- Physical Examination
- Surgical Examination
- Ophthalmology
- Clinical Skills
- Orthopedics
- Surgery Videos
- Laparoscopy
- Pediatrics
- Funny Videos
- Cardiothoracic Surgery
- Nursing Videos
- Plastic Surgery
- Otorhinolaryngology
- Histology and Histopathology
- Neurosurgery
- Dermatology
- Pediatric Surgery
- Urology
- Dentistry
- Oncology and Cancers
- Anatomy Videos
- Health and Fitness
- Radiology
- Anaesthesia
- Physical Therapy
- Pharmacology
- Interventional Radiology
- Cardiology
- Endocrinology
- Gynecology
- Emergency Medicine
- Psychiatry and Psychology
- Childbirth Videos
- General Medical Videos
- Nephrology
- Physiology
- Diet and Food Health
- Diabetes Mellitus
- Neurology
- Women Health
- Osteoporosis
- Gastroenterology
- Pulmonology
- Hematology
- Rheumatology
- Toxicology
- Nuclear Medicine
- Infectious Diseases
- Vascular Disease
- Reproductive Health
- Burns and Wound Healing
- Other
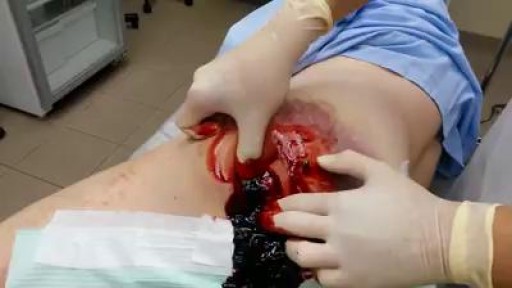
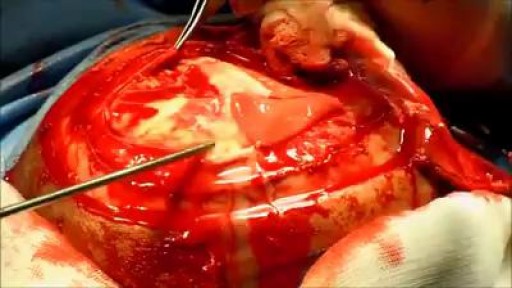
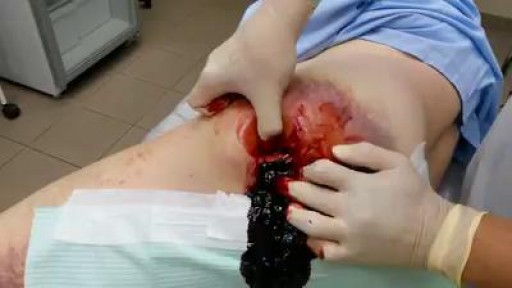
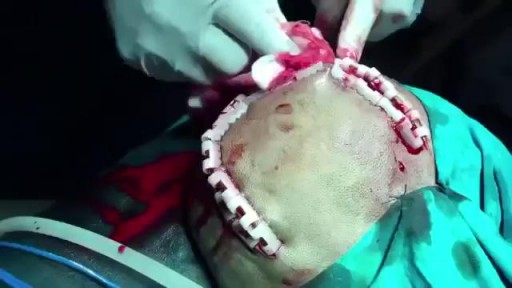
Traumatic Acute Subdural Hematoma
A subdural hematoma (SDH) is a collection of blood below the inner layer of the dura but external to the brain and arachnoid membrane (see the images below). Subdural hematoma is the most common type of traumatic intracranial mass lesion. Subdural hematoma occurs not only in patients with severe head injury but also in patients with less severe head injuries, particularly those who are elderly or who are receiving anticoagulants. Subdural hematoma may also be spontaneous or caused by a procedure, such as a lumbar puncture (see Etiology). Rates of mortality and morbidity can be high, even with the best medical and neurosurgical care (see Prognosis). Subdural hematomas are usually characterized on the basis of their size and location and the amount of time elapsed since the inciting event age (ie, whether they are acute, subacute, or chronic). When the inciting event is unknown, the appearance of the hematoma on neuroimaging studies can help determine when the hematoma occurred. These factors, as well as the neurologic and medical condition of the patient, determine the course of treatment and may also influence the outcome. Generally, acute subdural hematomas are less than 72 hours old and are hyperdense compared with the brain on computed tomography scans. The subacute phase begins 3-7 days after acute injury. Chronic subdural hematomas develop over the course of weeks and are hypodense compared with the brain. However, subdural hematomas may be mixed in nature, such as when acute bleeding has occurred into a chronic subdural hematoma. Presentation varies widely in acute subdural hematoma (see Clinical). Many of these patients are comatose on admission. However, approximately 50% of patients with head injuries who require emergency neurosurgery present with head injuries that are classified as moderate or mild (Glasgow Coma Scale scores 9-13 and 14-15, respectively). Many of these patients harbor intracranial mass lesions. In a large series of patients who developed intracranial hematomas requiring emergent decompression, more than half had lucid intervals and were able to make conversation between the time of their injury and subsequent deterioration. In a more comprehensive review of the literature on the surgical treatment of acute subdural hematomas, lucid intervals were noted in up to 38% of cases. These patients may be more likely to benefit from medical and surgical intervention when instituted in a timely fashion (ie, before further neurological deterioration).