Top videos
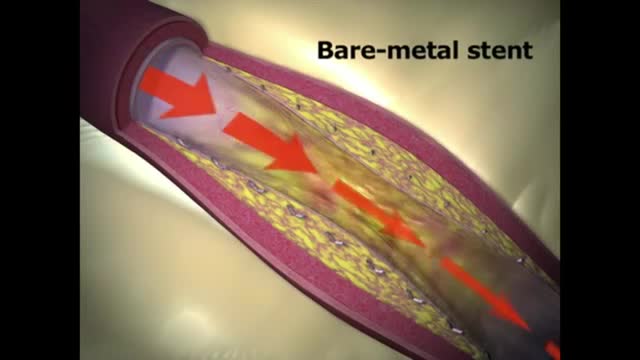
INDICATIONS The Absorb GT1 Bioresorbable Vascular Scaffold (BVS) is a temporary scaffold that will fully resorb over time and is indicated for improving coronary luminal diameter in patients with ischemic heart disease due to de novo native coronary artery lesions (length ≤ 24 mm) with a reference vessel diameter of ≥ 2.5 mm and ≤ 3.75 mm WHAT ARE THE POTENTIAL RISKS AND COMPLICATIONS? Treatment options for CAD have become increasingly common but, as with any invasive procedure, there are potential risk factors and complications. Serious complications do not occur often, and research is ongoing to make these procedures even safer and more effective. The risk of complications from percutaneous treatment methods may be higher for individuals: 75 years of age and older Who are women Who have kidney disease or diabetes Who have serious heart disease Who have had prior cardiac interventions
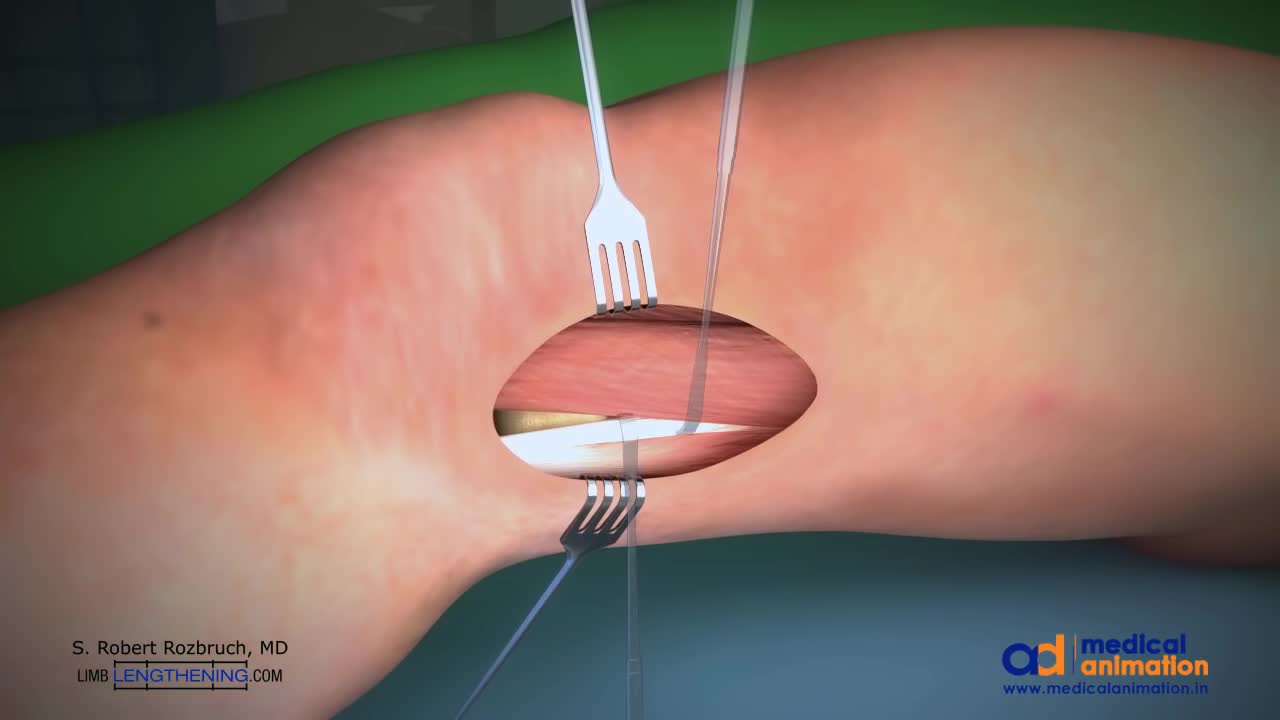
The Distal Femoral Osteotomy System utilizes the same principles of design featured in the Tibial Osteotomy System. Specifically designed femoral osteotomy plates take into account the anatomical differences between the distal femur and proximal tibia.

Bell's palsy is a form of facial paralysis resulting from damage or trauma to the facial nerves. The facial nerve-also called the 7th cranial nerve-travels through a narrow, bony canal (called the Fallopian canal) in the skull, beneath the ear, to the muscles on each side of the face. For most of its journey, the nerve is encased in this bony shell. Each facial nerve directs the muscles on one side of the face, including those that control eye blinking and closing, and facial expressions such as smiling and frowning. Additionally, the facial nerve carries nerve impulses to the lacrimal or tear glands, the saliva glands, and the muscles of a small bone in the middle of the ear called the stapes. The facial nerve also transmits taste sensations from the tongue. When Bell's palsy occurs, the function of the facial nerve is disrupted, causing an interruption in the messages the brain sends to the facial muscles. This interruption results in facial weakness or paralysis. Bell's palsy is named for Sir Charles Bell, a 19th century Scottish surgeon who described the facial nerve and its connection to the condition. The disorder, which is not related to stroke, is the most common cause of facial paralysis. Generally, Bell's palsy affects only one of the paired facial nerves and one side of the face, however, in rare cases, it can affect both sides.

A central venous catheter, also called a central line, is a long, thin, flexible tube used to give medicines, fluids, nutrients, or blood products over a long period of time, usually several weeks or more. A catheter is often inserted in the arm or chest through the skin into a large vein.

The brain is the most complex organ in our body. It controls everything we do, from simple things such as breathing, to complex things such as co-ordinating our movements. The brain stores our memories, allows us to think and speak, and controls how we behave

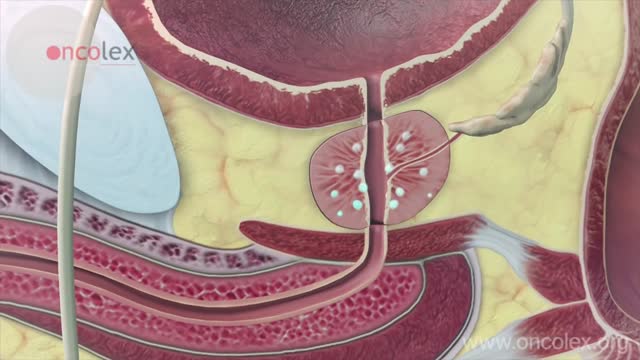
An undescended testicle (cryptorchidism) is a testicle that hasn't moved into its proper position in the bag of skin hanging below the penis (scrotum) before birth. Usually just one testicle is affected, but about 10 percent of the time both testicles are undescended. An undescended testicle is uncommon in general, but common among baby boys born prematurely. The vast majority of the time, the undescended testicle moves into the proper position on its own, within the first few months of life. If your son has an undescended testicle that doesn't correct itself, surgery can relocate the testicle into the scrotum.
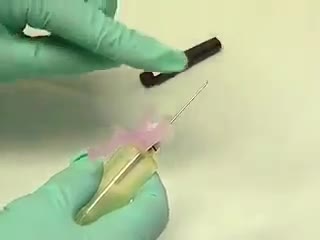
The venipuncture procedure is complex, requiring both knowledge and skill to perform. Each phlebotomist generally establishes a routine that is comfortable for her or him. Several essential steps are required for every successful collection procedure: Identify the patient. Assess the patient's physical disposition (i.e. diet, exercise, stress, basal state). Check the requisition form for requested tests, patient information, and any special requirements. Select a suitable site for venipuncture. Prepare the equipment, the patient and the puncture site. Perform the venipuncture. Collect the sample in the appropriate container. Recognize complications associated with the phlebotomy procedure. Assess the need for sample recollection and/or rejection. Label the collection tubes at the bedside or drawing area. Promptly send the specimens with the requisition to the laboratory.

Dermatomyositis (dur-muh-toe-my-uh-SY-tis) is an uncommon inflammatory disease marked by muscle weakness and a distinctive skin rash. Dermatomyositis affects adults and children alike. In adults, dermatomyositis usually occurs from the late 40s to early 60s. In children, the disease most often appears between 5 and 15 years of age. Dermatomyositis affects more females than males. There's no cure for dermatomyositis, but periods of remission — when symptoms improve spontaneously — may occur. Treatment can clear the skin rash and help you regain muscle strength and function. Symptoms ShareTweet June 17, 2014 References Products and Services Newsletter: Mayo Clinic Health Letter See also Dysphagia Electromyography Fatigue MRI Muscle pain Peptic ulcer Prednisone risks, benefits Show more Advertisement Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission. Advertising & Sponsorship PolicyOpportunitiesAd Choices Mayo Clinic Store Check out these best-sellers and special offers on books and newsletters from Mayo Clinic. NEW! – The Mayo Clinic Diet, Second Edition Treatment Strategies for Arthritis Mayo Clinic on Better Hearing and Balance Keeping your bones healthy and strong The Mayo Clinic Diet Online

The Ortolani method is an examination method that identifies a dislocated hip that can be reduced into the socket (acetabulum). Ortolani described the feeling of reduction as a “Hip Click” but the translation from Italian was interpreted a sound instead of a sensation of the hip moving over the edge of the socket when it re-located. After the age of six weeks, this sensation is rarely detectable and should not be confused with snapping that is common and can occur in stable hips when ligaments in and around the hip create clicking noises. When the Ortolani test is positive because the hip is dislocated, treatment is recommended to keep the hip in the socket until stability has been established

Norepinephrine is synthesized from dopamine by dopamine β-hydroxylase.[7] It is released from the adrenal medulla into the blood as a hormone, and is also a neurotransmitter in the central nervous system and sympathetic nervous system where it is released from noradrenergic neurons.