Top videos

In as many as 80% of cases, doctors don’t find the exact reason for a curved spine. Scoliosis without a known cause is what doctors call “idiopathic.” Some kinds of scoliosis do have clear causes. Doctors divide those curves into two types -- structural and nonstructural. In nonstructural scoliosis, the spine works normally, but looks curved. Why does this happen? There are a number of reasons, such as one leg’s being longer than the other, muscle spasms, and inflammations like appendicitis. When these problems are treated, this type of scoliosis often goes away.

Body Restorations will do an “Early Assessment” when you come in for physiotherapy; this allows therapists to identify the more complicated cases quickly and get started with treatment right away. If you are feeling pain now, it is best that you seek treatment as soon as possible. Research has proven that people who seek treatment for their pain immediately have less of a chance of it becoming an issue later own. Early intervention is always the best option. Visit - https://stalbertphysiotherapy.com/contact/

Elizabeth Stephens, MD joined the Department of Cardiovascular Surgery at Mayo Clinic Rochester, Minnesota in 2019. To learn more about Dr. Stephens’ practice: https://www.mayoclinic.org/bio....graphies/stephens-el
Elizabeth H. Stephens, M.D., Ph.D., is an Assistant Professor of Surgery in Cardiovascular Surgery specializing in congenital cardiac surgery. She received her medical degree from Baylor College of Medicine and Ph.D in Bioengineering from Rice University focusing on tissue engineering heart valves. Her adult cardiothoracic training was completed at Columbia University and congenital training at Lurie Children's Hospital in Chicago. Her clinical areas of expertise include the treatment of:
• Neonates, infants, and children with complex congenital heart disease
• Adult patients with congenital heart disease, including patients previously repaired
• Valve disease, including Ebstein's anomaly
• Pediatric patients with heart failure, including mechanical circulatory support and heart transplantation
• Patients with vascular rings and tracheal stenosis
In addition to her clinical areas of expertise, Dr. Stephens is active in outcomes research relative to congenital heart disease and is extensively published on various cardiac surgery conditions. She has a particular interest in education, including serving on national committees and mentoring trainees of all levels.

Breast Cancer spreads by 3 mechanisms- local spread, by lymph nodes, or through the blood. Dr. Lorraine Champion, and Dr. Lisa Bailey discuss how breast cancer spreads. They discuss the different methods of spread and how this will affect the treatment of breast cancer.

Healthcare providers are in the best position to assess for domestic violence, yet have obstacles to doing so. See the benefits to moving beyond these obstacles for those you serve. And discover an accurate, convenient and confidential way to assess for domestic abuse.
Septic arthritis is also known as infectious arthritis, and is usually caused by bacteria, or fungus. The condition is an inflammation of a joint that's caused by infection. Typically, septic arthritis affects one large joint in the body, such as the knee or hip. Less frequently, septic arthritis can affect multiple joints
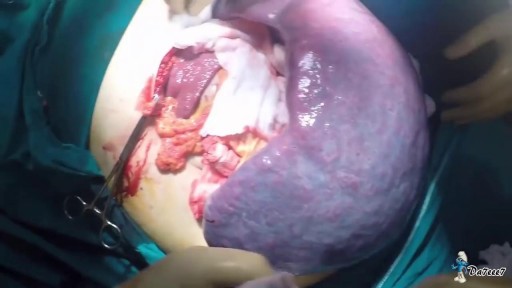
The spleen is one of the most frequently injured intraperitoneal organs, and management of splenic injuries may require splenectomy .. The spleen is an wedge-shaped organ that lies in relation to the ninth and 11th ribs, located in the left hypochondrium and partly in the epigastrium; thus, it is situated between the fundus of the stomach and the diaphragm. The spleen is highly vascular and reddish purple; its size and weight are variable. A normal spleen is not palpable. The spleen's key function is the removal of old red blood cells "RBCs", defective circulating cells, and circulating bacteria. In addition, the spleen helps maintain normal erythrocyte morphology by processing immature erythrocytes, removing their nuclei, and changing the shape of the cellular membrane. Other functions of the spleen include the removal of nuclear remnants of RBCs, denatured hemoglobin, and iron granules ..

Dr. Erica Hodgman discusses pediatric surgery at the Johns Hopkins Children's Center Pediatric General Surgery program, what common surgeries the program specializes in, what makes the program unique and her work as a pediatric surgeon. #PediatricSurgery #JohnsHopkinsChildrenCenter
Questions Answered:
0:03 Describe the pediatric general surgery division at Johns Hopkins Children's Center.
1:00 What makes this program unique?
1:31 What are some common pediatric surgery cases?
2:23 Explain your work as a pediatric general surgeon?

Leading cardiologists Valentin Fuster, MD, PhD, Director of Mount Sinai Heart and Herschel Sklaroff, MD, Clinical Professor of Medicine, Cardiology at Mount Sinai Heart were filmed for one-month for the “Making Rounds” documentary film as they cared for critically-ill heart patients in the Cardiac Care Unit at The Mount Sinai Hospital.
Watch Mount Sinai Heart doctors, fellows, residents, and nurses in action and saving lives demonstrating how simply listening to patients at the bedside remains medicine’s most indispensable tool over any technology.
In this film Mount Sinai Heart helps preserve the disappearing art and science of how to examine and diagnose patients at the bedside for future generations of physicians.
**This film was made possible by the generous support
of the McInerney Family.**
Copyright 2015 Middlemarch Films, Inc
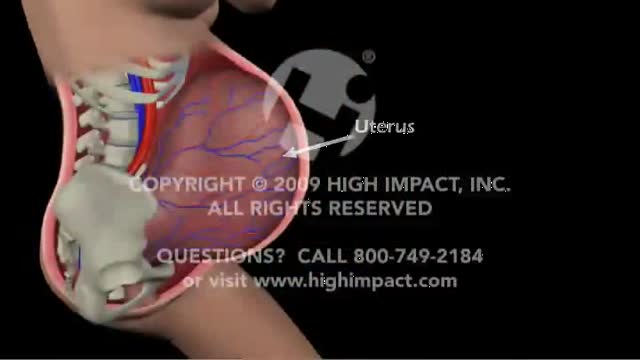
The fetal circulation is the circulatory system of a human fetus, often encompassing the entire fetoplacental circulation that also includes the umbilical cord and the blood vessels within the placenta that carry fetal blood.
The fetal circulation works differently from that of born humans, mainly because the lungs are not in use: the fetus obtains oxygen and nutrients from the mother through the placenta and the umbilical cord.

Aortoiliac occlusive disease (AIOD) occurs commonly in patients with PAD. Significant lesions in the aortoiliac arterial segment are exposed easily by palpation of the femoral pulses. Any diminution of the palpable femoral pulse indicates that a more proximal obstruction exists. Obstructive lesions may be present in the infrarenal aorta, common iliac, internal iliac (hypogastric), external iliac, or combinations of any or all of these vessels. Occasionally, degenerated nonstenotic atheromatous disease exists in these vessels and may manifest by atheroembolism to the foot, the "blue toe" or "trash foot" syndrome. Generally, patients with aortoiliac PAD have a poorer general prognosis than those with more distal PAD.