Top videos

26 years old man lost his right hand thumb and index fingers with an industrial machine.the thumb amputated part was not found. the thumb is much more important of any other finger in the hand and should be reconstructed by any means. so the index amputated part was filleted and replanted over the thumb stump. the video is taken 1 year after replantation. You can see another videos in my site: https://drliaghatclinic.com, https://instagram.com/liaghatclinic, https://t.me/liaghatclinic
Over one million Americans have the sexually transmitted virus, HIV, which can lead to the deadly disease known as AIDS.
HIV can be transmitted in the sexual fluids, blood or breast milk of an infected person. HIV prevention therefore involves a wide range of activities including prevention of mother-to-child transmission, needle exchanges and harm reduction for injecting drug users, and precautions for health care workers.
Laparoscopic ventral hernia repair is a technique to fix tears or openings in the abdominal wall using small incisions, laparoscopes (small telescopes inserted into the abdomen) and a patch (screen or mesh) to reinforce the abdominal wall.

Ankle and Foot Clinical Examination - Clinical Skills - Dr Gill
When it comes to joints of the body, the ankle is one of the joints most commonly injured. This is vitally important to be able to effectively examine a patient who is complaining of pain in the ankle and foot.
In this video we will perform a demonstration of the ankle and foot examination.
Examination of the foot, and the ankle joint, follows the standard orthopaedic approach of look, feel, move.
There is a connected video to the foot and ankle examination, on the causes of carpal tunnel syndrome - here
https://youtu.be/aXx6NfBWDSs
________
Please note that there is no ABSOLUTE way to perform a clinical examination. Different institutions and even clinicians will have differing degrees of variations - the aim is the effectively identify medically relevant signs.
However during OSCE assessments. Different medical schools, nursing colleges, and other health professional courses will have their own preferred approach to a clinical assessment - you should concentrate on THEIR marks schemes for your assessments.
The examination demonstrated here is derived from Macleod's Clinical Examination - a recognized standard textbook for clinical skills.
#footpain #clinicalexamination #DrGill
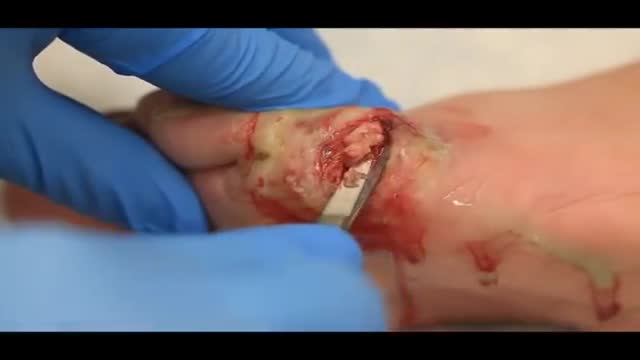
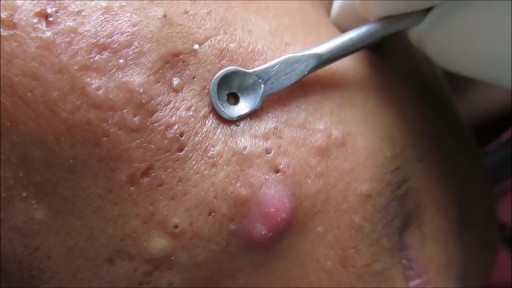
Treatment may not be needed for an eschar if it is part of the natural healing process. However, if an eschar looks like it may have a wound infection – symptoms can include oozing fluid such as pus or blood, your clinician will likely recommend topical treatment or debridement to help control and remove the infection.
Psychological counseling can help parents learn to provide an appropriate environment for the child, especially for homework completion. Psychological counseling may also help children and their families deal more effectively with the social and emotional aspects of TS. Counseling can be an important part of treatment and should not be overlooked.

The bone marrow aspiration is usually done first. The doctor makes a small incision, then inserts a hollow needle through the bone and into the bone marrow. Using a syringe attached to the needle, the doctor withdraws a sample of the liquid portion of the bone marrow. You may feel a brief sharp pain or stinging.

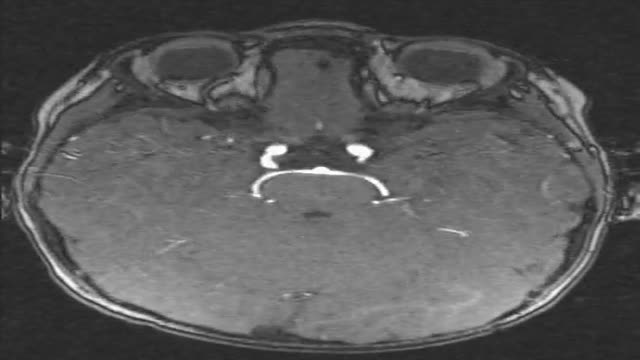
The term subarachnoid hemorrhage (SAH) refers to extravasation of blood into the subarachnoid space between the pial and arachnoid membranes. SAH constitutes half of all spontaneous atraumatic intracranial hemorrhages; the other half consists of bleeding that occurs within the brain parenchyma. Subarachnoid hemorrhage occurs in various clinical contexts, the most common being head trauma. However, the familiar use of the term SAH refers to nontraumatic (or spontaneous) hemorrhage, which usually occurs in the setting of a ruptured cerebral aneurysm or arteriovenous malformation (AVM).