Top videos

A Hundred Orgasms A Day follow the story of 3 women who were tormented every hour of everyday with the need to have orgasm. This documentary explain how Persistent Sexual Arousal Syndrome or PSAS causes this unusual condition. PSAS is a little know neurological disorder where women have symptoms of continuous uncontrollable genital arousal. This condition is unrelated to any kind of sensations of sexual desire. PSAS was initially documented by Doctor Sandra Leiblum in mid 2001, just recently recognized as a unique syndrome in medical science which has a comparable equivalent progressively more claimed by men. A few physicians makes use of the name Persistent Sexual Arousal Syndrome to reference the disorder in women; some others look at the syndrome of priapism in adult males to be a similar disorder. Most importantly, it is really not connected with hyper-sexuality, also known as nymphomania. Both hyper-sexuality, and nymphomania are not known diagnosable health conditions. Not only is it very rare, the disorder is also seldom reported by affected individual who may think it is embarrassing.

If you look at someone’s back, you’ll see that the spine runs straight down the middle. When a person has scoliosis, their backbone curves to the side. The angle of the curve may be small, large or somewhere in between. But anything that measures more than 10 degrees is considered scoliosis. Doctors may use the letters “C” and “S” to describe the curve of the backbone. You probably don’t look directly at too many spines, but what you might notice about someone with scoliosis is the way they stand. They may lean a little or have shoulders or hips that look uneven. What Causes Scoliosis? In as many as 80% of cases, doctors don’t find the exact reason for a curved spine. Scoliosis without a known cause is what doctors call “idiopathic.” Some kinds of scoliosis do have clear causes. Doctors divide those curves into two types -- structural and nonstructural. In nonstructural scoliosis, the spine works normally, but looks curved. Why does this happen? There are a number of reasons, such as one leg’s being longer than the other, muscle spasms, and inflammations like appendicitis. When these problems are treated, this type of scoliosis often goes away. In structural scoliosis, the curve of the spine is rigid and can’t be reversed

Acromegaly is usually caused by a noncancerous tumor. Middle-aged adults are most commonly affected. Symptoms include enlargement of the face, hands, and feet. Prompt treatment is needed to avoid serious illness. Drugs can reduce the effects of growth hormone. If needed, surgery and radiation may be used to remove tumor cells.
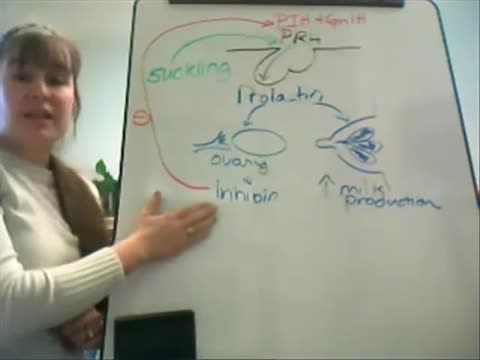
This video is designed for my introductory A&P course to study the endocrine system. This tutorial will take you through the various endocrine organs, hormones produced, and effects at each tissue. Prolactin is one of the 5 hormones we are studying of the anterior pituitary. SHOW MORE
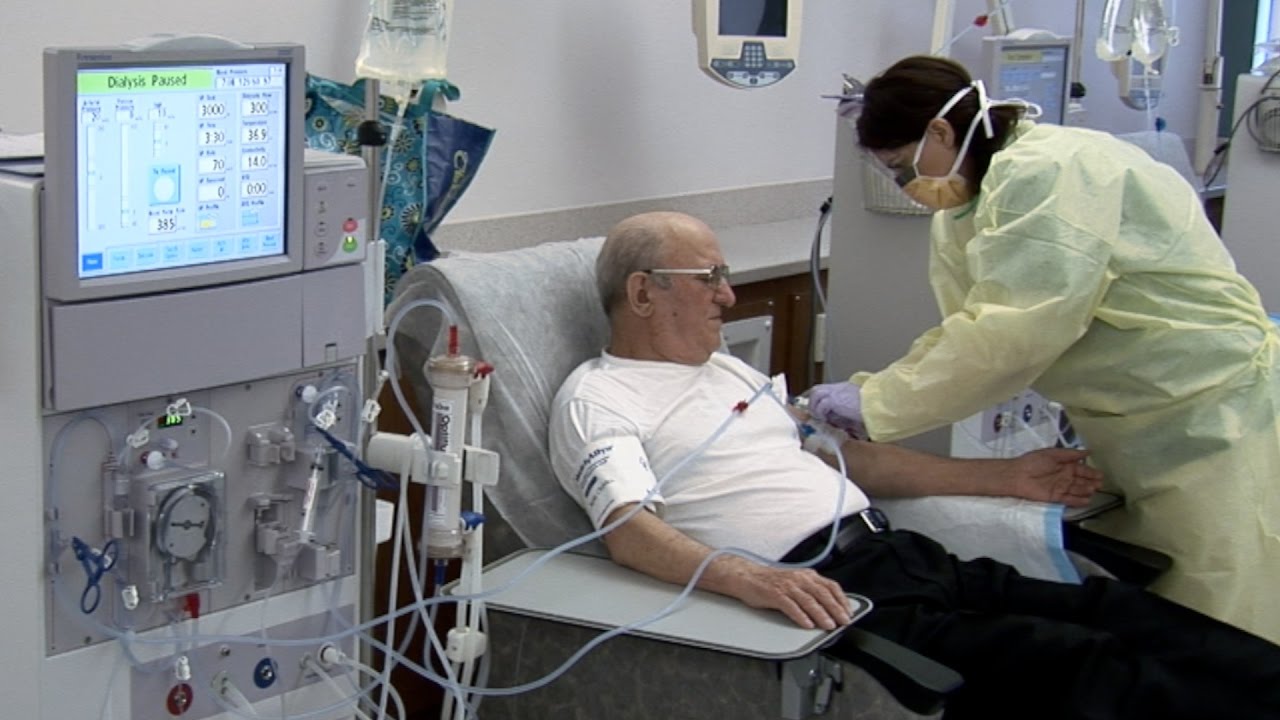
Rhode Island Hospital's outpatient dialysis program cares for patients with chronic kidney disease. Learn more about the program, which includes a new, state of the art dialysis center in East Providence. http://www.rhodeislandhospital.....org/outpatient-dial

complications from using a urinary catheter include: allergic reaction to the material used in the catheter, such as latex. bladder stones. blood in the urine. injury to the urethra. kidney damage (with long-term indwelling catheters) septicemia, or infection of the urinary tract, kidneys, or blood.

Recovery Tips
LASIK eye surgery is the best known and most commonly performed laser refractive surgery to correct vision problems. The total recovery time is 1 to 2 weeks. However, vision may fluctuate slightly over the next 2 months.
Avoid watching television or reading for the first few days.
You can get back to work after 1 week.
Avoid applying pressure on the eyes for 7 days.
Avoid dust, smoke, yard and garden work, and eye make-up.
Wear eye shields at night given by a surgeon for 1 week.
Driving is allowed after 4 to 5 days.
Avoid swimming or using a hot tub for 2 weeks after surgery.
While using the computer, take frequent breaks and lubricate your eyes with artificial tears.
For treatment assistance in your country or abroad:
Email: hello@vaidam.com
Phone/WhatsApp/Viber: +91-9650001746
Website: www.vaidam.com
Vaidam is an ISO and NABH accredited medical assistance company. Patients from 100+ countries have used our services.
Useful Links:
India
Doctors: https://www.vaidam.com/doctors/opthalmology/lasik-procedure/india
Hospitals: https://www.vaidam.com/hospitals/opthalmology/lasik-procedure/india
Cost of Lasik Eye Surgery: https://www.vaidam.com/cost/lasik-procedure-cost-in-india
Turkey
Doctors: https://www.vaidam.com/doctors/opthalmology/lasik-procedure/turkey
Hospitals: https://www.vaidam.com/hospitals/opthalmology/lasik-procedure/turkey

http://permanently-cure-your-ulcer.info-pro.co/ Symptoms Of An Ulcer, H Pylori Natural Treatment, H Pylori Treatment Natural, Diet For H Pylori. Are You Sure You Have An Ulcer? There are many symptoms that are associated with ulcers. Some ulcer sufferers only experience mild symptoms while others experience more severe. The more common symptoms of an ulcer are listed below. Abdominal discomfort is the most common symptom of an ulcer. This discomfort usually: is a dull, gnawing ache. • comes and goes for several days or weeks. • occurs 2 to 3 hours after a meal. • occurs in the middle of the night (when the stomach is empty). • is relieved by eating. • is relieved by antacid medications. Other symptoms include: • weight loss • poor appetite • bloating • burping • nausea • vomiting If you have some or all of these symptoms, it’s a good indicator that you may have an ulcer or be developing an ulcer. Discover my 100% natural cure for ulcers. click here. http://permanently-cure-your-ulcer.info-pro.co/
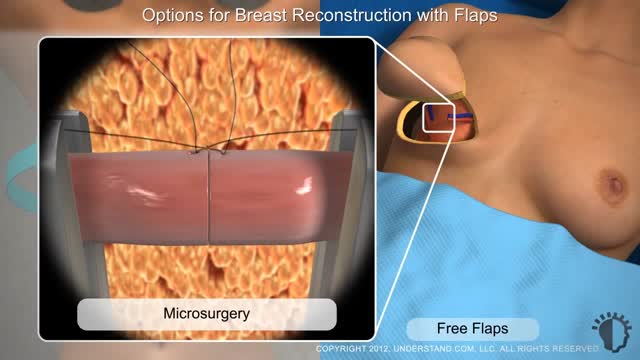
Typically, breast reconstruction takes place during or soon after mastectomy, and in some cases, lumpectomy. Breast reconstruction also can be done many months or even years after mastectomy or lumpectomy. During reconstruction, a plastic surgeon creates a breast shape using an artificial implant (implant reconstruction), a flap of tissue from another place on your body (autologous reconstruction), or both.
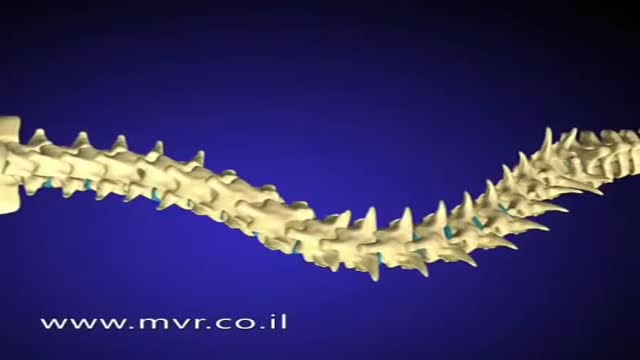
There are several approaches to scoliosis surgery, but all use modern instrumentation systems in which hooks and screws are applied to the spine to anchor long rods. The rods are then used to reduce and hold the spine while bone that is added fuses together with existing bone.
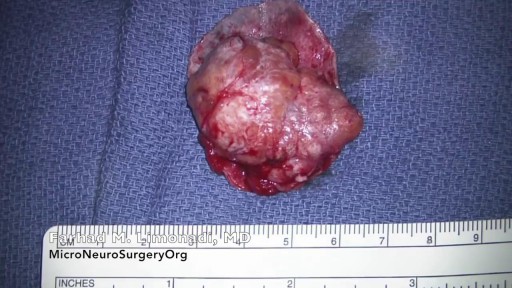
A meningioma is a tumor that arises from the meninges — the membranes that surround your brain and spinal cord. Most meningiomas are noncancerous (benign), though rarely a meningioma may be cancerous (malignant). Some meningiomas are classified as atypical, meaning they're neither benign nor malignant but, rather, something in between.
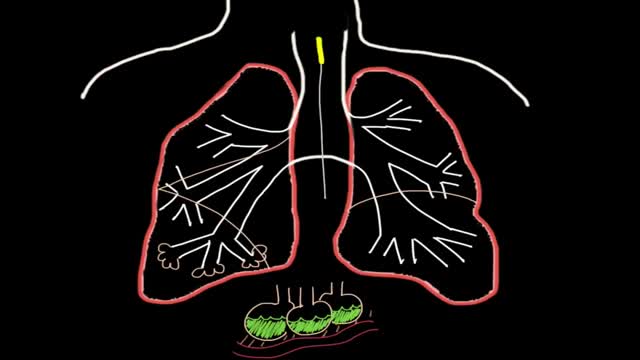
How do you know if you have pneumonia? They may include: Cough. You will likely cough up mucus (sputum) from your lungs. ... Fever. Fast breathing and feeling short of breath. Shaking and "teeth-chattering" chills. Chest pain that often feels worse when you cough or breathe in. Fast heartbeat. Feeling very tired or very weak. Nausea and vomiting.

Claudication, which is defined as reproducible ischemic muscle pain, is one of the most common manifestations of peripheral arterial occlusive disease (PAOD) caused by atherosclerosis. Claudication occurs during physical activity and is relieved after a short rest. Pain develops because of inadequate blood flow. Examination of a patient with claudication should include a complete lower-extremity evaluation and pulse examination, including measuring segmental pressures. Attempt to palpate pulses from the abdominal aorta to the foot, with auscultation for bruits in the abdominal and pelvic regions. When palpable pulses are not present, a handheld Doppler device may be used to assess circulation.

A torn meniscus is one of the most common knee injuries. Any activity that causes you to forcefully twist or rotate your knee, especially when putting the pressure of your full weight on it, can lead to a torn meniscus. Each of your knees has two menisci — C-shaped pieces of cartilage that act like a cushion between your shinbone and your thighbone. A torn meniscus causes pain, swelling and stiffness. You also might have trouble extending your knee fully. Conservative treatment — such as rest, ice and medication — is sometimes enough to relieve the pain of a torn meniscus and give the injury time to heal on its own. In other cases, however, a torn meniscus requires surgical repair.