Top videos
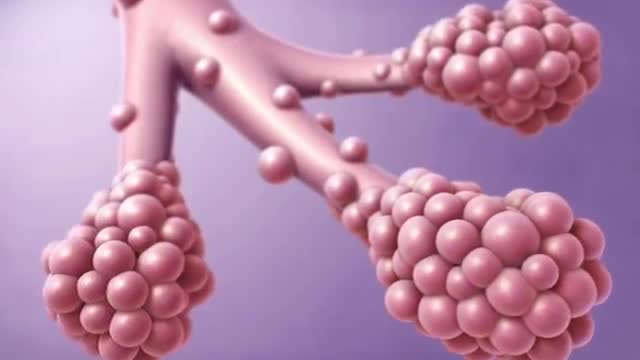
Idiopathic pulmonary fibrosis (IPF) is defined as a specific form of chronic, progressive fibrosing interstitial pneumonia of unknown cause, primarily occurring in older adults, limited to the lungs, and associated with the histopathologic and/or radiologic pattern of usual interstitial pneumonia (UIP).[1] Signs and symptoms The clinical symptoms of idiopathic pulmonary fibrosis are nonspecific and can be shared with many pulmonary and cardiac diseases. Most patients present with a gradual onset (often >6 mo) of exertional dyspnea and/or a nonproductive cough. Approximately 5% of patients have no presenting symptoms when idiopathic pulmonary fibrosis is serendipitously diagnosed.
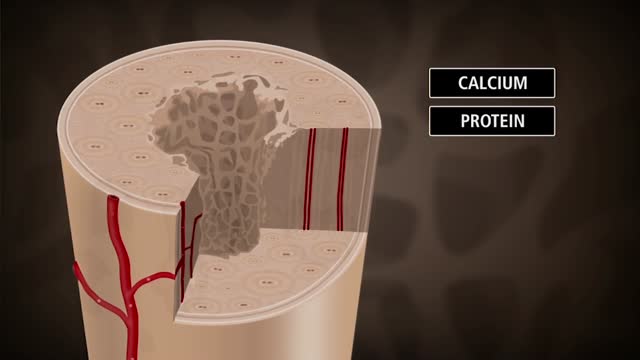
Bone is not a static part of the body — it's constantly being resorbed (broken down) and formed throughout your life. Your entire skeleton is replaced about every decade, according to the NIH. During your childhood and teenage years, bone formation occurs more quickly than bone resorption, resulting in growth. You reach your maximum bone density and strength around age 30, after which bone resorption slowly overtakes bone formation. Osteoporosis develops when there's an abnormal imbalance between bone resorption and formation — that is, resorption occurs too quickly, or formation too slowly.

Start in RLQ (so you don’t miss a giant spleen). Get your fingers set then ask patient to take a deep breath. Don’t dip your fingers or do anything but wait. When patient expires, take up new position. Note lowest point of spleen below costal margin, texture of splenic contour, and tenderness If spleen is not felt, repeat with pt lying on right side. Gravity may bring spleen within reach. “LET THE SPLEEN PALPATE YOUR FINGERS AND NOT THE OTHER WAY AROUND. THERE IS NO GOLD, SO DON’T DIG!”
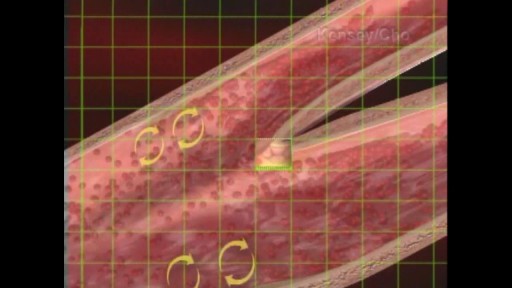
When the hematocrit rises to 60 or 70%, which it often does in polycythemia, the blood viscosity can become as great as 10 times that of water, and its flow through blood vessels is greatly retarded because of increased resistance to flow. This will lead to decreased oxygen delivery.
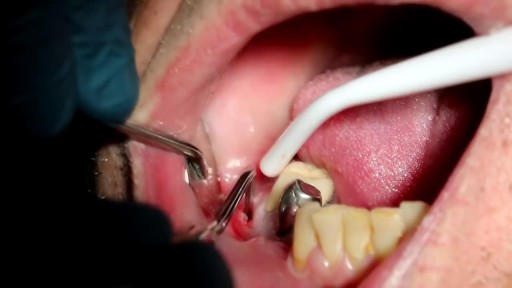
The gold standard treatment for bladder outlet obstruction.This is an endoscopic procedure in which a resectoscope is placed transurethrally and the obstructing lobes of the prostate are removed as chips of tissue. TURP results in improvement of flow rate, and symptom scores are superior to that of other minimally invasive therapies
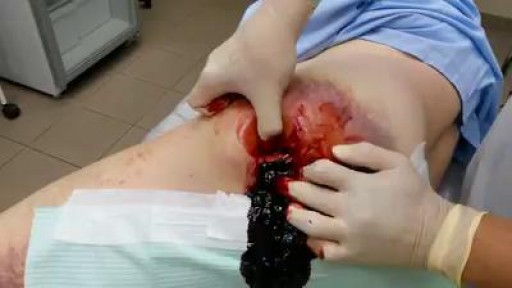
A hematoma is a collection of blood outside of a blood vessel. There are several types of hematomas and they are often described based on their location. Examples of hematomas include subdural, spinal, under the finger or toenail bed (subungual), ear, and liver (hepatic). Some causes of hematomas are as pelvic bone fractures, fingernail injuries (subungual), bumps, passing blood clots, blood clot in the leg (DVT), blood cancers, and excessive alcohol use. Symptoms of hematomas depend upon their location and whether adjacent structures are affected by the inflammation and swelling associated with the bleeding and may include
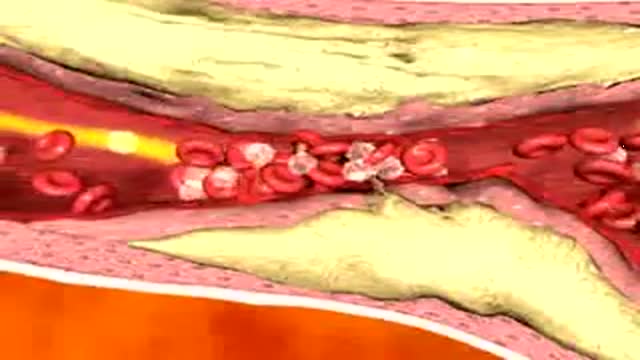
In this animation it depicts an artery with cholesterol plaque (the yellowish area) which is blocking most of the inside of this artery. Then small cells called platelets become clumped together and cause the red blood cells to form a clot. This is what causes a HEART ATTACK.
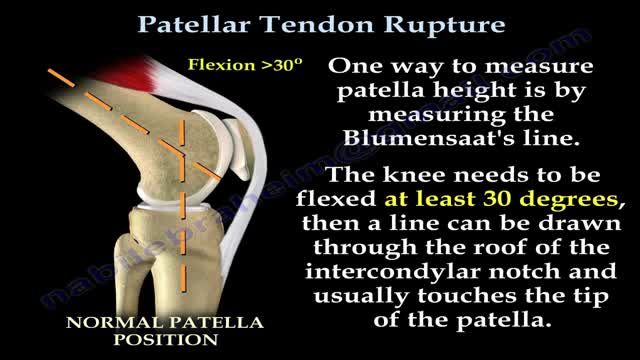
Patellar tendon rupture is a rupture of the tendon that connects the patella to the tibia. The superior portion of the patellar tendon attaches on the posterior portion of the patella, and the posterior portion of the patella tendon attaches to the tibial tubercle on the front of the tibia.
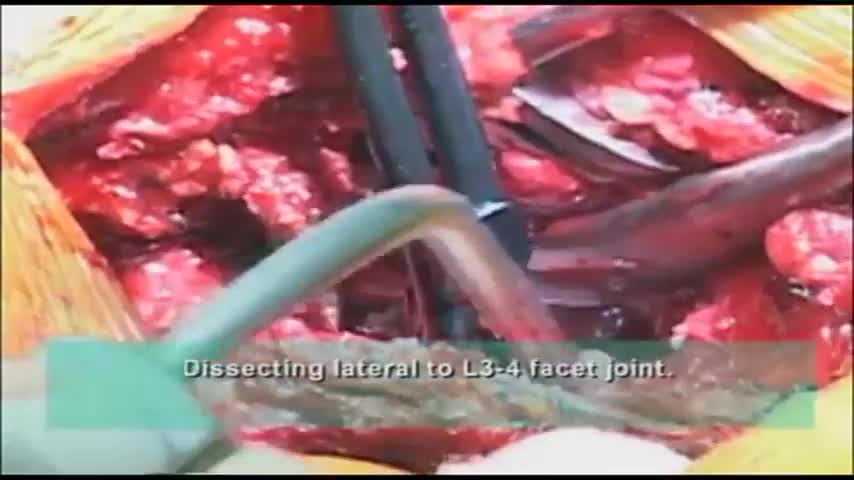
Surgeon performs a dissection of the transverse process during spine surgery, explaining the benefits of including the AQUAMANTYS System from Salient Surgical Technologies during the procedure. The AQUAMANTYS System uses Salient's patented TRANSCOLLATION technology, which has been clinically shown to reduce blood loss and lower blood transfusion rates when used during surgery.
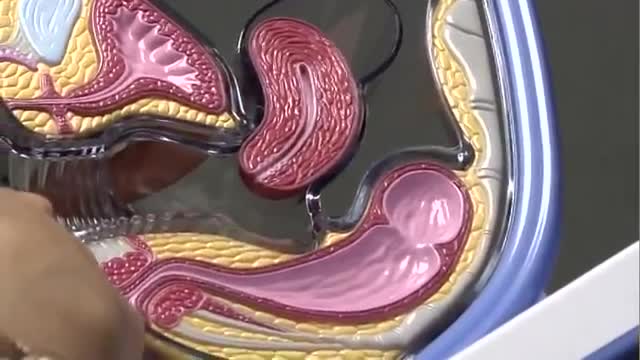
Postmenopausal bleeding (PMB) is defined for practical purposes as vaginal bleeding occurring after twelve months of amenorrhoea, in a woman of the age where the menopause can be expected.[1] Hence it does not apply to a young woman, who has had amenorrhoea from anorexia nervosa, or a pregnancy followed by lactation. However, it can apply to younger women following premature ovarian failure or premature menopause. Unscheduled bleeding in women of menopausal age taking hormone replacement therapy (HRT) should be managed in the same way from a practical perspective.[2] 'Unscheduled bleeding' is defined as non-cyclical bleeding still continuing six months after commencing HRT or after six months of amenorrhoea.
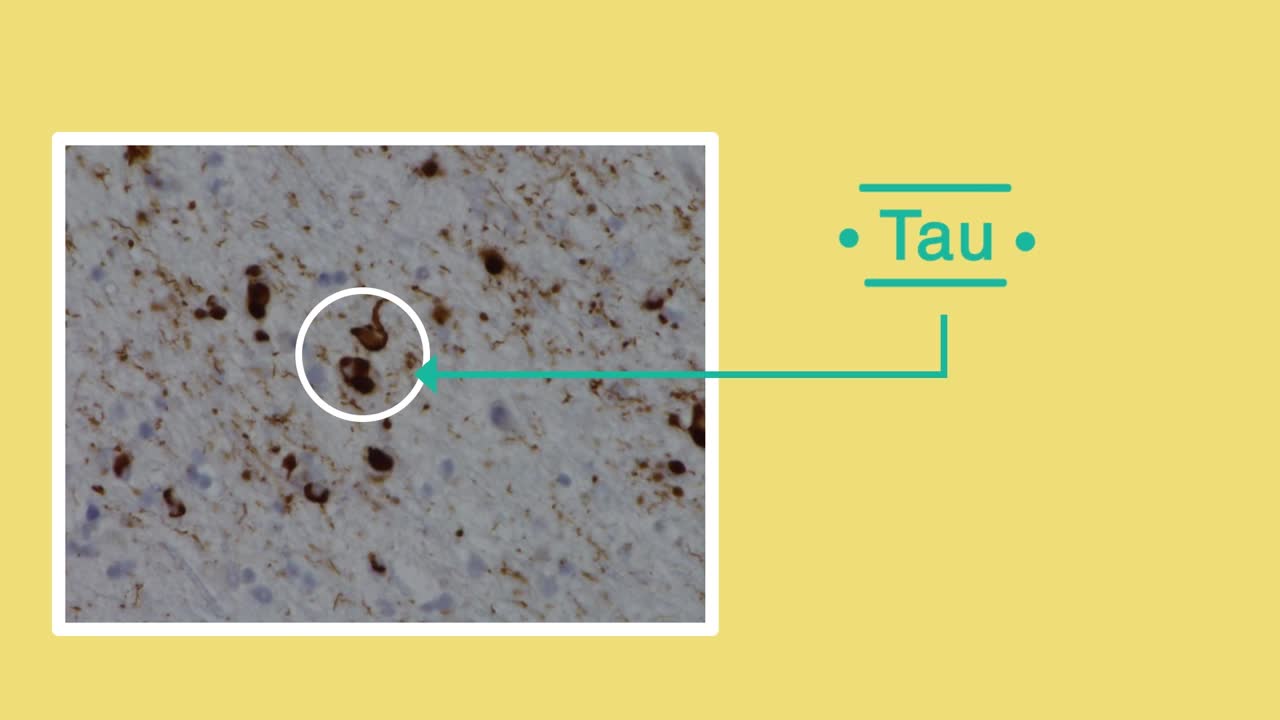
Frontotemporal dementia is the name for a range of conditions in which cells in the frontal and temporal lobes of the brain are damaged. These lobes control behaviour, emotional responses and language. This means that people will experience changes in personality and behaviour, or may struggle with language – for example, in finding the right word. Frontotemporal dementia is a less common form of dementia which is more likely to affect younger people – those under 65.
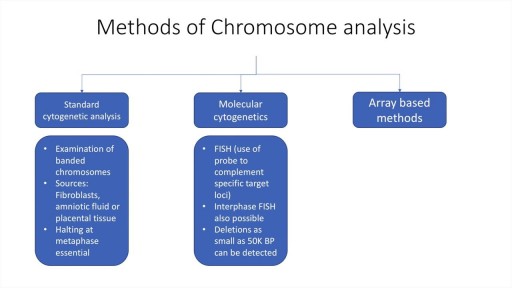
A brief description of the mechanisms, types and assessment of chromosomal analyses. Techniques such as standard cytogenetic testing, FISH and array methods are discussed. Indications for testing in prenatal, neonatal and adult periods are also discussed. Deletions, translocations, inversions etc are described, as are mosaicism and aneuploidy.