boys born prematurely. The vast majority of the time, the undescended testicle moves into the proper position on its own, within the first few months of life. If your son has an undescended testicle that doesn't correct itself, surgery can relocate the testicle into the scrotum.
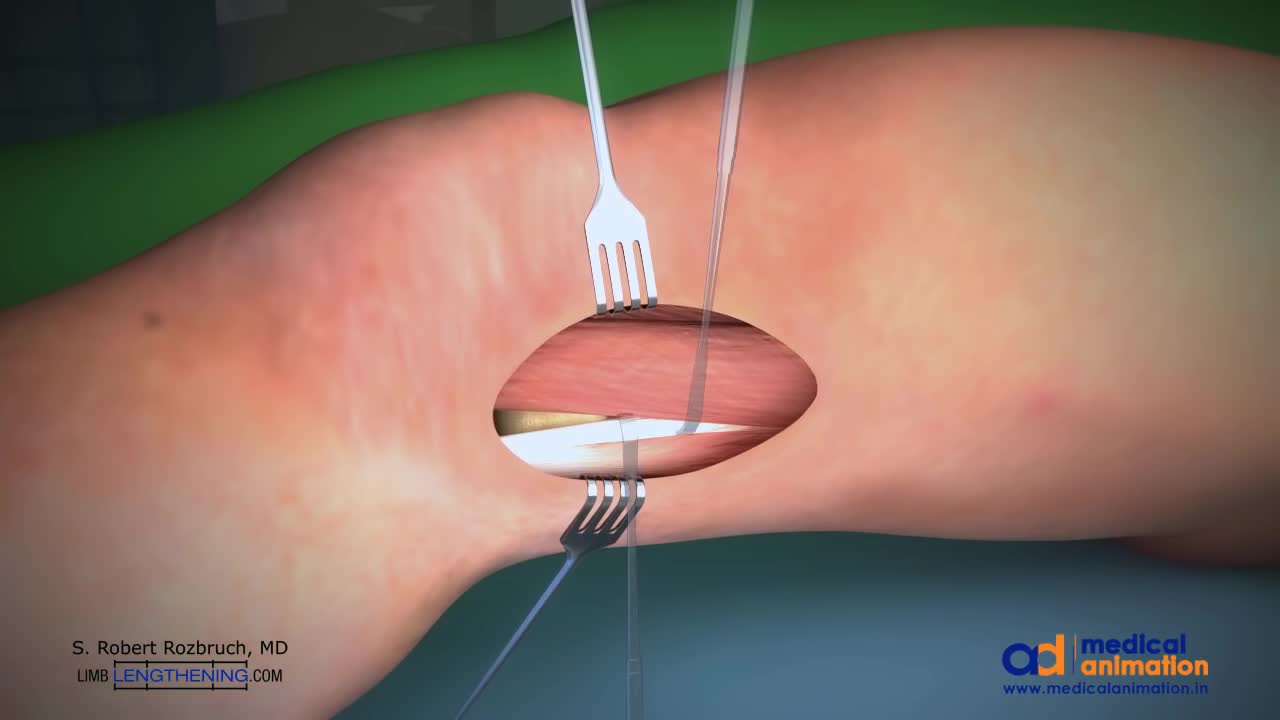
The Distal Femoral Osteotomy System utilizes the same principles of design featured in the Tibial Osteotomy System. Specifically designed femoral osteotomy plates take into account the anatomical differences between the distal femur and proximal tibia.