Top videos

Norepinephrine is synthesized from dopamine by dopamine β-hydroxylase.[7] It is released from the adrenal medulla into the blood as a hormone, and is also a neurotransmitter in the central nervous system and sympathetic nervous system where it is released from noradrenergic neurons.
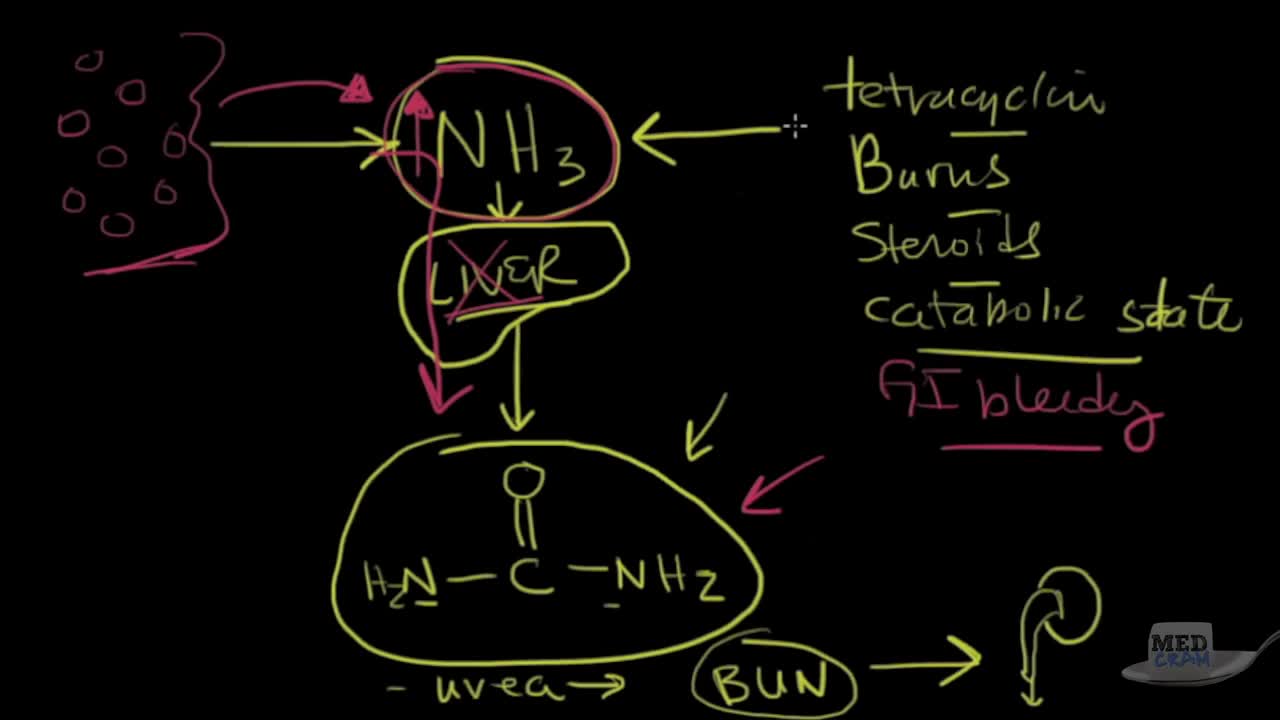
Acute kidney failure — also called acute renal failure or acute kidney injury — develops rapidly over a few hours or a few days. Acute kidney failure is most common in people who are already hospitalized, particularly in critically ill people who need intensive care. Acute kidney failure can be fatal and requires intensive treatment. However, acute kidney failure may be reversible. If you're otherwise in good health, you may recover normal or nearly normal kidney function

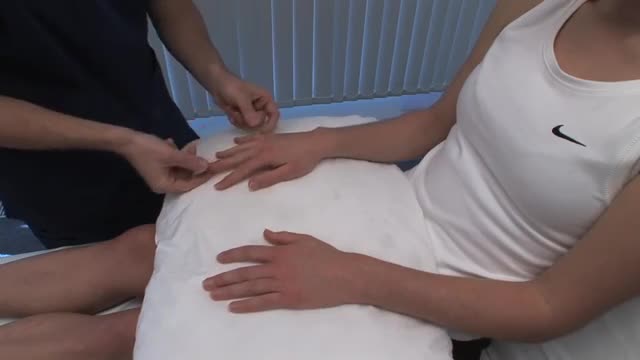
The Ortolani method is an examination method that identifies a dislocated hip that can be reduced into the socket (acetabulum). Ortolani described the feeling of reduction as a “Hip Click” but the translation from Italian was interpreted a sound instead of a sensation of the hip moving over the edge of the socket when it re-located. After the age of six weeks, this sensation is rarely detectable and should not be confused with snapping that is common and can occur in stable hips when ligaments in and around the hip create clicking noises. When the Ortolani test is positive because the hip is dislocated, treatment is recommended to keep the hip in the socket until stability has been established
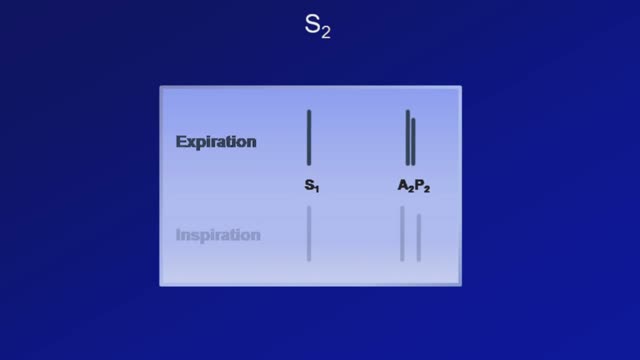
Heart sounds are the noises generated by the beating heart and the resultant flow of blood through it. Specifically, the sounds reflect the turbulence created when the heart valves snap shut. In cardiac auscultation, an examiner may use a stethoscope to listen for these unique and distinct sounds that provide important auditory data regarding the condition of the heart. In healthy adults, there are two normal heart sounds often described as a lub and a dub (or dup), that occur in sequence with each heartbeat. These are the first heart sound (S1) and second heart sound (S2), produced by the closing of the atrioventricular valves and semilunar valves, respectively. In addition to these normal sounds, a variety of other sounds may be present including heart murmurs, adventitious sounds, and gallop rhythms S3 and S4.

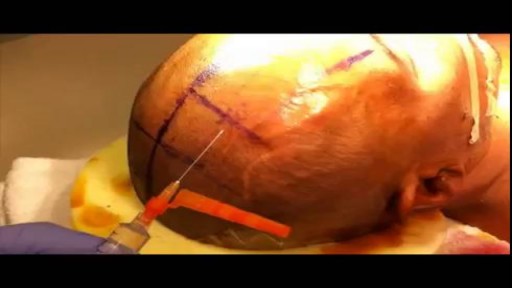
The needle should pass through the tissue at a perpendiculaPlace the tips of the left-hand forceps on the underside of the tissue at the point where the needle will enter, and gently push the edge upward. With the right hand, bring the needle into contact with the tissue, and press downward. These movements create eversion. Pass the needle through. Do not grab the tissue with your left hand forceps since it will damage the intima. If needed, you can pick up adventitia or a nearby suture to help with exposure and eversion. r.The needle must pass through the other side at a perpendicular, too. Bring the tip of the needle to the place where you intend to bring it out on the other side. Put the tip of your left-hand forceps on the upper surface of the tissue at the intended exit point. Press down with the left-hand forceps and push up with the needle to give you the correct eversion. The width of the bite should be about three times the thickness of the needle. The bites on both sides must be equal, and the needle should cross exactly in a straight line (not diagonally). Pull the needle through the tissue following the curve of the needle

The vagina is the most delicate and sensitive part of every woman’s body. Naturally female vagina appears to be darker compared to the complexion of other parts of the body. Hence, it is every woman’s dream to have a white complexioned vagina just like their body skin. Most of the women feel that using shop every day may keep their vagina clean and help to make it lighter. But reality is just the opposite. Soaps contain harsh chemicals which not only irritate the delicate skin of vagina and make it darker but they also dis-balance the ph level which plays an important role in maintaining the normal texture of the skin. Well, women need not get disappointed as now there are alternatives of harsh soaps in the market. These alternatives are none other than natural creams which are the best solution to have a naturally fair and glowing vagina without any side effects. Mentioned below are some of the best natural products available in the market to whiten vagina naturally.
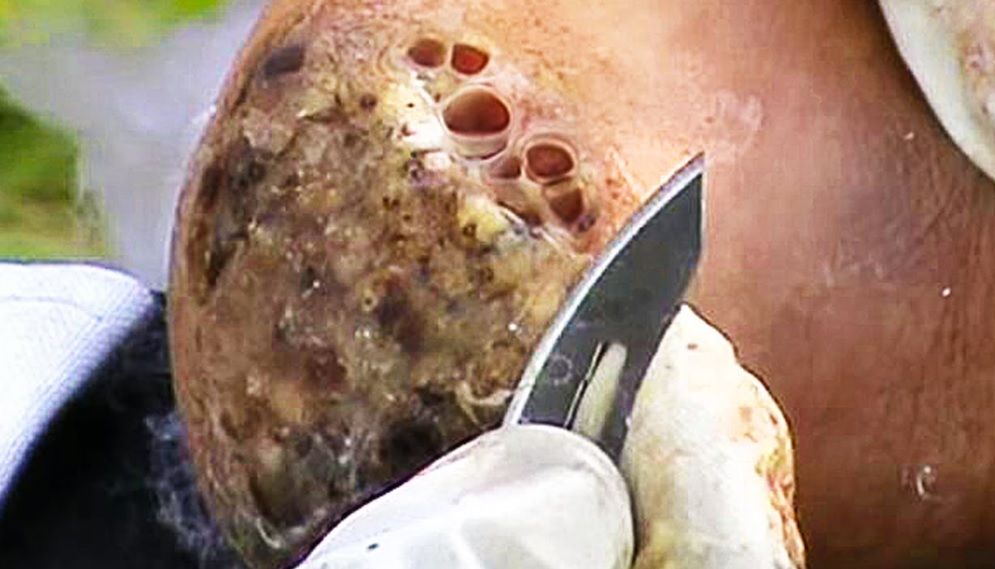
The epididymis is a long coiled tube that lies above and behind each testicle. The epididymis collects and transports sperm from the testis to the vas deferens (tubes that transport sperm to the urethra). An epididymal cyst is a cyst-like mass in the epididymis that contains clear fluid. Typically, epididymal cysts and spermatoceles do not cause symptoms. When discovered, the epididymal cyst is usually about the size of a pea and feels separate from the top of the testis. Spermatoceles typically arise from the head of the epididymis, and are felt on the top portion of the testicle. Epididymal cysts and spermatoceles are often incidental findings on testicular self-examination or routine physical examination. It is important that any mass noted in the scrotum be examined by a urologist in order to obtain an accurate diagnosis, especially a mass on the testicle itself. Our team in the Division of Urology will typically be able to confirm the diagnosis on physical exam. However, a scrotal ultrasound may also be used in order to rule out other conditions.